NMJ Fundamentals - Synaptic Spark
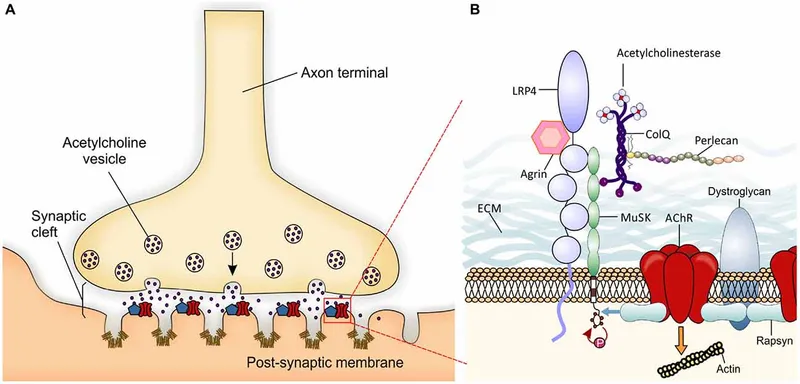
- NMJ: Specialized chemical synapse; motor neuron axon terminal connects to muscle fiber's motor end plate.
- Key Components:
- Presynaptic Terminal: Stores acetylcholine (ACh) in vesicles; site of voltage-gated Ca2+ channels.
- Synaptic Cleft: Contains acetylcholinesterase (AChE) for ACh breakdown.
- Postsynaptic Membrane (Motor End Plate): Rich in nicotinic ACh receptors (nAChR); has junctional folds.
- Transmission Steps:
⭐ Voltage-gated Ca2+ channels at the presynaptic terminal are crucial for ACh release.
Myasthenia Gravis - Receptor Wreck
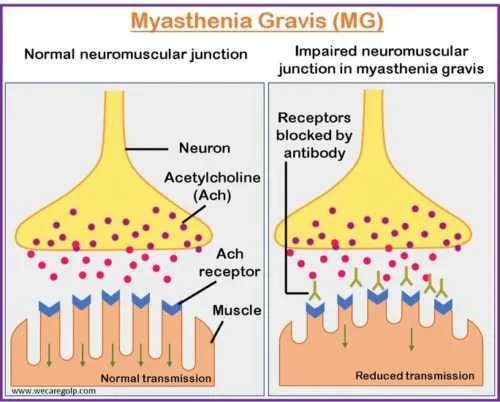
- Patho: Autoimmune. IgG Abs vs. postsynaptic AChRs (Acetylcholine Receptors) (80-90%) or MuSK (Muscle-Specific Kinase). ↓ACh binding at NMJ.
- Clinical: Fluctuating, fatigable weakness (worse with use/end of day, better with rest).
- Ocular (common initial): Ptosis, diplopia.
- Bulbar: Dysphagia, dysarthria, "nasal" voice.
- Generalized: Proximal muscle weakness. Normal reflexes & sensation.
- Diagnosis:
- AChR-Ab (serum, best initial). MuSK-Ab if AChR-Ab negative.
- Electrophysiology:
- RNS (Repetitive Nerve Stimulation): >10% decremental response at 3 Hz.
- SFEMG (Single Fiber EMG): ↑ jitter & blocking (most sensitive).
- Ice pack test: Improves ptosis.
- Chest CT/MRI: For thymoma/thymic hyperplasia.
⭐ Myasthenia Gravis is strongly associated with thymic hyperplasia (70%) or thymoma (10-15%).
- Treatment:
- Symptomatic: Pyridostigmine (AChE inhibitor).
- Chronic Immunomodulation: Prednisolone, Azathioprine, Mycophenolate.
- Rapid (Crisis/Severe): IVIg, Plasmapheresis.
- Thymectomy: All thymoma patients; generalized MG in younger patients (<60-65 yrs).
- Myasthenic Crisis: Respiratory failure due to severe weakness. Improves with Edrophonium (Tensilon) test.
- Cholinergic Crisis: Due to AChE inhibitor overdose. Worsens with Edrophonium. 📌 DUMBELS (Diarrhea, Urination, Miosis, Bronchospasm/Bradycardia, Emesis, Lacrimation, Salivation) or SLUDGE-M.
Lambert-Eaton Syndrome - Calcium Blockade Blues
- Pathophysiology: Autoantibodies target presynaptic P/Q-type voltage-gated $Ca^{2+}$ channels (VGCC) → ↓ Acetylcholine (ACh) release.
- Association: Often paraneoplastic, especially Small Cell Lung Cancer (SCLC) (~50-60%).
- 📌 LEMS: Lung cancer, Exercise helps, Motor (presynaptic), Stimulation (increment).
- Symptoms: Proximal muscle weakness (improves with brief exercise - "second wind"), hyporeflexia, autonomic dysfunction (dry mouth, constipation).
- Diagnosis:
- Anti-VGCC antibodies.
- Electromyography (EMG): ↓ CMAP amplitude.
⭐ LEMS classically shows an incremental response (facilitation >100%) on high-frequency repetitive nerve stimulation (RNS).
- Treatment: Address underlying SCLC; 3,4-diaminopyridine; immunosuppressants.

Other NMJ Disruptors - Toxic Transmissions
- Organophosphates/Carbamates: AChE inhibitors → cholinergic crisis (DUMBELS 📌). Rx: Atropine, Pralidoxime (OPs).
- Botulinum Toxin: Presynaptic block of ACh release → flaccid paralysis.
⭐ Botulinum toxin causes irreversible inhibition of ACh release, leading to flaccid paralysis; recovery requires sprouting of new nerve terminals.
- Tetanus Toxin: Blocks glycine/GABA release (spinal cord) → spastic paralysis.
- Aminoglycosides: ↓ Presynaptic ACh release; can worsen Myasthenia Gravis.
- Black Widow Spider Venom: Massive ACh release then depletion → cramps, pain.
- Neurotoxic Snake Venoms:
- α-bungarotoxin: Postsynaptic AChR block.
- β-bungarotoxin: Presynaptic ↓ ACh release.
NMJ Disorders - Compare & Contrast Clinic
| Feature | Myasthenia Gravis (MG) | Lambert-Eaton (LEMS) |
|---|---|---|
| Pathology | Post-synaptic: AChR Antibodies | Pre-synaptic: VGCC Antibodies, ↓ACh release |
| Weakness | Fluctuating; Ocular, Bulbar, Proximal | Proximal (legs > arms); Spares Ocular/Bulbar initially |
| Exertion | Worsens (fatigability) | Transient improvement (facilitation) |
| Reflexes | Normal / Fatigable | ↓/Absent; Augment post-exercise |
| Autonomic | Rare | Common (dry mouth, impotence) |
High‑Yield Points - ⚡ Biggest Takeaways
- Myasthenia Gravis: Postsynaptic AChR antibodies cause fluctuating weakness (ptosis, diplopia); Tensilon test positive; thymoma association.
- LEMS: Presynaptic VGCC antibodies cause proximal weakness improving with exercise; strong SCLC link.
- Botulism: Toxin inhibits presynaptic ACh release, causing descending flaccid paralysis; infantile form via honey.
- Organophosphate Poisoning: AChE inhibition causes cholinergic crisis (DUMBBELLS); treat with atropine & pralidoxime.
- RNS: Shows decremental response in MG, incremental in LEMS.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more