Non-Cicatricial Alopecias - Hair Today Gone Tomorrow
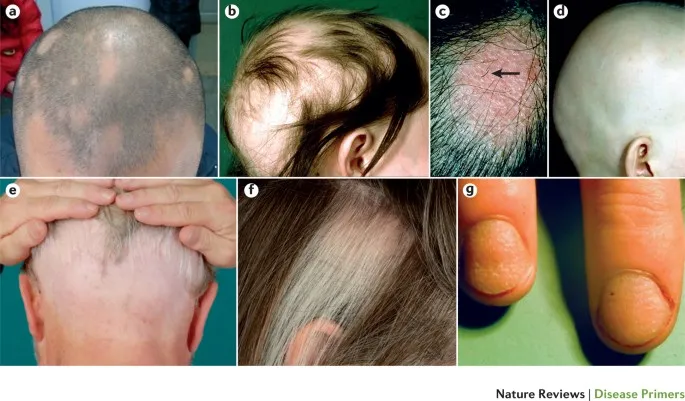
| Feature | Androgenetic Alopecia (AGA) | Alopecia Areata (AA) | Telogen Effluvium (TE) |
|---|---|---|---|
| Key Features | Gradual, patterned loss (Hamilton-Norwood/Ludwig); follicular miniaturization | Autoimmune; patchy/total loss (ophiasis); nail pitting; exclamation mark hairs | Acute, diffuse shedding 2-3 months post-trigger; +ve pull test |
| Histology | ↑Telogen hairs, miniaturized follicles, ↓anagen:telogen ratio | Peribulbar lymphocytic infiltrate ("swarm of bees") | ↑Telogen hairs (>20-25%); no significant inflammation |
| Treatment Pearls | Minoxidil, Finasteride (males), Spironolactone (females) | Corticosteroids (topical/IL/systemic), immunotherapy | Address trigger, reassurance, topical Minoxidil |
Cicatricial Alopecias & Hair Shaft - Scarred Scalps Snapped Strands
Permanent hair loss due to follicle destruction and scarring. Key types:
| Feature | Lichen Planopilaris (LPP) | DLE (Scalp) | Folliculitis Decalvans (FD) |
|---|---|---|---|
| Clinical | Perifollicular erythema/scaling. Frontal Fibrosing Alopecia (FFA) variant. | Erythematous plaques, atrophy, follicular plugging, dyspigmentation. | Chronic pustules, crusts. 'Tufted folliculitis' (polytrichia). |
| Histology | Lymphocytic interface/bulge infiltrate, perifollicular lamellar fibrosis, vacuolar alteration. Loss of sebaceous glands. | Epidermal atrophy, follicular plugging, interface dermatitis, thickened basement membrane, dermal mucin. | Early: neutrophilic perifollicular abscess. Late: lymphoplasmacytic infiltrate, plasma cells, fibrosis. |
| Distinguishing | Lonely hairs, loss of follicular openings. | Carpet tack sign. Photosensitivity. | Often S. aureus. Boggy, tender scalp. |
⭐ 'Tufted folliculitis' is characteristic of Folliculitis Decalvans.
Hair shaft defects (e.g., Trichorrhexis Nodosa) cause brittle hair, snapped strands, usually non-scarring.
Nail Infections & Anatomy - Fungal Fingers Toe Troubles
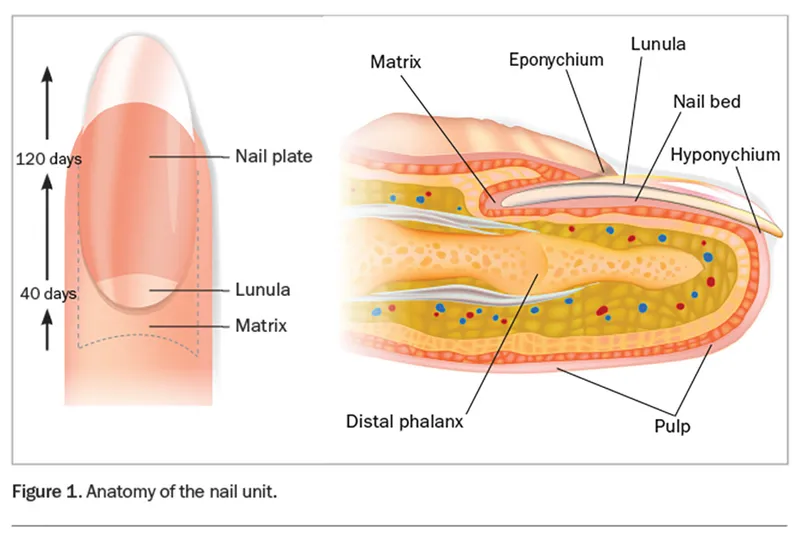 and paronychia)
and paronychia)
- Nail Anatomy: Plate, bed, matrix (growth), nail folds (proximal/lateral), eponychium (cuticle), hyponychium.
