Hospice Care - Defining Dignity
- Aim: Enhance QoL & dignity in terminal illness.
- Prognosis: Typically ≤ 6 months.
- Location: Home, hospice, hospital, nursing facility.
- Services: Pain/symptom control, psychosocial & spiritual support.
- Team: Interdisciplinary (MDs, nurses, SWs, counselors, volunteers).
- Philosophy: Care, not cure; dying as a normal process.

⭐ Hospice care prioritizes quality of life and comfort for individuals with life-limiting illnesses when curative treatment is no longer an option or desired.
Hospice Care - Entry Pass Grace
- Focus: Comfort, quality of life, not curative treatment.
- Eligibility: Terminal illness with life expectancy ≤ 6 months.
- Certified by two physicians (typically).
- Patient chooses hospice care (informed consent).
- Forgoes curative treatments for the terminal illness.
⭐ A key eligibility criterion for hospice care is a physician-certified prognosis of 6 months or less if the disease follows its natural course.
Hospice Care - Comfort Care Circle
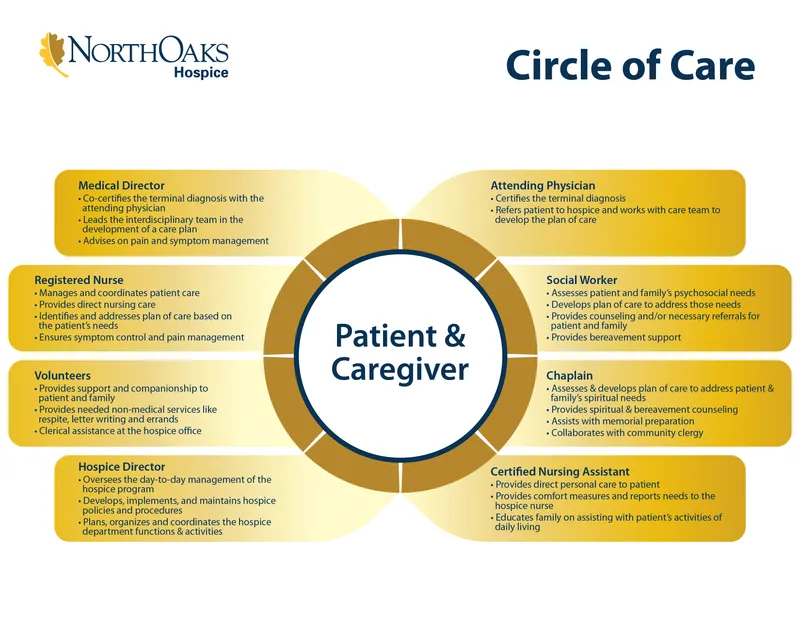
- Core Aim: Enhance quality of life, provide comfort, and uphold dignity for individuals with terminal illness.
- Multidisciplinary Team Services:
- Medical: Expert pain and symptom management.
- Nursing: Skilled, compassionate care.
- Psychosocial: Counseling for patient and family.
- Spiritual: Support tailored to beliefs.
- Bereavement: Grief support for family post-loss.
⭐ Hospice services include comprehensive medical care, nursing support, psychosocial counseling, spiritual care, and bereavement support for the family for up to 1 year.
Hospice Care - Angels on Call
- Philosophy: Comfort and quality of life for terminally ill patients (prognosis typically ≤ 6 months).
- Goal: Symptom control (e.g., pain, dyspnea), not cure.
- Services: Comprehensive support - medical, emotional, spiritual, social.
- Bereavement care for family is a key component.
- Setting: Home, dedicated facilities, hospitals, nursing homes.
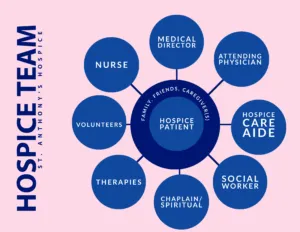
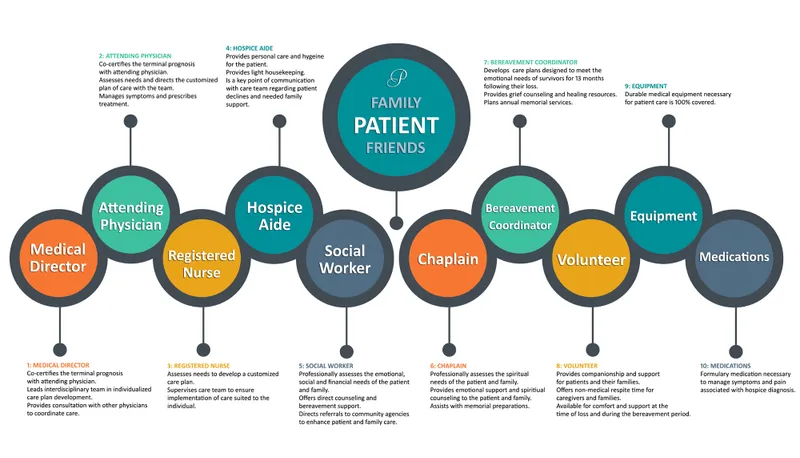
⭐ The hospice interdisciplinary group (IDG), including physicians, nurses, social workers, and counselors, collaboratively develops and reviews the patient's care plan.
Hospice Care - Easing Final Steps
- Goal: Maximize comfort & quality of life for terminally ill (prognosis < 6 months).
- Approach: Holistic care for physical, emotional, psychosocial, spiritual needs of patients & families.
- Core Services: Expert pain/symptom management, counseling, spiritual support, bereavement services.
- Team: Interdisciplinary: physicians, nurses, social workers, chaplains, volunteers.
⭐ Morphine is the WHO-recommended strong opioid for managing moderate to severe pain in hospice patients, with dose titrated to effect.
Hospice Care - Rightful Release Rules
- Focus: Quality of life, symptom relief.
- Eligibility: Terminal illness (prognosis < 6 months).
- Legal (India):
- Active euthanasia: Illegal.
- Passive euthanasia: Permitted (Supreme Court).
- Withdrawal of life support allowed.
- Requires consent/advance directives.
- Principle: Patient autonomy, dignity.
⭐ In India, while active euthanasia is illegal, the Supreme Court has recognized the 'right to die with dignity' and permitted passive euthanasia, including withdrawal of life support, aligning with hospice principles under strict guidelines.
High‑Yield Points - ⚡ Biggest Takeaways
- Eligibility: Terminal illness, prognosis ≤ 6 months, physician certified.
- Focus: Comfort care and symptom control (especially pain), not cure.
- Team: Multidisciplinary (MD, nurse, social worker, spiritual support).
- Opioids: No ceiling dose for pain; titrate to effect for optimal relief.
- Bereavement Support: Provided to family for up to 1 year post-death.
- Hospice vs Palliative: Hospice is for terminal phase; palliative care can start anytime, with/without curative intent.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

