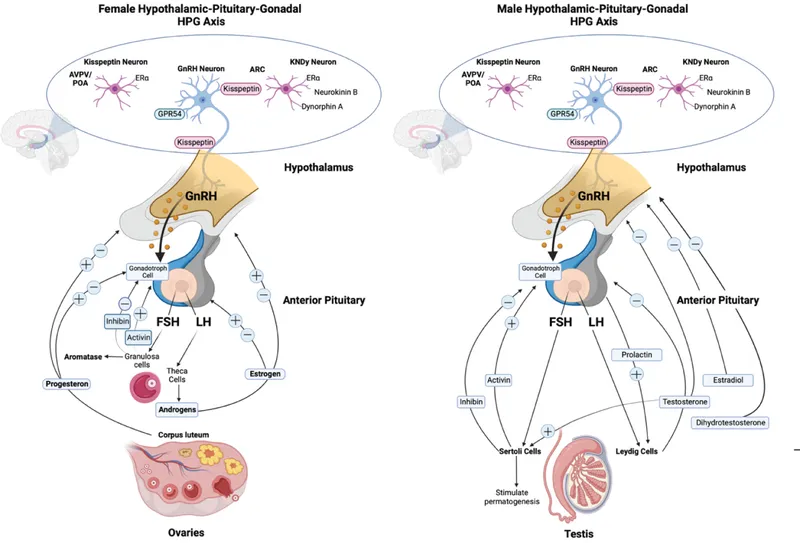
HPG Axis & Puberty - Hormonal Harmony
- HPG Axis:
- Hypothalamus: Pulsatile Gonadotropin-Releasing Hormone ($GnRH$).
- Pituitary: Luteinizing Hormone ($LH$) & Follicle-Stimulating Hormone ($FSH$).
- Gonads:
- $LH$ → Theca/Leydig cells → Androgens (Testosterone).
- $FSH$ → Granulosa/Sertoli cells → Gametogenesis, Estrogen, Inhibin.
- Regulation:
- Negative Feedback: Sex steroids, Inhibin (on $FSH$).
- Positive Feedback: Activin (on $FSH$).
- Puberty Onset:
- Reactivation of pulsatile $GnRH$. Leptin permissive.
- Girls: Thelarche (Estrogen-driven) often first sign.
- Boys: Testicular enlargement (>4ml or >2.5cm; Testosterone-driven) often first sign.
⭐ Kallmann Syndrome: Defective GnRH neuron migration (anosmia + hypogonadotropic hypogonadism). Often due to KAL1 gene mutation.
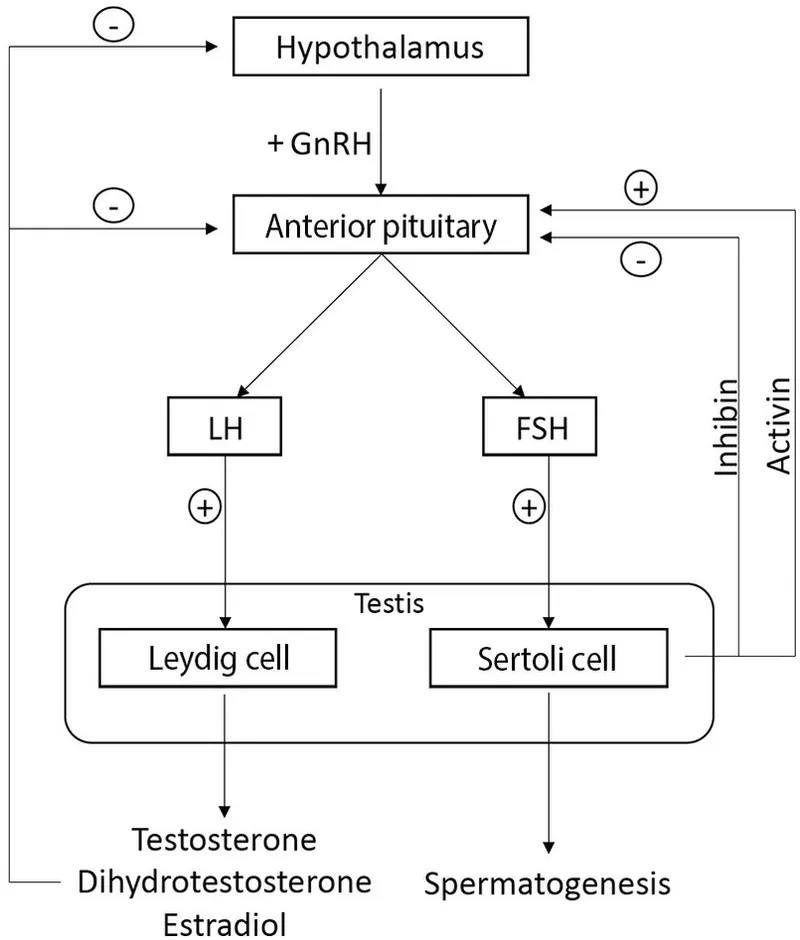
Male Repro Endo - Testo Tune-Up
- HPG Axis (Male): Hypothalamus (GnRH) → Pituitary (LH, FSH) → Testes.
- LH → Leydig cells → Testosterone (T).
- FSH → Sertoli cells → Spermatogenesis, Inhibin B.
- Testosterone:
- Functions: Spermatogenesis, 2° sexual characteristics, libido, muscle/bone mass.
- Transport: ~2% Free (active), SHBG, Albumin.
- Metabolism: → DHT (5α-reductase); → Estradiol (Aromatase).
