Inheritance Patterns - Gene Game Rules
-
Autosomal Dominant (AD): Vertical transmission. 50% offspring risk. Variable expressivity. New mutations.
-
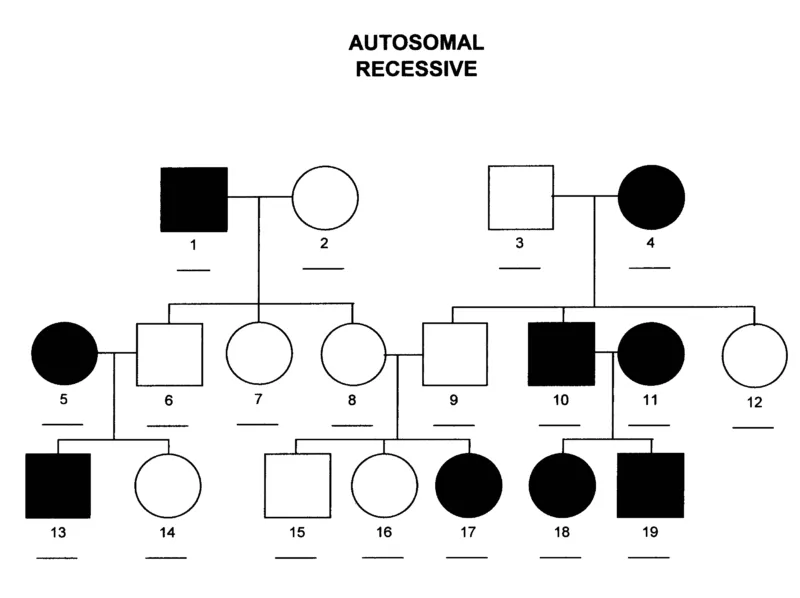
Autosomal Recessive (AR): Horizontal. Skips generations. 25% risk (carrier parents). Consanguinity ↑.
-
X-linked Recessive (XLR): Males > Females. No male-to-male. Carrier ♀ → 50% sons affected.
-
X-linked Dominant (XLD): Affected ♂ → all daughters. Affected ♀ → 50% offspring.
-
Mitochondrial: Maternal. Affected ♀ → all offspring. Heteroplasmy.
-
Key Concepts:
- Penetrance: Genotype shows phenotype (%).
- Expressivity: Severity varies.
- Pleiotropy: 1 gene, multiple effects.
- Anticipation: Worsens/earlier over generations.
-
Pedigree: □ Male, ○ Female, Shaded=Affected.

⭐ For Autosomal Dominant, think vertical transmission (parent to child) and variable expressivity. Achondroplasia often arises from a new mutation (Advanced Paternal Age).
Autosomal Dominant - Top Dog Genes
- Marfan Syndrome
- Gene: FBN1 (Fibrillin-1)
- Features: Arachnodactyly, ectopia lentis, aortic root dilatation/dissection. 📌 FAME: Fibrillin, Arachnodactyly, Mitral valve prolapse, Ectopia lentis.
- Clues: Ghent criteria, family history.
- Huntington Disease
- Gene: HTT (Huntingtin); CAG repeats >39 for full penetrance.
- Features: Chorea, cognitive decline, psychiatric disturbances.
- Clues: Family history, genetic testing (CAG repeat count).
- Neurofibromatosis Type 1 (NF1)
- Gene: NF1 (Neurofibromin)
- Features: Café-au-lait macules (≥6), neurofibromas, Lisch nodules (iris hamartomas), optic glioma.
- Clues: NIH diagnostic criteria.
- Achondroplasia
- Gene: FGFR3 (Fibroblast Growth Factor Receptor 3)
- Features: Rhizomelic short stature, macrocephaly, frontal bossing, trident hand.
- Clues: Clinical features, characteristic X-ray findings.
⭐ Huntington Disease is characterized by anticipation, where the disease manifests earlier and more severely in successive generations due to expansion of CAG trinucleotide repeats.
