Platelet Essentials - Hemostasis Heroes
- Small, anucleated cells derived from bone marrow megakaryocytes. Lifespan: 7-10 days. Normal count: 1.5 - 4.5 lakhs/µL.
- Key players in primary hemostasis: forming the initial platelet plug.
- Contain α-granules (vWF, fibrinogen) & dense granules (ADP, Ca²⁺, serotonin).
- Key surface receptors: GPIb (binds vWF for adhesion), GPIIb/IIIa (binds fibrinogen for aggregation).
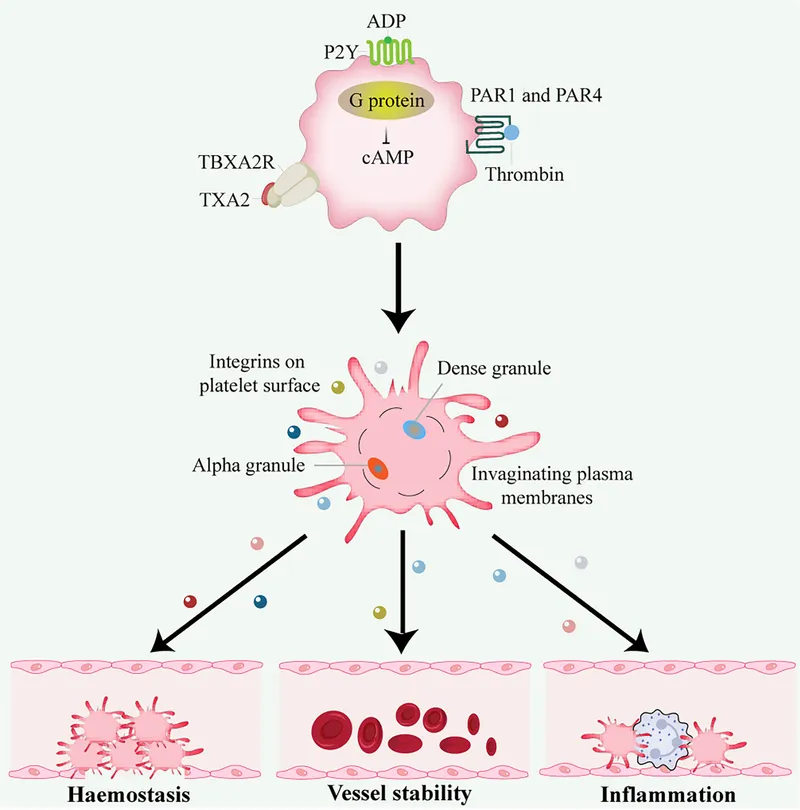
⭐ Glanzmann thrombasthenia results from a deficiency or dysfunction of the GPIIb/IIIa receptor, leading to impaired platelet aggregation.
Thrombocytopenia: Causes & Approach - Count Catastrophe
- Platelets < 150,000/μL. Severe: < 50,000/μL. Bleed risk ↑ if < 10,000-20,000/μL.
- Always rule out 📌 Pseudothrombocytopenia (EDTA clumping) with citrate tube/smear.
- Major Mechanisms & Causes:
- ↓ Production: Marrow disorders (aplasia, leukemia, MDS), B12/folate def., drugs, viral (HIV).
- ↑ Destruction:
- Immune: ITP, HIT, drugs, SLE.
- Non-immune: DIC, TTP-HUS, sepsis, HELLP.
- Sequestration: Splenomegaly (e.g., cirrhosis).
- Dilutional: Massive transfusion.
- Approach Algorithm:
⭐ ITP is a diagnosis of exclusion: isolated thrombocytopenia, normal marrow (if done), no other cause. Often follows viral illness in children.
Immune Thrombocytopenias - Self Sabotage
| Feature | ITP | HIT | Drug-Induced |
|---|---|---|---|
| Mechanism | Anti-GpIIb/IIIa autoAbs | Abs vs PF4-heparin | Drug-dependent Abs |
| Onset | Insidious/Acute | 5-10 days post-heparin | Acute post-drug |
| Platelets | <30k/µL often | ↓ >50%; rarely <20k/µL | Variable, severe |
| Hallmark | Isolated thrombocytopenia | Thrombosis risk; 📌 4Ts Score | Drug link; resolves on stop |
| Diagnosis | Exclusion; Anti-platelet Abs | 4Ts; HIT Ab assay | Drug Hx |
| Treatment | Steroids, IVIG, TPO-RAs | Stop heparin; DTI (e.g. Argatroban) | Stop drug; supportive |
⭐ HIT: prothrombotic despite thrombocytopenia due to Ab-mediated platelet activation.
MAHAs & Consumptive Coagulopathies - Fragmented Frenzy
RBC fragmentation (schistocytes) & thrombocytopenia define Microangiopathic Hemolytic Anemias (MAHAs).

- Comparison:
Feature TTP HUS DIC Cause ↓ADAMTS13 (<10%) Shiga toxin (E.coli) Sepsis, trauma, malignancy Clinical 📌 FAT RN Pentad (Fever, Anemia, Thrombocytopenia, Renal, Neuro) Triad (Anemia, Thrombocytopenia, AKI - esp. kids) Bleeding & thrombosis Coags Normal Normal ↑PT/PTT, ↑D-dimer, ↓Fibrinogen Rx Plasma Exchange (PEX) Supportive Treat cause, FFP, Cryo
⭐ In TTP, initiate plasma exchange emergently upon suspicion, pre-ADAMTS13 results.
Platelet Dysfunction & Thrombocytosis - Sticky & Swarming
- Platelet Dysfunction (Qualitative)
- Inherited:
Feature Glanzmann's (GT) Bernard-Soulier (BSS) Defect GpIIb/IIIa (Aggregation) GpIb (Adhesion) Inheritance AR AR Ristocetin Agg. Normal ↓ / Absent Platelet Size Normal Giant (📌 Big Suckers) - Acquired: Uremia, drugs (Aspirin, Clopidogrel).

- Inherited:
- Thrombocytosis (Quantitative): Platelet count > 450,000/μL.
Feature Reactive Clonal (ET) Cause Infection, inflammation, Fe def JAK2 mut. (MPN) Platelet Func. Normal Often Abnormal Splenomegaly No (or from cause) Possible Treatment Treat cause Cytoreduction, Aspirin
⭐ BSS: Absent Ristocetin aggregation. Giant platelets. Defect in GpIb (vWF receptor).
High‑Yield Points - ⚡ Biggest Takeaways
- ITP: Isolated thrombocytopenia from anti-GpIIb/IIIa antibodies. First-line: steroids.
- TTP: ADAMTS13 deficiency; Pentad (Fever, MAHA, Thrombocytopenia, Renal, Neuro). Plasma exchange is crucial.
- HUS: Often post-E. coli O157:H7; Triad (MAHA, Thrombocytopenia, ARF). Primarily supportive.
- Bernard-Soulier Syndrome: GpIb defect (adhesion); Giant platelets, thrombocytopenia.
- Glanzmann Thrombasthenia: GpIIb/IIIa defect (aggregation); Normal count, impaired aggregation.
- von Willebrand Disease (vWD): Most common inherited bleeding disorder; ↓vWF, ↓FVIII. Desmopressin for Type 1.
- DIC: Consumptive coagulopathy; ↓platelets, ↓fibrinogen, ↑PT/APTT, ↑D-dimer. Treat underlying cause.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

