Introduction & Epidemiology - Cancer's Early Clues
- Breast cancer: Leading malignancy in Indian women; incidence rising, particularly in urban areas. Accounts for significant morbidity.
- Early detection through screening is crucial for improved prognosis and survival rates.
- Indian scenario:
- Peak incidence: 40-50 years (a decade earlier than Western counterparts).
- Presentation often at locally advanced stages, leading to poorer outcomes.
- Screening goal: Identify asymptomatic, early-stage, curable disease.
- Primary modalities: Mammography, Clinical Breast Examination (CBE), Breast Self-Examination (BSE).
⭐ Mammography remains the only screening modality proven to reduce breast cancer mortality, by up to 20-30% in organized screening programs for women aged 50-69 years old.
Mammography - X-Ray Vision
- Primary screening tool for breast cancer; uses low-dose X-rays.
- Standard Views:
- Cranio-Caudal (CC)
- Medio-Lateral Oblique (MLO) - visualizes most breast tissue, including axillary tail.
- Technique: Breast compression is crucial for ↓ radiation dose, ↑ image quality, ↓ motion blur.
- Types:
- Full-Field Digital Mammography (FFDM).
- Digital Breast Tomosynthesis (DBT/3D): ↑ cancer detection, ↓ recall rates, especially in dense breasts.

- Key Malignant Signs:
- Spiculated masses.
- Suspicious microcalcifications (e.g., pleomorphic, fine linear, branching/casting type).
- Architectural distortion.
- Developing asymmetry.
- Reporting: BI-RADS (Breast Imaging Reporting and Data System) for standardized assessment and risk stratification.
⭐ DBT (3D Mammography) significantly improves cancer detection rates by 1-2 per 1000 screened and reduces false positives, particularly in women with dense breast tissue.
BI-RADS & Other Modalities - Decoding Reports
-
BI-RADS (Breast Imaging Reporting & Data System): Standardized lexicon for mammography, USG, MRI.
- 0: Incomplete - Needs more views/USG.
- 1: Negative - Routine screen.
- 2: Benign - Routine screen.
- 3: Probably Benign - 6-month follow-up; <2% malignancy risk.
- 4: Suspicious (4A-low, 4B-mod, 4C-high) - Biopsy.
- 5: Highly Suggestive of Malignancy (>95% risk) - Biopsy.
- 6: Known Malignancy - Treatment planning.
-
Other Modalities:
- Ultrasound (USG): Dense breasts, cyst/solid differentiation, palpable lumps, biopsy guidance.
- MRI: High-risk screen (BRCA, >20% lifetime risk), staging, problem-solving, implants.
- Tomosynthesis (3D Mammo): ↑Cancer detection, ↓recalls, esp. dense breasts.
- CEM (Contrast-Enhanced Mammography): Emerging; indications similar to MRI (staging, problem-solving).
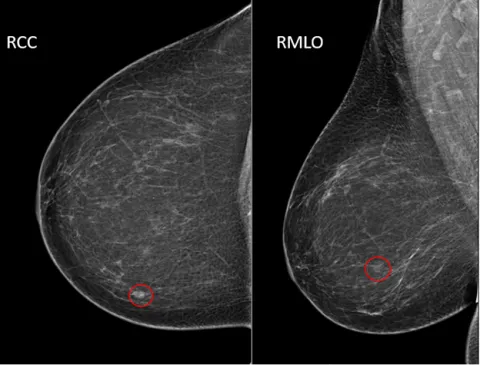
⭐ BI-RADS 3 lesions have a <2% likelihood of malignancy; typically managed with short-interval (6-month) follow-up rather than immediate biopsy.
Screening Guidelines (India) - When & Who
- Opportunistic Screening: No national program. Emphasis on awareness.
- Average Risk Women:
- Age 20+: Monthly Breast Self-Examination (BSE).
- Age 40-49: Individualized decision for mammography (annual/biennial). Clinical Breast Exam (CBE) recommended.
- Age 50-74: Mammography every 1-2 years. Annual CBE.
- Age ≥75: Discuss with doctor; decision based on health status.
- High-Risk Women: (e.g., BRCA mutation, strong family history)
- Earlier screening: Start mammography by age 25-30 or 10 years before youngest family case.
- Annual mammography; consider annual MRI.
⭐ Many Indian breast cancers present at a younger age (40-50 years) compared to Western countries, impacting screening considerations.
High‑Yield Points - ⚡ Biggest Takeaways
- Screening mammography is the primary tool for early breast cancer detection.
- BI-RADS classification is crucial for standardized mammography reporting.
- Screening typically begins at age 40-50 years; frequency varies.
- High-risk individuals (e.g., BRCA mutation) need earlier screening, often with MRI.
- Digital Breast Tomosynthesis (DBT) improves cancer detection, especially in dense breasts.
- Triple assessment (clinical exam, imaging, biopsy) is key for symptomatic patients, not for screening asymptomatic women.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

