Principles of Medical Genetics - Code's Core
- DNA & RNA: Fundamental nucleic acids.
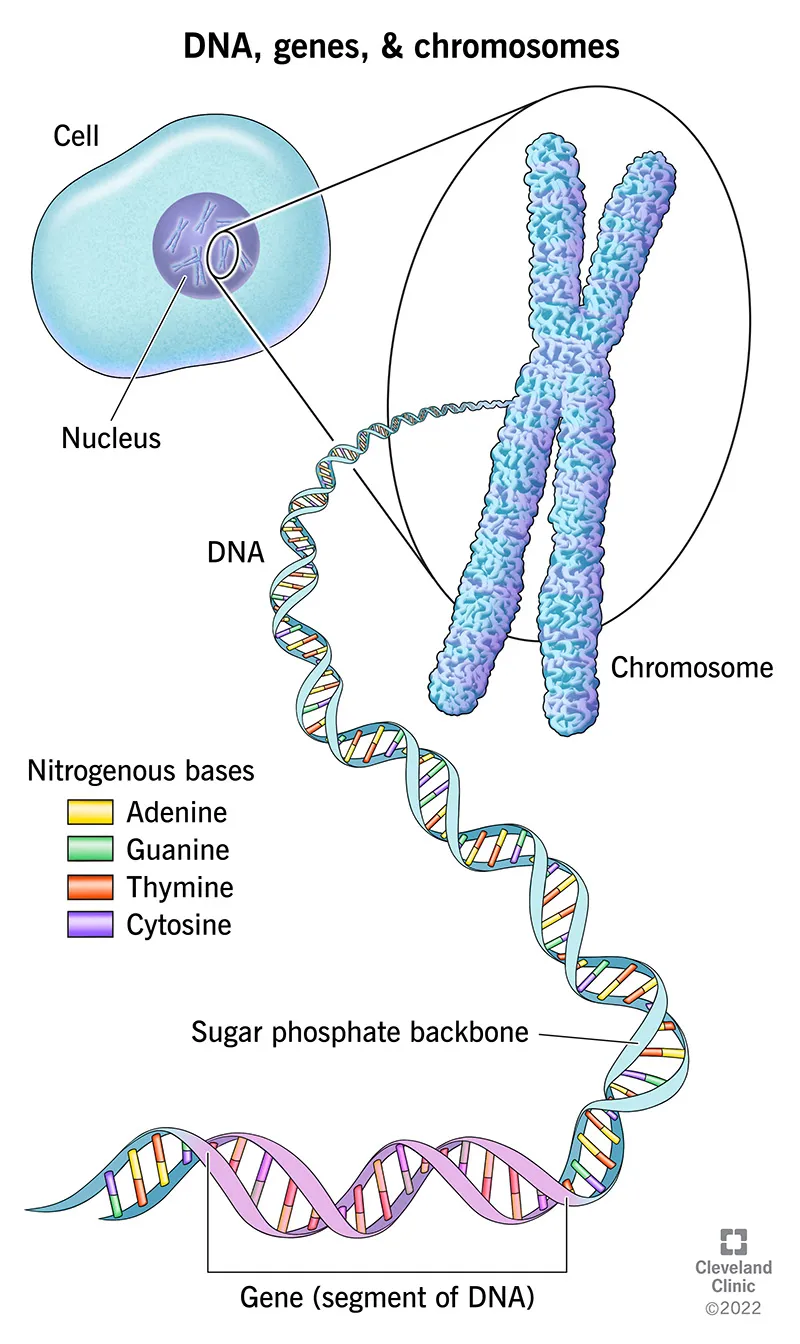
- DNA (Deoxyribonucleic Acid): Double helix; A-T, G-C base pairing; stores genetic blueprint.
- RNA (Ribonucleic Acid): Single strand; A-U, G-C pairing; involved in protein synthesis & gene regulation.
- Gene: Basic hereditary unit; DNA segment coding for a functional product (protein/RNA).
- Chromosome: Organized structure of DNA & proteins; humans have 23 pairs (46 total).
- Genome: An organism's complete set of DNA.
- Mutation: Permanent alteration in DNA sequence.
- Point Mutation: Single nucleotide change (e.g., silent, missense, nonsense).
- Frameshift Mutation: Insertion/deletion of nucleotides (not in multiples of three); alters reading frame.
- Chromosomal Aberrations: Changes in chromosome number or structure.
- Key Terminology:
- Allele: Alternative form of a gene at a given locus.
- Locus: Specific physical location of a gene on a chromosome.
- Genotype: Genetic constitution of an individual.
