Calcium & Phosphate - Mineral Harmony
- Normal Serum Calcium: 8.5-10.5 mg/dL (Total); 4.5-5.5 mg/dL (Ionized - active form).
- Normal Serum Phosphate: 2.5-4.5 mg/dL.
- Key Hormonal Regulators:
- Parathyroid Hormone (PTH): ↑ Ca, ↓ PO₄ (acts on bone, kidney).
- Vitamin D (Calcitriol): ↑ Ca, ↑ PO₄ (acts on gut, bone, kidney).
- Calcitonin: ↓ Ca, ↓ PO₄ (minor role in humans).
- Calcium-Phosphate Product: $Ca \times PO_4$ normally < 55 mg²/dL².
- 📌 Mnemonic: "PTH Pushes The High (Ca), Flushes The Low (PO₄)".
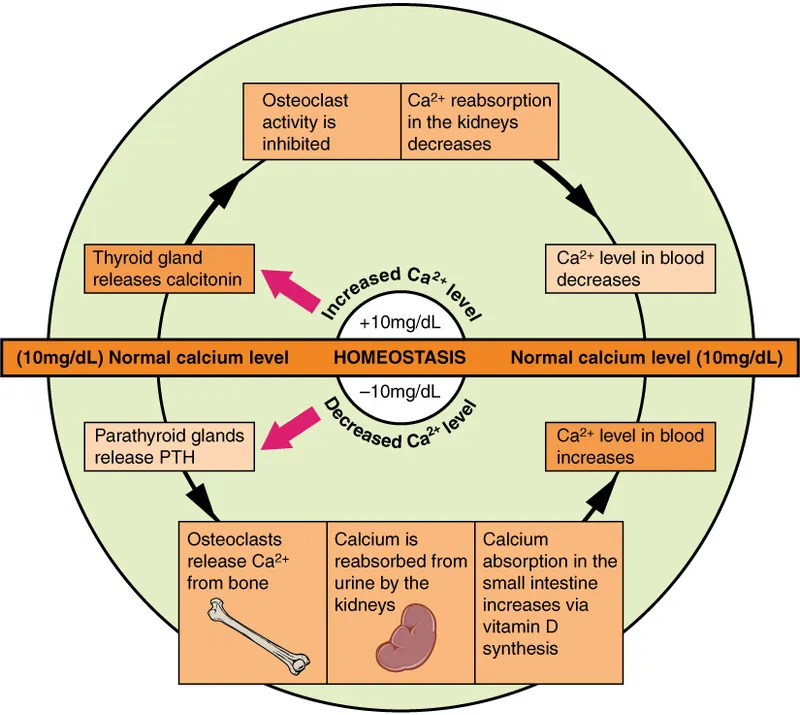
⭐ Ionized calcium is the physiologically active form and is affected by pH (acidosis ↑ ionized Ca, alkalosis ↓ ionized Ca).
Calcium's Captains - PTH & Vit D
Parathyroid Hormone (PTH):
- Secreted by: Parathyroid chief cells (stimulus: ↓ Serum $Ca^{2+}$).
- Key Actions:
- Bone: ↑ Osteoclast activity → ↑ $Ca^{2+}$ & ↑ $PO_4^{3-}$ release.
- Kidney: ↑ $Ca^{2+}$ reabsorption (DCT); ↓ $PO_4^{3-}$ reabsorption (PCT) → phosphaturia. 📌 PTH = Phosphate Trashing Hormone.
- Kidney: Stimulates 1α-hydroxylase → ↑ active Vit D ($1,25(OH)_2D$).
- Overall: ↑ Serum $Ca^{2+}$, ↓ Serum $PO_4^{3-}$.
Vitamin D (Calcitriol - $1,25(OH)_2D$):
- Activation: Diet/Skin → Liver ($25(OH)D$) → Kidney ($1,25(OH)_2D$ by 1α-hydroxylase; stim: PTH, ↓$Ca^{2+}$, ↓$PO_4^{3-}$).
