TORCH Infections Intro - Prenatal Peril Primer
- Congenital infections: Infections transmitted from mother to child during pregnancy (prenatal) or around childbirth (perinatal).
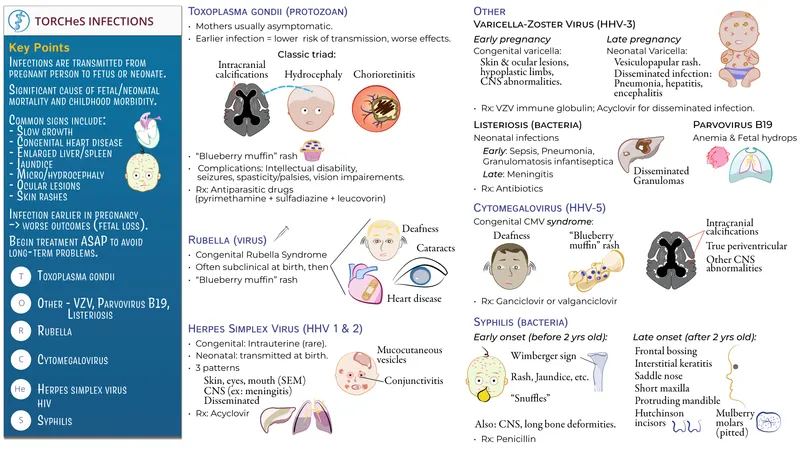
- 📌 TORCH complex: A group of common, significant congenital pathogens:
- Toxoplasmosis
- Other (e.g., Syphilis, Varicella-Zoster, Parvovirus B19, Zika)
- Rubella
- Cytomegalovirus (CMV)
- Herpes Simplex Virus (HSV)
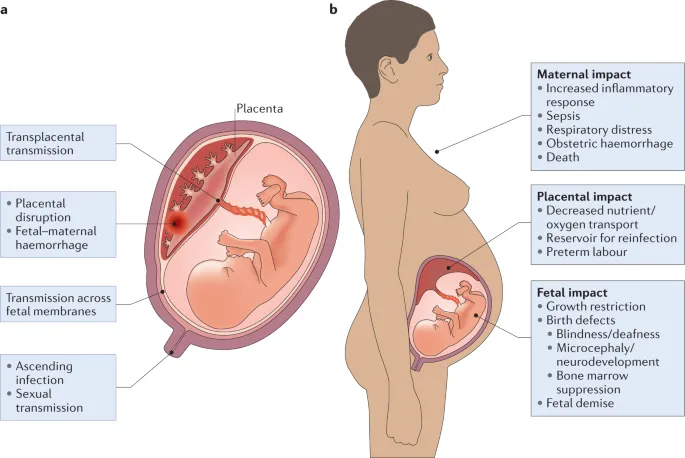
- Transmission routes:
- Transplacental (hematogenous spread across placenta)
- Perinatal (ascending infection or during passage through birth canal)
- Timing vs. Severity: Earlier gestational infection (especially <16-20 weeks or 1st trimester) often leads to ↑ severe fetal outcomes.
⭐ Cytomegalovirus (CMV) is the most common congenital viral infection globally.
Toxoplasmosis & Rubella - Parasite & Rash Pair
| Feature | Toxoplasmosis | Rubella (German Measles) |
|---|---|---|
| Agent | Toxoplasma gondii (parasite) | Rubella virus (Togavirus) |
| Key Features | 📌 Triad: Chorioretinitis, Hydrocephalus, Intracranial calcifications (diffuse). Rash, hepatosplenomegaly. | 📌 Triad: Cataracts, Deafness (sensorineural), Cardiac defects (PDA, PPS). "Blueberry muffin" rash. IUGR. |
| Diagnosis | Serology (IgM, IgG); PCR (amniotic fluid). Head US/CT. | Serology (IgM, IgG); PCR (nasopharyngeal, urine, amniotic fluid). |
| Management | Pyrimethamine + Sulfadiazine + Folinic acid (for 1 year). | Symptomatic; supportive care. Early intervention for defects. |
| Prevention | Avoid raw meat, cat litter. Spiramycin (if acute maternal infection). | MMR vaccine (pre-pregnancy). Avoid pregnancy for 1 month post-vaccination. |
⭐ Congenital Rubella Syndrome (CRS) risk is highest (up to 90%) if maternal infection occurs in the first 10-12 weeks of gestation.