- Spermatogenesis: In seminiferous tubules; supported by Sertoli cells. Inhibin B from Sertoli cells selectively inhibits FSH.
- Key Disorders:
- Hypogonadism:
- Primary: Testicular failure (↑LH/FSH, ↓T). E.g., Klinefelter (XXY).
- Secondary: Pituitary/Hypothalamic (↓/N LH/FSH, ↓T). E.g., Kallmann (anosmia).
- Androgen Insensitivity Syndrome (AIS): Receptor defect.
- Hypogonadism:
⭐ Klinefelter syndrome (47,XXY) is the most common chromosomal disorder causing male hypogonadism.
Menstrual Cycle - Monthly Marvels
- Cycle Basics:
- Avg. 28 days (range 21-35). Menses: 2-7 days, loss ~35 mL.
- Phases: Follicular (variable, proliferative), Ovulation, Luteal (fixed 14 days, secretory).
- Hormonal Axis: GnRH → FSH/LH → Estrogen/Progesterone.
- Follicular Phase (Days 1 to ~13):
- ↑FSH → follicle growth; dominant follicle selected.
- ↑Estrogen from follicle → endometrial proliferation.
- Ovulation (Day ~14):
- Sustained high Estrogen → LH surge (positive feedback).
- Ovum released 10-12 hrs post LH peak.
- 📌 Mnemonic: Ovulation by LH (LHas Out).
- Luteal Phase (Days ~15 to 28):
- Corpus luteum → ↑Progesterone (dominant) & Estrogen.
- Progesterone → secretory endometrium, ↑basal body temp.
- No fertilization → corpus luteum atrophies → ↓hormones → menstruation.
