Pharmacogenetics Basics - Gene-Drug Dance Intro
- Pharmacogenetics (PGt): How single genes affect drug response; specific gene-drug interactions.
- Pharmacogenomics (PGx): Broader; how genome (all genes) affects drug response.
- Goal: Tailor drug choice & dose to individual genetic makeup.
- Maximise efficacy.
- Minimise adverse drug reactions (ADRs).
- Foundation of Personalized Medicine: Right drug, right dose, right patient.
- Genetic variations (e.g., SNPs) alter drug ADME & drug targets.
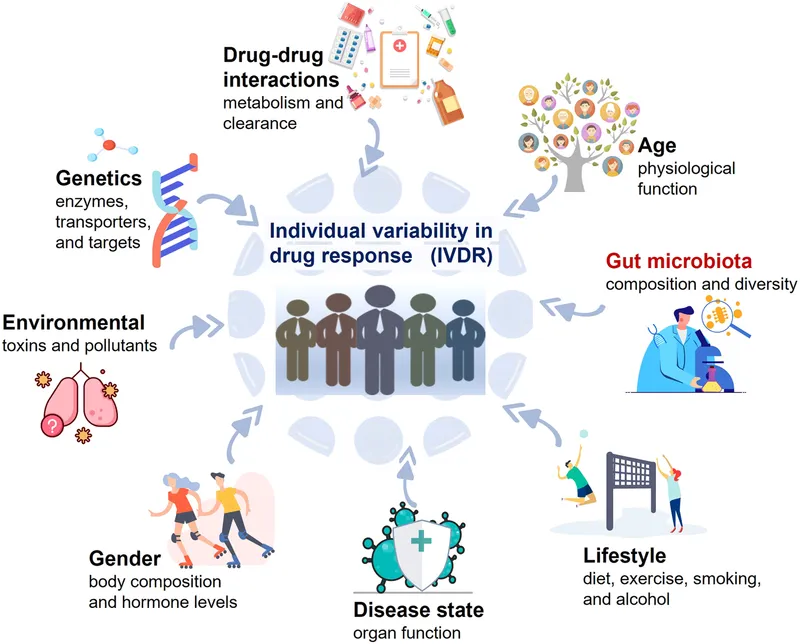
⭐ PGt/PGx aims to predict if a drug will be effective or cause side effects before it's prescribed.
Genetic Variations - DNA's Drug Twists
- Principle: Inherited DNA sequence changes cause inter-individual differences in drug response.
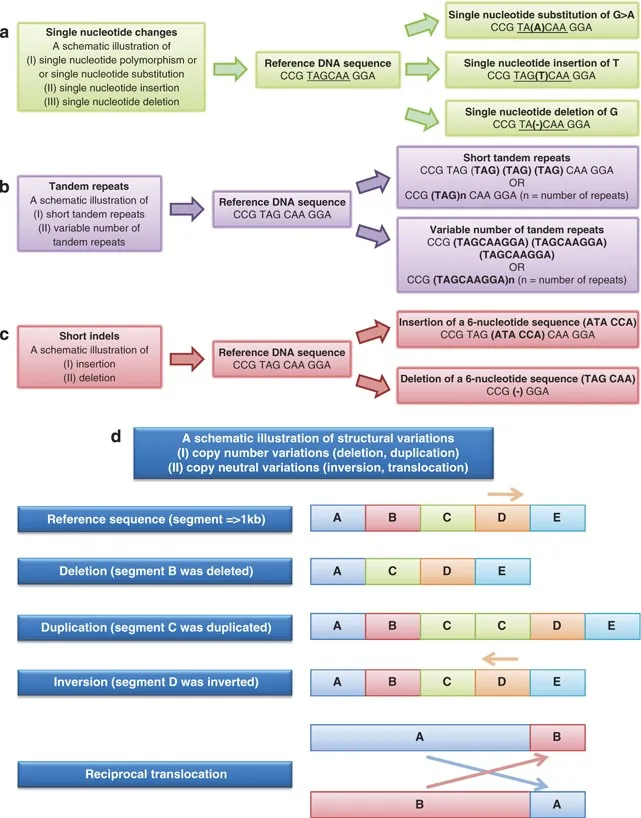
- Major Types of Variations:
- SNPs (Single Nucleotide Polymorphisms): Most frequent; single base-pair substitutions (e.g., C→T).