- Onychomycosis (Tinea Unguium): Fungal nail infection.
Type Organism(s) Highlights Key Feature(s) DLSO T. rubrum (most common) Distal/lateral entry, subungual hyperkeratosis WSO T. mentagrophytes Superficial white patches on nail plate PSO T. rubrum, Candida (HIV assoc.) Proximal entry, cuticle; immunocompromised TDO End-stage of others Total nail destruction, thickened - Paronychia: Nail fold inflammation.
- Acute: Bacterial (S. aureus, Strep.). <6 wks. Rapid pain, erythema, pus. Tx: Warm soaks, antibiotics.
- Chronic: Candida albicans, irritants. >6 wks. Boggy, tender folds, nail dystrophy. Tx: Avoid irritants, antifungals.
⭐ Trichophyton rubrum is the most common dermatophyte causing onychomycosis worldwide.
Nail Disease & Tumors - Nail Clues Nasty Knots
-
Nail Psoriasis vs. Lichen Planus (LP):
Feature Psoriasis Lichen Planus (LP) Pitting Irregular, deep Fine, rare Onycholysis Common, "oil drop" Common Subungual Hyperkeratosis Common Common Pterygium Absent Present (dorsal, classic) 
-
Key Nail Lines & Associations:
- Beau's lines: Transverse grooves; severe illness, chemo.
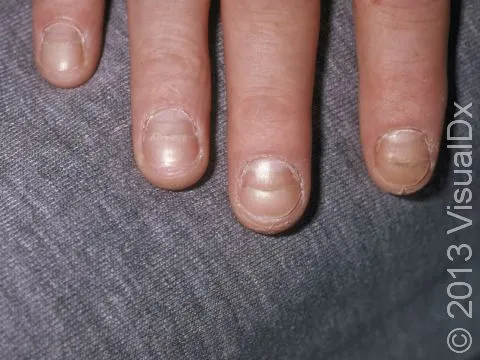
- Mees' lines: Transverse white bands; arsenic, renal failure.
- Muehrcke's lines: Paired white bands (nail bed); hypoalbuminemia.
- Beau's lines: Transverse grooves; severe illness, chemo.
-
Other Important Changes:
- Clubbing: Lovibond angle >180°; lung disease, cyanotic heart disease.
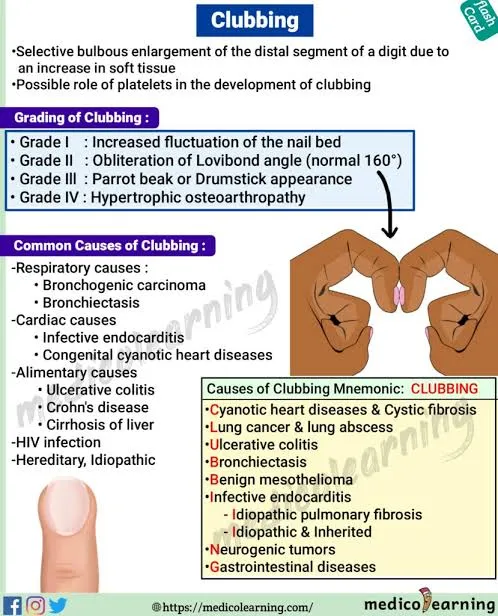
- Koilonychia: Spoon nails; iron deficiency.
- Onycholysis: Nail plate separation from bed.
- Paronychia: Nail fold inflammation (acute/chronic).
- Onychomycosis: Fungal; thick, discolored.
- Clubbing: Lovibond angle >180°; lung disease, cyanotic heart disease.