CMV & HSV - Viral Villains Unveiled
⭐ Sensorineural hearing loss (SNHL) is the most common long-term sequela of congenital CMV infection.
| Feature | Cytomegalovirus (CMV) | Herpes Simplex Virus (HSV) |
|---|---|---|
| Agent | DNA virus (Herpesviridae) | DNA virus (Herpesviridae) |
| Key Features | - Periventricular calcifications - Sensorineural hearing loss (SNHL) - Chorioretinitis, microcephaly - Hepatosplenomegaly, petechiae | - Skin, Eye, Mouth (SEM): vesicular lesions - CNS: seizures, encephalitis - Disseminated: multi-organ, sepsis-like |
| Diagnosis | - Urine/saliva PCR or culture (within 3 weeks of birth) | - PCR from lesions, CSF, blood; Viral culture |
| Management | - Ganciclovir / Valganciclovir (symptomatic CNS/severe) | - Acyclovir IV (14-21 days) |
| Prevention | - Strict hygiene; Screen blood/organ donors | - Maternal acyclovir (3rd trimester if recurrent); C-section if active genital lesions |
| Mnemonic | 📌 Most common congenital infection. | 📌 Acyclovir is key for treatment. |
Syphilis & Others - Spirochete & Sundry Syndromes
-
Congenital Syphilis (T. pallidum):
- Early (<2 yrs): Snuffles (rhinitis), maculopapular rash (palms/soles), hepatosplenomegaly, osteochondritis (Parrot's pseudoparalysis), condyloma lata.
- Late (>2 yrs): 📌 Hutchinson's triad (Interstitial keratitis, Peg-shaped incisors, 8th nerve deafness), mulberry molars, saber shins, Clutton's joints.
⭐ "Snuffles" (copious nasal discharge) is often the earliest and most characteristic sign of congenital syphilis.
- Dx: VDRL/RPR; confirm FTA-ABS. Darkfield microscopy. X-ray long bones (osteochondritis, periostitis).
- Mgmt: Penicillin G.
-
Other Congenital Infections:
- VZV (Varicella): Limb hypoplasia, cicatricial skin lesions (zig-zag), chorioretinitis, microcephaly. Risk: maternal infection 1st/2nd trimester.
- Parvovirus B19: Hydrops fetalis, severe anemia, aplastic crisis.
- HIV: Risk ↓ with maternal ART. Dx: HIV DNA/RNA PCR (not Ab <18mo). Prophylaxis: Nevirapine/Zidovudine.
- Zika Virus: Microcephaly, intracranial calcifications, ocular abnormalities, arthrogryposis.
High‑Yield Points - ⚡ Biggest Takeaways
- CMV: Most common congenital infection; key features include periventricular calcifications, microcephaly, and sensorineural hearing loss (SNHL).
- Toxoplasmosis: Presents with the classic triad of chorioretinitis, hydrocephalus, and diffuse intracranial calcifications.
- Rubella: Characterized by cataracts, SNHL, patent ductus arteriosus (PDA), and often a "blueberry muffin" rash.
- Congenital Syphilis: Early signs include snuffles and maculopapular rash; late stigmata include Hutchinson teeth and saber shins.
- Neonatal HSV: Manifests with skin vesicles, keratoconjunctivitis, and seizures; disseminated disease has high mortality.
- Parvovirus B19: Can lead to hydrops fetalis, severe anemia, and pure red cell aplasia in the fetus/newborn.
- Zika Virus: Associated with microcephaly and other severe fetal brain defects; can also cause Guillain-Barré syndrome in adults/children.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