- Indels: Small insertions or deletions of DNA bases.
- CNVs (Copy Number Variations): Duplication or deletion of larger DNA segments, affecting gene dosage.
- Consequences:
- Altered drug metabolism (e.g., CYP enzymes).
- Modified drug transporter function.
- Changes in drug target sensitivity.
⭐ TPMT gene variations: Predict thiopurine (e.g., azathioprine, 6-mercaptopurine) toxicity. Low TPMT activity leads to ↑ risk of myelosuppression.
Key Pathways & Players - Metabolism's Genetic Code
- Cytochrome P450 (CYPs): Key drug metabolizers.
- CYP2D6: Codeine (↓ analgesia), tamoxifen (↓ efficacy).
- CYP2C9: Warfarin (↑ bleeding risk with *2, *3 variants).
- CYP2C19: Clopidogrel (↓ effect with *2, *3; "resistance").
- Other Enzymes:
- TPMT (Thiopurine S-Methyltransferase): Azathioprine, 6-MP (↑ myelosuppression with low activity).
- UGT1A1: Irinotecan (↑ toxicity with *28 allele), bilirubin.
- Transporters:
- SLCO1B1 (OATP1B1): Statins (simvastatin, ↑ myopathy with 521T>C).
- ABCB1 (MDR1/P-glycoprotein): Digoxin (altered levels).
⭐ TPMT testing is crucial before initiating thiopurines (azathioprine, 6-MP) to prevent severe myelosuppression in deficient individuals.
Clinical Applications - Genes Guiding Doses
- Warfarin: CYP2C9 (metabolism) & VKORC1 (sensitivity) variants guide dose.
- ↓ function alleles require ↓ dose to reduce bleeding risk.
- Clopidogrel: CYP2C19 activates prodrug.
- Poor metabolizers (PMs): ↓ efficacy, ↑ MACE. Alt: prasugrel, ticagrelor.
- Abacavir: HLA-B*5701 testing mandatory.
- Positive: high HSR risk; contraindicated.
⭐ HLA-B*1502 screening in Asians for Carbamazepine is crucial to prevent SJS/TEN.
- Azathioprine/6-MP: TPMT/NUDT15 variants affect metabolism.
- ↓ enzyme activity: ↑ myelosuppression risk. Dose reduction vital.
- Codeine: CYP2D6 metabolizes to morphine.
- Ultra-rapid metabolizers (UMs): ↑ toxicity risk. Poor metabolizers (PMs): ↓ analgesia.
Future & Hurdles - Tailored Meds Ahead
- Future Scope:
- AI/ML for drug development & patient selection
- Polygenic Risk Scores (PRS) for disease prediction
- Advanced gene editing (e.g., CRISPR)
- Seamless PGx data integration in EHRs
- Key Hurdles:
- Ethical, Legal, Social Implications (ELSI)
- High costs & reimbursement issues
- Clinical implementation & workforce training
- Data security & privacy concerns
- Managing complex gene-environment interactions
⭐ Pre-treatment screening for HLA-B*5701 is crucial to prevent abacavir hypersensitivity.
High‑Yield Points - ⚡ Biggest Takeaways
- Genetic variations (e.g., SNPs, CYP2D6, TPMT) significantly alter drug efficacy and toxicity.
- CYP2D6 polymorphisms impact metabolism of codeine, tamoxifen, and many beta-blockers.
- TPMT deficiency ↑ mercaptopurine toxicity (e.g., myelosuppression); genotyping crucial.
- Warfarin dosing is guided by CYP2C9 & VKORC1 variants for optimal anticoagulation.
- HLA-B*5701 screening is vital before abacavir to prevent severe hypersensitivity.
- Clopidogrel efficacy ↓ in CYP2C19 poor metabolizers.
- Personalized medicine optimizes drug therapy using an individual's genetic profile.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