- Key Actions:
- Intestine: ↑ $Ca^{2+}$ & ↑ $PO_4^{3-}$ absorption (primary effect).
- Bone: Promotes mineralization; high doses → resorption.
- Kidney: ↑ $Ca^{2+}$ & ↑ $PO_4^{3-}$ reabsorption.
- Parathyroid: ↓ PTH synthesis (feedback).
- Overall: ↑ Serum $Ca^{2+}$, ↑ Serum $PO_4^{3-}$.
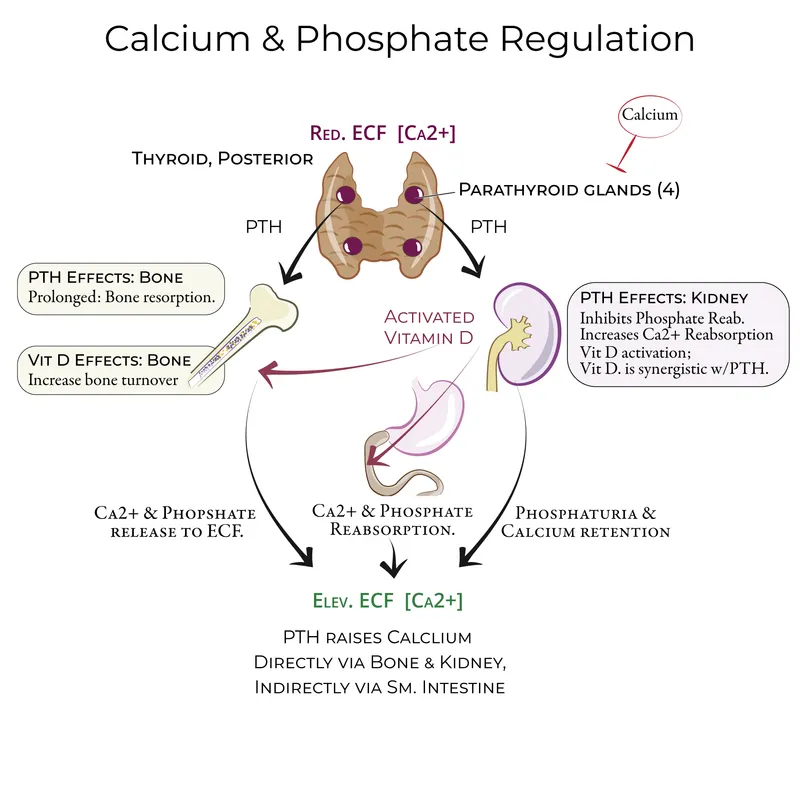
⭐ PTH primarily increases serum calcium and decreases serum phosphate (via phosphaturia), while active Vitamin D (calcitriol) increases both serum calcium and serum phosphate (via gut/kidney absorption).
Calcium Chaos - Ups & Downs Drama
Hypocalcemia (↓$Ca^{2+}$)
- Causes: Hypoparathyroidism, Vit D deficiency, CKD, ↓Mg.
- S/S: Tetany (Chvostek's, Trousseau's signs), paresthesia. 📌 CATS Go Numb (Convulsions, Arrhythmias, Tetany, Spasms). ECG: ↑QT interval.
- Rx: Acute: IV $Ca^{2+}$ gluconate. Chronic: Oral $Ca^{2+}$ + Vit D.
Hypercalcemia (↑$Ca^{2+}$)
- Causes:
- PTH-dependent: Primary hyperparathyroidism.
- PTH-independent: Malignancy (PTHrP), Vit D toxicity, Sarcoidosis. 📌 CHIMPANZEES.
- S/S: "Stones (renal), Bones (pain), Groans (abd pain), Thrones (polyuria), Psych". ECG: ↓QT interval.
- Rx: IV Saline, Furosemide (post-hydration), Bisphosphonates.
⭐ Malignancy & primary hyperparathyroidism: most common causes of hypercalcemia in adults.
Bone Structure Blues - When Bones Weaken
- Osteoporosis: Reduced bone mass & microarchitectural deterioration, ↑fracture risk.
