Definition, Screening & Diagnosis - Spotting the Spirits
-
Alcohol Use Disorder (AUD): Maladaptive alcohol use causing significant impairment/distress.
- DSM-5 Criteria (≥2 of 11 criteria in 12 months):
- Mild: 2-3 criteria
- Moderate: 4-5 criteria
- Severe: ≥6 criteria
- DSM-5 Criteria (≥2 of 11 criteria in 12 months):
-
Screening Tools:
Tool Items Focus Key Cut-offs (Positive Screen) CAGE 4 Lifetime problem; Dependence cues ≥2 "Yes". 📌 (Cut down, Annoyed, Guilty, Eye-opener) AUDIT 10 Current use, Dependence, Problems Score ≥8 (general); ≥7 (women/elderly) AUDIT-C 3 At-risk drinking (heavy/binge) Score: Men ≥4; Women ≥3 -
Biomarkers (indicate heavy/prolonged use):
- ↑GGT (Gamma-Glutamyl Transferase)
- ↑MCV (Mean Corpuscular Volume)
- ↑CDT (Carbohydrate-Deficient Transferrin) - most specific for chronic alcohol consumption.
⭐ AUDIT-C, a 3-item questionnaire, is a highly effective screening tool for heavy drinking and AUD in primary care.
Acute Effects & Withdrawal - The Alcohol Rollercoaster
- Intoxication: Effects correlate with Blood Alcohol Concentration (BAC).
- 0.08% (Legal limit): Impaired coordination.
- >0.3%: Stupor, coma.
- Withdrawal: Begins 6-24h post-last drink. CIWA-Ar score for severity: <8-10 mild, 10-18 moderate, >18 severe.
- Symptoms: Autonomic hyperactivity (↑HR, ↑BP), tremors, anxiety.
- Severe: Seizures, hallucinations, Delirium Tremens (DTs).
- 📌 Mnemonic for DT symptoms: "FATAL DT" - Fever, Autonomic hyperactivity, Tremors, Agitation/Altered mental status, Leukocytosis, Delirium Tremens.
⭐ Delirium Tremens (DTs) is a medical emergency characterized by global confusion, sympathetic overdrive, and has a mortality rate of 5-15% if untreated. Onset 48-96 hours post-last drink.
Chronic Complications - Body's Booze Battle
- Liver: Steatosis → alcoholic hepatitis → cirrhosis.
- GI: Gastritis, pancreatitis, Mallory-Weiss tear.
- CV: Alcoholic cardiomyopathy, hypertension.
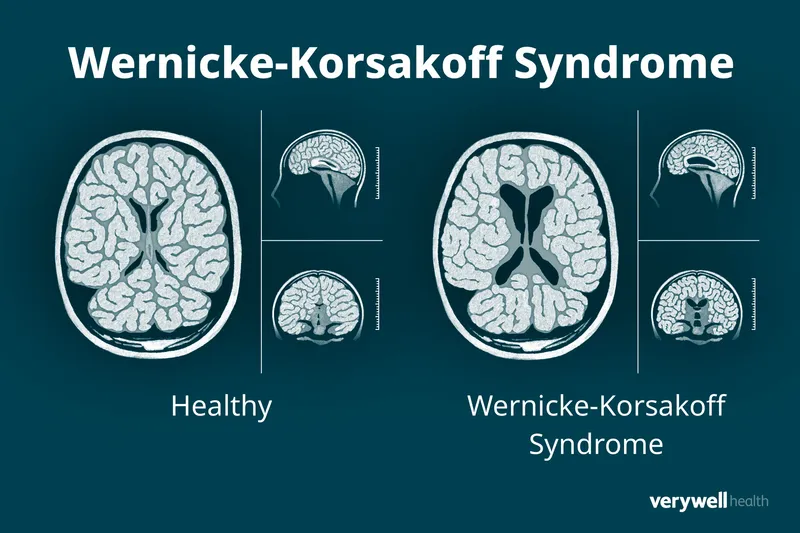
- Neuro: Wernicke-Korsakoff syndrome, cerebellar degeneration, peripheral neuropathy.
- 📌 Wernicke's triad ("COAT"): Confusion, Ophthalmoplegia, Ataxia, Thiamine deficiency.
- Treat Wernicke's: Thiamine 100-500mg IV/IM TID.
- Cancers: Oropharyngeal, esophageal, liver, laryngeal.
| Feature | Wernicke's Encephalopathy (WE) | Korsakoff's Psychosis (KP) |
|---|---|---|
| Presentation | Acute: Confusion, Ophthalmoplegia, Ataxia | Chronic: Amnesia (antero/retro), Confabulation, Apathy |
| Thiamine Response | Reversible | Often irreversible memory loss |
 oka
oka
Management Strategies - Treatment Toolkit
- Withdrawal Management: BZD (e.g., Diazepam, Lorazepam) via CIWA-Ar.
- Relapse Prevention Pharmacotherapy:
Drug MOA Key SE CIs Dose (Oral) Naltrexone Opioid antag; ↓cravings Nausea, HA, hepatotox (rare) Active opioids, liver fail. 50mg/day Acamprosate GABA/glutamate mod; ↓withdrawal Diarrhea Sev. renal impair (CrCl <30mL/min) 666mg TID Disulfiram Aldehyde DH inhib; aversive Metallic taste, neuropathy Cardiac dis, psychosis, alcohol use, preg. 250-500mg/day 📌 For Disulfiram reaction: "Don't Ingest Sulfiram Like Alcohol Makes Nasty Vomiting" - Dyspnea, Itching, Sweating, Lightheadedness, Angina, Nausea, Vomiting. - Psychosocial Support: MI, CBT, AA.
Pharmacotherapy Selection Algorithm:
⭐ Naltrexone is contraindicated in patients receiving opioid analgesics or with acute hepatitis/liver failure, while Acamprosate is preferred in liver disease but needs dose adjustment in renal impairment.
High‑Yield Points - ⚡ Biggest Takeaways
- CAGE questionnaire is a key screening tool for Alcohol Use Disorder (AUD).
- Wernicke-Korsakoff syndrome results from thiamine (B1) deficiency in chronic alcohol use.
- Delirium Tremens (DTs) is a severe, life-threatening alcohol withdrawal, treat with benzodiazepines.
- Naltrexone, acamprosate, and disulfiram are first-line pharmacotherapies for AUD.
- An AST:ALT ratio > 2:1 strongly suggests alcoholic liver disease.
- Fetal Alcohol Syndrome (FAS) causes distinct craniofacial dysmorphism and neurodevelopmental issues.
- Marchiafava-Bignami disease, a rare complication, involves corpus callosum demyelination.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