-
Melanonychia Evaluation: (📌 ABCDEF rule for melanoma)
> ⭐ Hutchinson's sign (pigment on proximal/lateral nail fold) is a red flag for subungual melanoma. 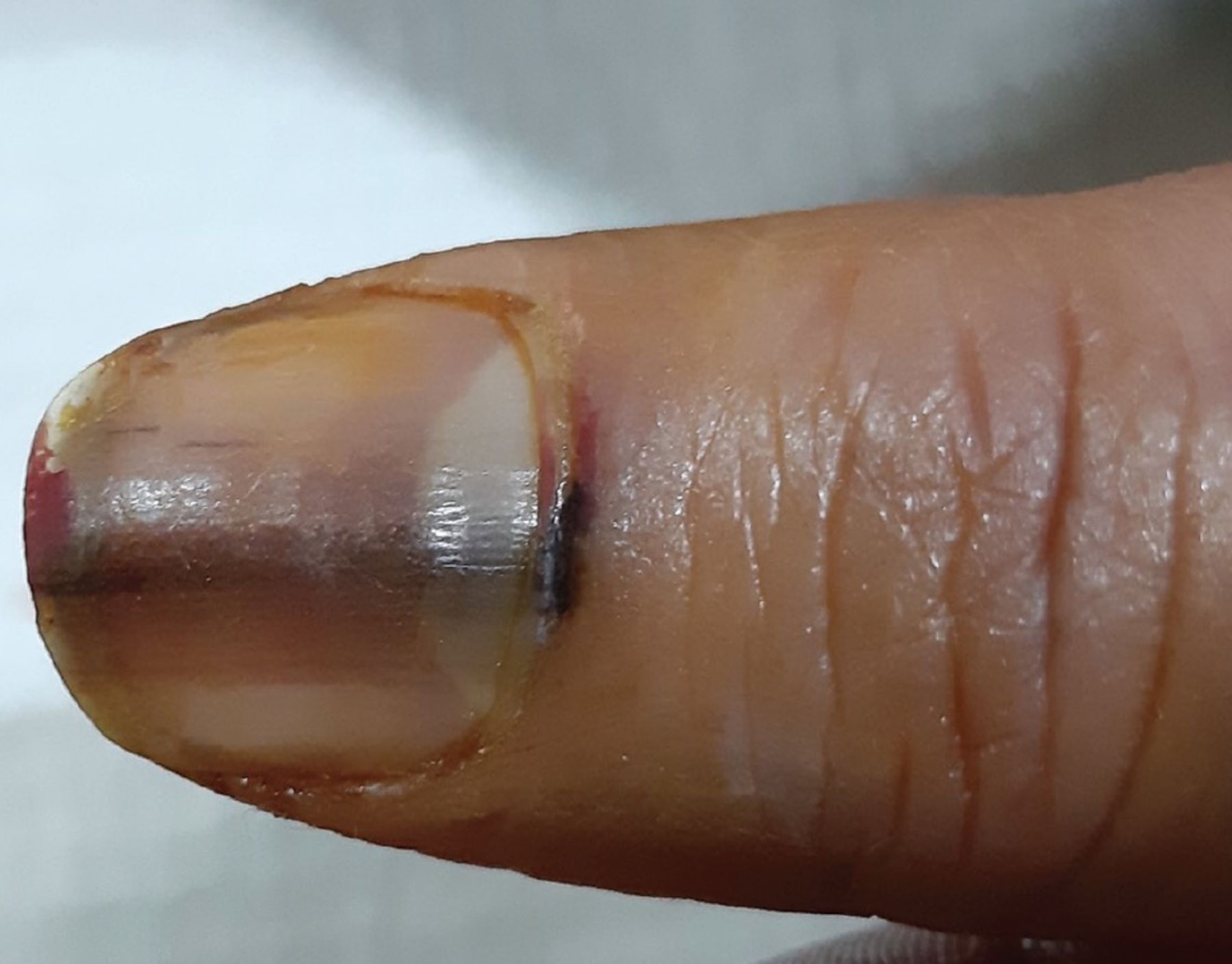
- Nail Tumors:
- Glomus tumor: TRIAD - severe pain, cold sensitivity, localized tenderness. Bluish.
- Subungual melanoma: Often melanonychia; check Hutchinson's sign.
High‑Yield Points - ⚡ Biggest Takeaways
- Alopecia Areata: Peribulbar lymphocytic infiltrate ("swarm of bees") is characteristic.
- Androgenetic Alopecia: Shows hair follicle miniaturization and ↑ telogen hairs.
- Lichen Planopilaris: Follicular interface dermatitis and fibrosis cause scarring alopecia.
- Tinea Capitis: Fungal elements (endothrix/ectothrix) in hair; PAS stain confirms.
- Nail Psoriasis: Oil spots, pitting, onycholysis; neutrophils in nail plate (Munro's).
- Onychomycosis: Fungal hyphae in nail plate/bed; PAS stain is diagnostic.
- DLE: May cause scarring alopecia with follicular plugging, interface changes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

