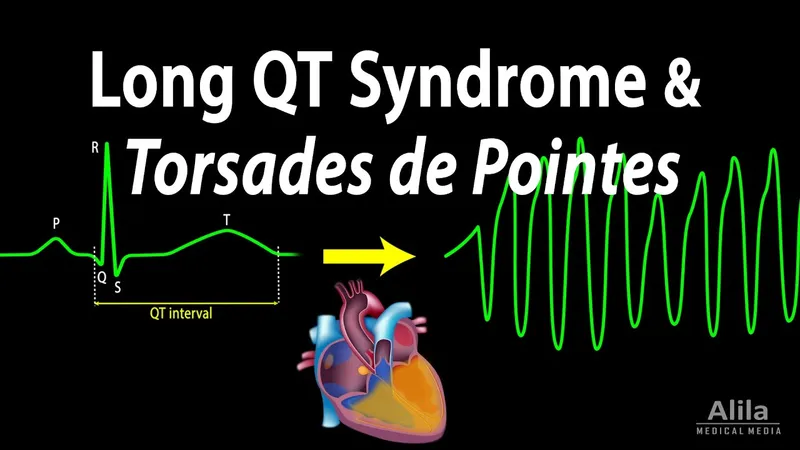
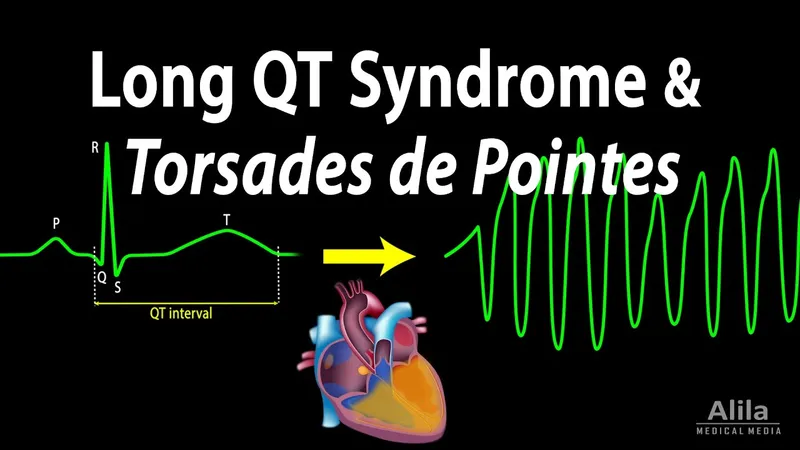
QT Interval & TdP - Electric Heartbeat Hiccups
- QT Interval: ECG: Start of QRS to end of T wave. Represents ventricular repolarization; duration varies with heart rate.
- Corrected QT (QTc): Adjusts QT for heart rate.
- Bazett's Formula: $QTc = QT / \sqrt{RR}$.
- Prolonged QTc thresholds (risk of TdP):
- Men: > 450ms
- Women: > 470ms
- Very High Risk for TdP: QTc > 500ms.
- Torsades de Pointes (TdP):
- Life-threatening polymorphic ventricular tachycardia.
- Triggered by QT prolongation.
- ECG: 'Twisting of points' appearance.
⭐ Torsades de Pointes (TdP) is a polymorphic ventricular tachycardia specifically associated with QT prolongation, appearing as a 'twisting of points' on ECG.
Causative Drugs - Pharma's QT Stretchers
Many drugs prolong QT, risking Torsades de Pointes (TdP). Key classes:
| Drug Class | Examples |
|---|---|
| Antiarrhythmics | Class IA (Quinidine, Procainamide, Disopyramide), Class III (Amiodarone, Sotalol, Dofetilide, Ibutilide) |
| Antibiotics | Macrolides (Erythromycin, Clarithromycin, Azithromycin), Fluoroquinolones (Ciprofloxacin, Levofloxacin, Moxifloxacin) |
| Antipsychotics | Haloperidol, Thioridazine, Ziprasidone, Risperidone, Olanzapine |
| Antidepressants | TCAs (Amitriptyline, Imipramine), SSRIs (Citalopram, Escitalopram) |
| Antiemetics | Ondansetron, Domperidone, Droperidol |
| Antifungals | Azoles (Fluconazole, Ketoconazole, Itraconazole) |
| Others | Methadone, Chloroquine, Hydroxychloroquine, Cisapride, Sumatriptan |
- Antiarrhythmics (Class IA, III)
- AntiBiotics (Macrolides, Quinolones)
- AntiCychotics (e.g., Haloperidol)
- AntiDepressants (TCAs, SSRIs)
- AntiEmetics (e.g., Ondansetron)
⭐ Many non-antiarrhythmic drugs, such as macrolide antibiotics (e.g., erythromycin), fluoroquinolones, antipsychotics (e.g., haloperidol), and ondansetron, are notorious for causing QT prolongation.
Risk Factors - Dodging Danger Zones
- Patient-Specific Vulnerabilities:
- Female gender, advanced age (>65 yrs)
- Genetic predisposition (e.g., congenital LQTS variants)
- Underlying structural heart disease (e.g., MI, HF, LVH)
- Baseline bradycardia or AV block
- Modifiable/External Factors:
- Polypharmacy: multiple QT-prolonging agents
- Drug interactions (e.g., CYP3A4 inhibitors)
- Rapid IV administration of offending drugs
- Renal or hepatic impairment (↓ drug clearance)
⭐ Electrolyte abnormalities, particularly hypokalemia and hypomagnesemia, are major predisposing factors that significantly potentiate drug-induced QT prolongation and risk of TdP.
Clinical Picture & Management - Taming Torsades Twists
- Presentation: Often asymptomatic. Palpitations, dizziness, syncope; can lead to Sudden Cardiac Death (SCD).
- ECG: QTc >450ms (males), >470ms (females); >500ms = high risk. Torsades de Pointes (TdP): characteristic polymorphic VT, "twisting of points".
- Management Algorithm:
⭐ Intravenous Magnesium Sulfate is the first-line treatment for Torsades de Pointes, even in patients with normal serum magnesium levels.
- Key Interventions: Discontinue culprit agent. Aggressively replete K⁺ (target 4.5-5.0 mEq/L) and Mg²⁺. Monitor ECG continuously during acute phase.
- QT prolongation indicates delayed ventricular repolarization, risking Torsades de Pointes (TdP).
- Critical risk factors: female sex, hypokalemia, hypomagnesemia, bradycardia, structural heart disease.
- Common drug classes: Antiarrhythmics (IA, III), antipsychotics, macrolides, fluoroquinolones, azole antifungals, ondansetron.
- Main mechanism: Blockade of the IKr (hERG) potassium channel.
- TdP treatment: Discontinue drug, correct electrolytes (K+, Mg2+), IV magnesium sulfate.
- QTc monitoring is crucial; Bazett's formula (QTc = QT/√RR) is often used.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