- Risk Factors: Age, post-menopause, low Ca/Vit D, corticosteroids, smoking. 📌 ACCESS: Alcohol, Corticosteroid, Calcium low, Estrogen low, Smoking, Sedentary.
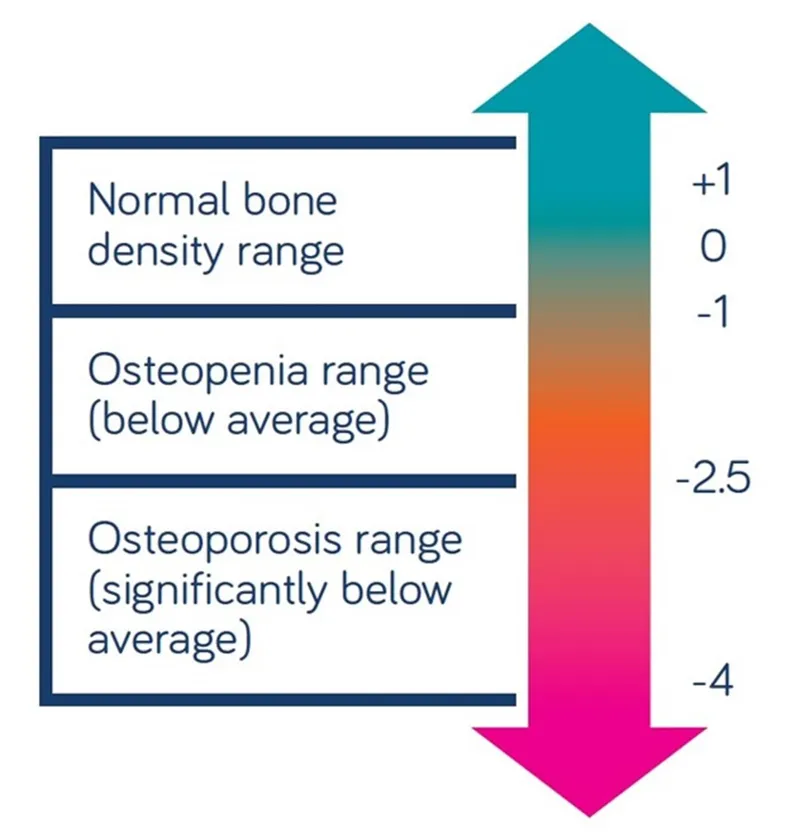
- Diagnosis: DEXA scan T-score ≤ -2.5.
- Clinical: Fragility fractures (vertebral, hip, Colles'). Often silent.
- Management: Calcium, Vit D, bisphosphonates, exercise.
- Osteomalacia & Rickets: Defective bone mineralization; soft bones.
- Rickets (children): Epiphyseal plate widening, bowing legs, rachitic rosary.
- Osteomalacia (adults): Bone pain, muscle weakness, waddling gait.
- Causes: Severe Vit D deficiency (common), renal phosphate wasting, malabsorption.
- Labs: ↓Ca²⁺, ↓PO₄³⁻ (or normal Ca²⁺ due to ↑PTH), ↑ALP, ↑PTH. $25(OH)D$ levels low.
⭐ Looser's zones (pseudofractures) on X-ray are characteristic of osteomalacia.
High-Yield Points - ⚡ Biggest Takeaways
- Primary hyperparathyroidism: Commonest outpatient hypercalcemia; stones, bones, groans.
- Vitamin D deficiency: Causes rickets/osteomalacia; ↓Ca, ↓PO4, ↑PTH, ↑ALP.
- Paget's disease of bone: ↑ALP, normal Ca/PO4; risk of osteosarcoma, deafness.
- Osteoporosis: Diagnosed by DEXA (T-score ≤ -2.5); bisphosphonates are first-line.
- Hypercalcemia of malignancy: Often due to PTHrP or lytic bone metastases.
- Hypoparathyroidism: Presents with ↓Ca, ↑PO4, ↓PTH; Chvostek's & Trousseau's signs.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