Autosomal Recessive - Hidden Heirs
- Cystic Fibrosis (CF)
- Gene: CFTR (ΔF508 common)
- Defect: Defective chloride channel
- Features: Recurrent lung infections, pancreatic insufficiency, meconium ileus, male infertility
- Dx: Sweat chloride > 60 mEq/L, genetic tests, newborn screening
- Sickle Cell Anemia
- Gene: HBB
- Defect: HbS (abnormal β-globin)
- Features: Vaso-occlusive crises, hemolytic anemia, dactylitis, acute chest syndrome
- Dx: Hb electrophoresis, newborn screen
- Phenylketonuria (PKU)
- Gene: PAH
- Defect: ↓ Phenylalanine hydroxylase
- Features: Intellectual disability, seizures, musty odor, eczema
- Dx: Newborn screen (↑ Phenylalanine)
- Tay-Sachs Disease
- Gene: HEXA
- Defect: ↓ Hexosaminidase A
- Features: Progressive neurodegeneration, cherry-red macula, exaggerated startle
- Dx: Enzyme assay, genetic testing
- Thalassemias (α & β)
- Gene: HBA1/2 (α), HBB (β)
- Defect: ↓ Globin chain synthesis
- Features: Microcytic anemia, hepatosplenomegaly, bone deformities (β-major)
- Dx: Hb electrophoresis, CBC (↓MCV)
⭐ The most common mutation in Cystic Fibrosis is ΔF508 in the CFTR gene, leading to defective chloride transport and characteristically high sweat chloride levels.## Autosomal Recessive - Hidden Heirs
- Cystic Fibrosis (CF)
- Gene: CFTR (ΔF508 common)
- Defect: Defective chloride channel
- Features: Recurrent lung infections, pancreatic insufficiency, meconium ileus, male infertility
- Dx: Sweat chloride > 60 mEq/L, genetic tests, newborn screening
- Sickle Cell Anemia
- Gene: HBB
- Defect: HbS (abnormal β-globin)
- Features: Vaso-occlusive crises, hemolytic anemia, dactylitis, acute chest syndrome
- Dx: Hb electrophoresis, newborn screen
- Phenylketonuria (PKU)
- Gene: PAH
- Defect: ↓ Phenylalanine hydroxylase
- Features: Intellectual disability, seizures, musty odor, eczema
- Dx: Newborn screen (↑ Phenylalanine)
- Tay-Sachs Disease
- Gene: HEXA
- Defect: ↓ Hexosaminidase A
- Features: Progressive neurodegeneration, cherry-red macula, exaggerated startle
- Dx: Enzyme assay, genetic testing
- Thalassemias (α & β)
- Gene: HBA1/2 (α), HBB (β)
- Defect: ↓ Globin chain synthesis
- Features: Microcytic anemia, hepatosplenomegaly, bone deformities (β-major)
- Dx: Hb electrophoresis, CBC (↓MCV) (image)[08bd91ea-483f-48a3-94eb-ea85ca8684f6]
⭐ The most common mutation in Cystic Fibrosis is ΔF508 in the CFTR gene, leading to defective chloride transport and characteristically high sweat chloride levels.## Autosomal Recessive - Hidden Heirs
- Cystic Fibrosis (CF)
- Gene: CFTR (ΔF508 common)
- Defect: Defective chloride channel
- Features: Recurrent lung infections, pancreatic insufficiency, meconium ileus, male infertility
- Dx: Sweat chloride > 60 mEq/L, genetic tests, newborn screening
- Sickle Cell Anemia
- Gene: HBB
- Defect: HbS (abnormal β-globin)
- Features: Vaso-occlusive crises, hemolytic anemia, dactylitis, acute chest syndrome
- Dx: Hb electrophoresis, newborn screen
- Phenylketonuria (PKU)
- Gene: PAH
- Defect: ↓ Phenylalanine hydroxylase
- Features: Intellectual disability, seizures, musty odor, eczema
- Dx: Newborn screen (↑ Phenylalanine)
- Tay-Sachs Disease
- Gene: HEXA
- Defect: ↓ Hexosaminidase A
- Features: Progressive neurodegeneration, cherry-red macula, exaggerated startle
- Dx: Enzyme assay, genetic testing
- Thalassemias (α & β)
- Gene: HBA1/2 (α), HBB (β)
- Defect: ↓ Globin chain synthesis
- Features: Microcytic anemia, hepatosplenomegaly, bone deformities (β-major)
- Dx: Hb electrophoresis, CBC (↓MCV) (image)[08bd91ea-483f-48a3-94eb-ea85ca8684f6]
⭐ The most common mutation in Cystic Fibrosis is ΔF508 in the CFTR gene, leading to defective chloride transport and characteristically high sweat chloride levels.
X-Linked & Mitochondrial - Special Ops Genes
-
X-Linked Recessive (XLR): No male-to-male transmission.
