LLD: Basics - Defining Despair
- Definition: Major Depressive Disorder (MDD) or clinically significant depressive symptoms with onset at age ≥60-65 years.
- Significance:
- Common, yet often underdiagnosed & undertreated.
- Impact: ↑ morbidity, ↑ mortality, ↓ Quality of Life (QoL).
- Epidemiology:
- Prevalence:
- Community: 1-5% (MDD), 10-15% (depressive symptoms).
- Primary Care: 5-10%.
- Long-term Care Facilities: 12-30%.
- Gender: Higher prevalence in women (F > M).
- Prevalence:
⭐ Late-life depression is a significant risk factor for developing dementia.
LLD: Origins - Unraveling Roots
LLD's etiology is multifactorial, understood via a Biopsychosocial model:
- Biological Factors:
- Neurotransmitter changes (↓ Serotonin, ↓ Norepinephrine, ↓ Dopamine)
- HPA axis dysregulation (often ↑ cortisol)
- Genetic predisposition (e.g., family history)
- Cerebrovascular disease ('vascular depression' hypothesis)
- Linked to white matter hyperintensities (WMHs)
- Chronic inflammation (e.g., ↑ pro-inflammatory cytokines)
- Structural brain changes (e.g., cortical atrophy, WMHs)
- Psychosocial Factors:
- Chronic medical illness, disability, chronic pain
- Polypharmacy (adverse effects, interactions)
- Bereavement, social isolation, loneliness
- Financial strain, caregiver burden
- Past trauma or significant life stressors
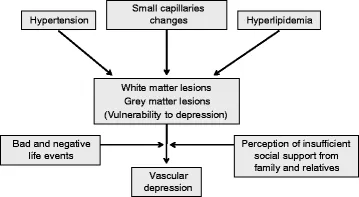
⭐ The 'vascular depression' hypothesis posits that cerebrovascular lesions disrupt fronto-striatal-limbic pathways, increasing vulnerability to depression.
LLD: Presentation & Diagnosis - Spotting Shadows
- Core Symptoms (📌 SIGECAPS): DSM-5: ≥5 symptoms for ≥2 weeks (must include depressed mood or anhedonia).
- Sleep disturbance
- Interest ↓ (anhedonia)
- Guilt/worthlessness
- Energy ↓ (fatigue)
- Concentration ↓
- Appetite change/weight change
- Psychomotor agitation/retardation
- Suicidal ideation
- Atypical Presentations:
- Prominent somatic complaints (pain, GI upset), anxiety, irritability, apathy.
- Cognitive impairment ('depressive pseudodementia'), social withdrawal. Less overt sadness.
- Diagnosis:
- DSM-5/ICD-11 criteria.
- Screening: Geriatric Depression Scale (GDS-15 >5), PHQ-9 (>10).
- Differential Diagnosis:
- Dementia (Alzheimer's, Vascular), Delirium.
- Medical: Hypothyroidism, Parkinson's. Medication side effects.
⭐ In 'depressive pseudodementia', cognitive deficits often improve significantly with antidepressant treatment, unlike in true dementia where decline is progressive.
LLD: Management & Prognosis - Guiding Lights
General Principles:
- "Start low, go slow."
- Monitor side effects (e.g., hyponatremia with SSRIs, QTc prolongation, fall risk) & drug interactions.
Pharmacotherapy:
- First-line: SSRIs (e.g., Sertraline 25-50mg, Escitalopram 5-10mg).
- SNRIs (Venlafaxine, Duloxetine) as alternatives.
- Avoid TCAs, MAOIs if possible.
- Consider augmentation for partial response.
Psychotherapy:
- Problem-Solving Therapy (PST), Interpersonal Therapy (IPT), Cognitive Behavioral Therapy (CBT).
- Effective alone or combined with medication.
Electroconvulsive Therapy (ECT):
- For severe, treatment-resistant, psychotic depression, or urgent need (suicidality, inanition).
⭐ ECT is a safe, highly effective treatment for severe LLD, even in frail elderly, with precautions.
Other: Lifestyle modifications, social support.
Prognosis:
- Variable; ↑relapse, chronicity. Comorbidities impact. ⚠️ High suicide risk.
Treatment Algorithm:
High‑Yield Points - ⚡ Biggest Takeaways
- Late-life depression often presents with somatic symptoms, anxiety, not just overt sadness.
- Strong link to vascular risk factors, cerebrovascular disease (vascular depression).
- ↑ risk of cognitive impairment, dementia; consider pseudodementia.
- SSRIs first-line (start low, go slow); ECT safe, effective for severe/resistant cases.
- Higher suicide risk, particularly in older, isolated males.
- Often co-occurs with chronic medical illnesses, polypharmacy.
- Differentiate from normal bereavement, adjustment disorders.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