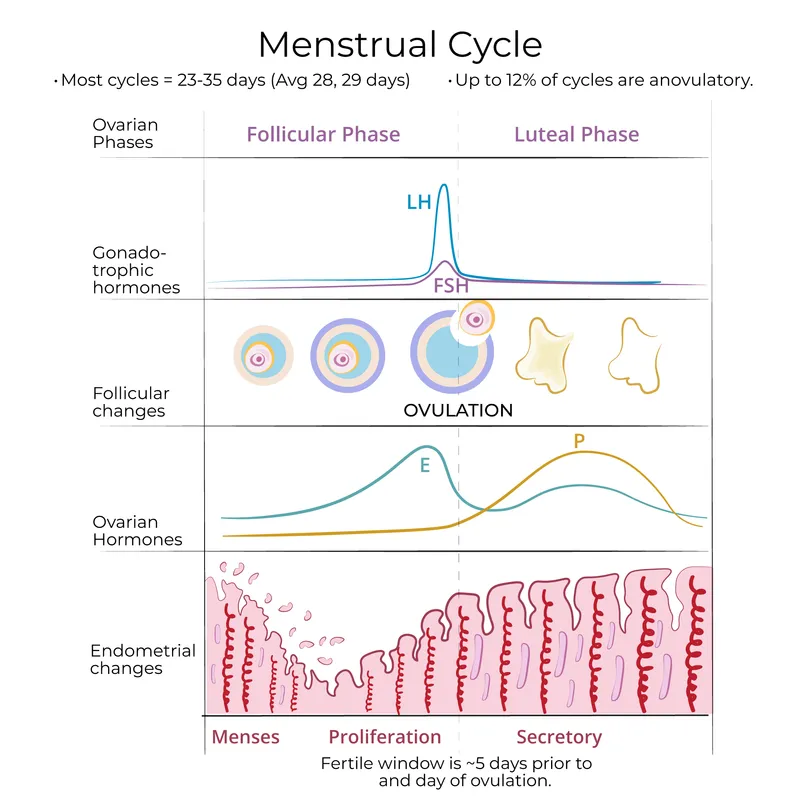
⭐ LH surge precedes ovulation by 24-36 hours; ovulation occurs 10-12 hours after the LH peak. Triggered by high estrogen levels from the dominant follicle anovulatory cycles can occur despite bleeding due to estrogen withdrawal if ovulation fails and no corpus luteum forms.
Female Repro Disorders - Womb Woes
-
Abnormal Uterine Bleeding (AUB):
- 📌 PALM-COEIN for causes:
- Polyp, Adenomyosis, Leiomyoma, Malignancy/Hyperplasia
- Coagulopathy, Ovulatory dysfunction, Endometrial, Iatrogenic, Not yet classified.
- 📌 PALM-COEIN for causes:
-
Leiomyoma (Fibroids): Benign uterine smooth muscle tumors. Types: Submucosal (↑AUB), Intramural, Subserosal. Symptoms: AUB, pressure, pain.
-
Endometriosis: Ectopic endometrial tissue (ovary: "chocolate cyst"). Symptoms: Dysmenorrhea, dyspareunia, infertility, chronic pelvic pain.
-
Adenomyosis: Endometrial glands/stroma within myometrium. Uterus: bulky, tender, "boggy". Symptoms: Menorrhagia, dysmenorrhea.
-
Endometrial Hyperplasia & Carcinoma: Key risk: unopposed estrogen.
⭐ Postmenopausal bleeding (PMB) is endometrial cancer until proven otherwise; requires prompt evaluation.
High‑Yield Points - ⚡ Biggest Takeaways
- PCOS: Rotterdam criteria (2/3: oligo/anovulation, hyperandrogenism, PCO on USG), ↑LH/FSH ratio.
- Amenorrhea workup: Exclude pregnancy (β-hCG); then TSH, Prolactin, FSH.
- Turner Syndrome (45,XO): Streak gonads, primary amenorrhea, short stature, ↑FSH/LH.
- Klinefelter Syndrome (47,XXY): Testicular atrophy, gynecomastia, azoospermia, ↑FSH/LH, ↓Testosterone.
- CAH (21-hydroxylase deficiency): ↑17-OHP, ambiguous female genitalia, salt wasting.
- Kallmann Syndrome: Hypogonadotropic hypogonadism, anosmia (failed GnRH migration).
- Hyperprolactinemia: Prolactinoma causes galactorrhea, amenorrhea; treat: dopamine agonists.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more