- Phenotype: Observable characteristics resulting from genotype-environment interaction.
⭐ Single Nucleotide Polymorphisms (SNPs) are the most common type of genetic variation among people, each SNP representing a difference in a single DNA building block, called a nucleotide.
Principles of Medical Genetics - Family Lines
Pedigree analysis: Visual tool tracking genetic traits across generations. Key for pattern recognition & risk assessment.
- Autosomal Dominant (AD):
- Vertical pattern; affects both sexes.
- 50% risk to offspring from affected heterozygote.
- Autosomal Recessive (AR):
- Horizontal pattern (siblings); skips generations.
- Parents usually unaffected carriers.
- 25% risk to offspring of two carriers. Consanguinity ↑ risk.
- X-linked Recessive (XLR):
- Mainly males affected; carrier females.
- No male-to-male transmission.
- X-linked Dominant (XLD):
- Affected fathers: all daughters affected, no sons.
- Affected mothers (heterozygous): 50% risk to offspring (any sex).
- Y-linked (Holandric):
- Only males affected; father to all sons.
- Mitochondrial:
- Maternal inheritance: affected mother to ALL offspring.
- Fathers don't transmit.

⭐ Variable expressivity and incomplete penetrance can complicate pedigree analysis in Autosomal Dominant conditions.
Principles of Medical Genetics - Count & Construct
- Chromosomal Abnormalities: Deviations in chromosome number or structure.
- Numerical Abnormalities (Aneuploidy): Gain or loss of chromosomes.
- Trisomy: Extra chromosome (e.g., Down Syndrome - Trisomy 21).
- Monosomy: Missing chromosome (e.g., Turner Syndrome - 45,X0).
- Examples:
- Down Syndrome (47,XX,+21 or 47,XY,+21)
- Turner Syndrome (45,X0)
- Klinefelter Syndrome (47,XXY)
- Structural Abnormalities: Changes in chromosome structure.
- Deletions: Loss of a chromosome segment (e.g., Cri-du-chat Syndrome - 5p deletion).
- Duplications: Repetition of a chromosome segment.
- Translocations: Exchange of segments between non-homologous chromosomes (e.g., Philadelphia chromosome in CML - t(9;22)).
- Inversions: Segment reversed.
- Numerical Abnormalities (Aneuploidy): Gain or loss of chromosomes.
- Karyotyping: Visual analysis of chromosomes; detects numerical and large structural changes.

⭐ Robertsonian translocation is a common cause of familial Down Syndrome, involving acrocentric chromosomes (13, 14, 15, 21, 22).
Principles of Medical Genetics - Disease Detectives
- Key Diagnostic Techniques:
- PCR (Polymerase Chain Reaction): Amplifies specific DNA segments. Used for infections, single gene disorders.
- FISH (Fluorescent In Situ Hybridization): Visualizes specific DNA sequences on chromosomes; detects aneuploidy, deletions.
- Microarrays (CGH, SNP): Genome-wide detection of copy number variations (CNVs) and SNPs.
- Sequencing (Sanger, Next-Generation Sequencing - NGS): Determines exact nucleotide order.
- Prenatal Diagnosis Methods:
- Invasive: Chorionic Villus Sampling (CVS) (10-13 wks), Amniocentesis (15-20 wks).
- Non-Invasive Prenatal Testing (NIPT): Analyzes cell-free fetal DNA in maternal blood.
- Population Genetics:
- Hardy-Weinberg Equilibrium: $p^2 + 2pq + q^2 = 1$ and $p+q=1$. Describes stable allele/genotype frequencies.
- Genetic Counseling Essentials:
- Providing information, risk assessment, discussing implications, informed consent, psychosocial support.
⭐ Trinucleotide repeat expansion disorders (e.g., Huntington's, Myotonic Dystrophy) often show anticipation - increased severity/earlier onset in successive generations.
High‑Yield Points - ⚡ Biggest Takeaways
- Autosomal Dominant: Vertical transmission; 50% offspring risk; variable expressivity.
- Autosomal Recessive: Horizontal transmission; 25% offspring risk (carrier parents); consanguinity ↑ risk.
- X-linked Recessive: Affects males; no male-to-male transmission; carrier females.
- Mitochondrial Inheritance: Maternal transmission to all offspring; heteroplasmy causes variability.
- Penetrance: All-or-none expression; Expressivity: Severity variation.
- Hardy-Weinberg principle predicts genotype frequencies from allele frequencies in populations.
- Pleiotropy: One gene, multiple traits. Locus heterogeneity: Different genes, same disease.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