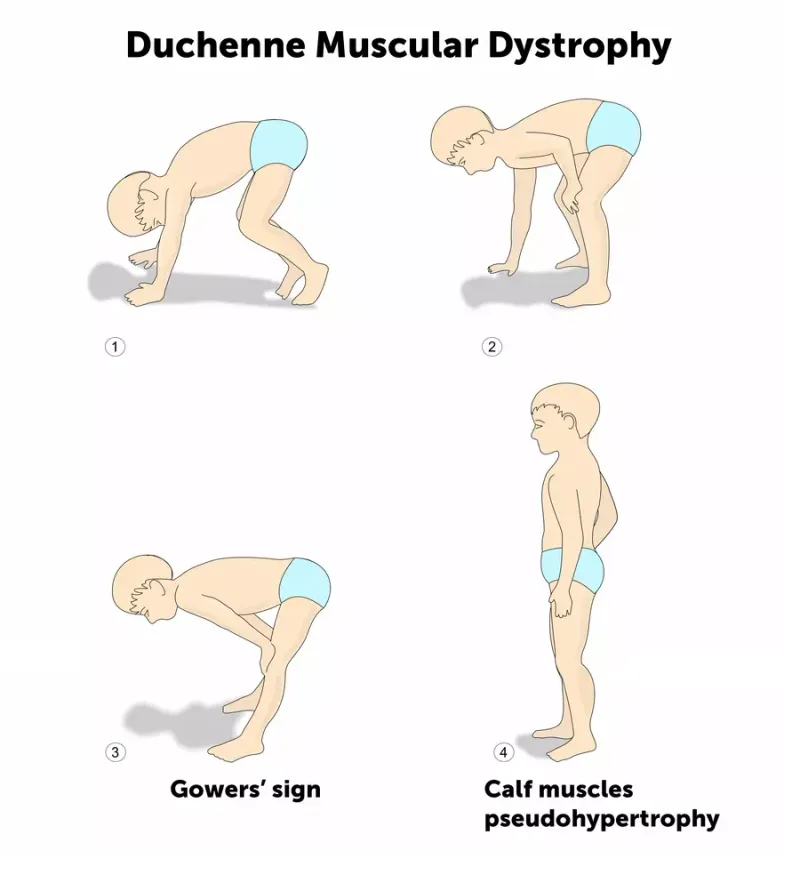
- Duchenne/Becker Muscular Dystrophy (DMD/BMD): DMD gene. Muscle weakness, Gower's sign, calf pseudohypertrophy. Becker milder.
- Hemophilia A/B: Factor VIII/IX deficiency. Bleeding, hemarthrosis, ↑aPTT.
- G6PD Deficiency: G6PD gene. Hemolytic anemia (triggers: drugs, fava), Heinz bodies. 📌 Heinz = G6PD.
- Duchenne/Becker Muscular Dystrophy (DMD/BMD): DMD gene. Muscle weakness, Gower's sign, calf pseudohypertrophy. Becker milder.
-
X-Linked Dominant (XLD): Affected father → all daughters affected, no sons.
- Fragile X Syndrome: FMR1 (CGG >200). ID, long face, macroorchidism. Anticipation.
- Rett Syndrome: MECP2. Girls: neuro-regression, hand-wringing (lethal males).
-
Mitochondrial: Maternal inheritance (mother to ALL offspring). Variable expressivity.
- LHON: Bilateral vision loss.
- MELAS: Mitochondrial Encephalopathy, Lactic Acidosis, Stroke-like episodes.
⭐ Affected XLR males transmit to all daughters (carriers), never sons. Gower's sign: classic in DMD.
High‑Yield Points - ⚡ Biggest Takeaways
- Autosomal Dominant: Vertical transmission, 50% offspring risk; Marfan syndrome, Huntington disease.
- Autosomal Recessive: Horizontal transmission (sibs), 25% offspring risk; consanguinity key; Cystic Fibrosis.
- X-linked Recessive: Affects males mainly, carrier females; no male-to-male transmission; Duchenne MD.
- X-linked Dominant: Affected fathers to all daughters, no sons; Rett syndrome.
- Mitochondrial Inheritance: Maternal transmission to all offspring; heteroplasmy (variable severity).
- Concepts: Penetrance, variable expressivity, pleiotropy, anticipation (Huntington's).
- Dynamic mutations: Expanding trinucleotide repeats cause Fragile X, Myotonic Dystrophy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

