PN Basics - Nerve Nuisance Intro
- Peripheral Neuropathy (PN): Disorder of peripheral nerves (motor, sensory, autonomic).
- Classification (Distribution):
- Mononeuropathy: Single nerve (e.g., Carpal Tunnel).
- Mononeuritis Multiplex: ≥2 separate nerves (e.g., Vasculitis).
- Polyneuropathy: Symmetrical, distal (e.g., Diabetic).
- Classification (Pathology):
- Axonal:
- Primary axon damage.
- ↓CMAP/SNAP amplitude.
- NCV normal/mildly ↓.
- Demyelinating:
- Primary myelin damage.
- ↓NCV, ↑distal latencies.
- Conduction block common.
- Axonal:
- Pathophysiology:
- Wallerian Degeneration: Axon breakdown distal to injury.
- Segmental Demyelination: Focal myelin loss.
- Neuronopathy: Nerve cell body (soma) damage.
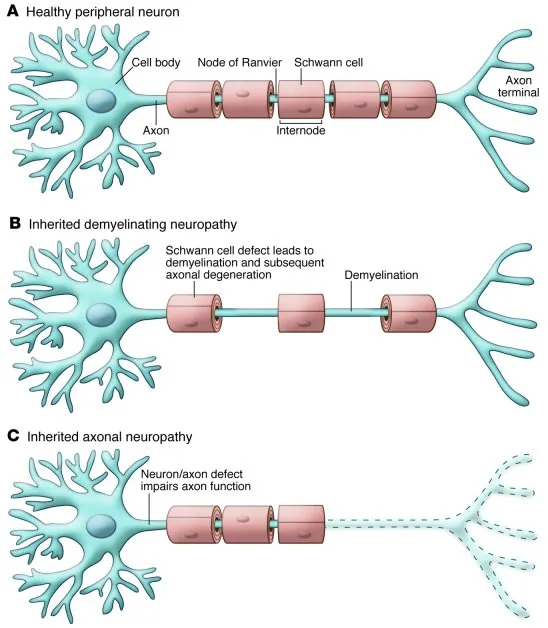
⭐ Demyelinating neuropathies primarily slow conduction velocity (CV) & prolong distal latencies. Axonal neuropathies reduce SNAP/CMAP amplitude.
Causes & Clues - The Why & How
- Metabolic:
- Diabetes Mellitus (DM): Most common; length-dependent.
- Uremia (CKD).
- Immune-Mediated:
- Guillain-Barré Syndrome (GBS): Acute, ascending.
- Vasculitis: Mononeuritis multiplex.
- Paraneoplastic syndromes.
- Infectious:
- Leprosy: Affects cool areas.
- HIV: Distal symmetric.
- Lyme disease: Cranial nerves, radiculopathy.
- Diphtheria: Exotoxin.
- Hereditary:
- Charcot-Marie-Tooth (CMT): Distal weakness/atrophy.
- Toxic:
- Alcohol.
- Lead: Wrist/foot drop.
- Drugs: Vincristine, Isoniazid (INH).
- Nutritional:
- Deficiency: Vit B12, B1, B6, E.
- Excess: Vit B6 (sensory).
- Other:
- Amyloidosis: Protein infiltration.
⭐ Diabetes mellitus is the leading cause of peripheral neuropathy in developed countries, typically presenting as a length-dependent sensorimotor polyneuropathy.
Signs & Sleuthing - Spotting the Damage
- Clinical Features:
- Sensory:
- Negative: Numbness, ↓proprioception, ataxia.
- Positive: Paraesthesia, dysesthesia, allodynia, neuropathic pain.
- Motor: Weakness (distal > proximal), atrophy, fasciculations, cramps, ↓/absent reflexes.
- Autonomic: Orthostatic hypotension, gastroparesis, bowel/bladder/sweating issues, erectile dysfunction.
- Sensory:
- Patterns:
- Stocking-glove, length-dependent.
- Mononeuropathy, Mononeuritis multiplex, Radiculopathy.

- Diagnosis:
- History & Neuro Exam: Sensory, motor, reflexes, gait.
- Electrodiagnosis:
- NCS: ↓Velocity, ↓amplitude, ↑latency, conduction block.
- EMG: Fibrillations, positive sharp waves, MUP changes.
- Nerve Biopsy Indications: Vasculitis, amyloidosis, CIDP, leprosy.
⭐ NCS differentiates axonal (↓amplitude) vs. demyelinating (↓velocity, ↑latency, conduction block) neuropathies, guiding investigation.
Key Syndromes - Neuropathy Notables
- Guillain-Barré Syndrome (GBS): Acute inflammatory demyelinating polyradiculoneuropathy (AIDP). Ascending paralysis, areflexia. 📌 GBS: Ground to Brain Syndrome. CSF: Albuminocytologic dissociation. Rx: IVIG/Plasmapheresis.
- Diabetic Neuropathy: Distal Symmetric Polyneuropathy (DSPN) "stocking-glove"; autonomic (gastroparesis); focal (CN III palsy). Rx: Glycemic control, pain relief.
- Charcot-Marie-Tooth (CMT): Hereditary Motor & Sensory Neuropathy (HMSN). Pes cavus, distal muscle wasting ("stork legs"). Biopsy (CMT1A): "Onion bulb".
- Bell's Palsy: Idiopathic CN VII palsy. Acute unilateral facial weakness (upper/lower face). Rx: Corticosteroids +/- antivirals.
- Carpal Tunnel Syndrome (CTS): Median nerve entrapment at wrist. Pain/paresthesia (thumb, index, middle fingers). Tinel's/Phalen's signs. Rx: Splinting, steroids, surgery.
⭐ Albuminocytologic dissociation (elevated CSF protein with normal or minimally increased white blood cell count) is a hallmark finding in Guillain-Barré Syndrome, typically seen after the first week.
High‑Yield Points - ⚡ Biggest Takeaways
- Guillain-Barré Syndrome (GBS): Ascending paralysis, areflexia, albuminocytologic dissociation in CSF.
- Charcot-Marie-Tooth (CMT): Most common hereditary neuropathy; pes cavus, distal muscle atrophy.
- Diabetic Neuropathy: Most common cause; stocking-glove sensory loss, autonomic dysfunction.
- Bell's Palsy: Unilateral LMN facial nerve (CN VII) palsy; sudden onset, good prognosis.
- Carpal Tunnel Syndrome: Median nerve compression at wrist; Phalen's/Tinel's positive, nocturnal symptoms.
- Vitamin B12 Deficiency: Subacute combined degeneration; dorsal columns, corticospinal tracts, peripheral neuropathy.
- Leprosy (Hansen's Disease): Mononeuritis multiplex, anesthetic skin patches, thickened nerves.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

