Preoperative Assessment & Principles - Pre-Op Game Plan
- History: Voiding diary (≥3 days), POP-Q, symptom scores (e.g., UDI-6, IIQ-7), obstetric/surgical history.
- Examination: Pelvic exam (assess prolapse stage, levator ani function), cough stress test, Q-tip test (urethral hypermobility).
- Investigations: Urinalysis, urine culture. Consider urodynamics (UDS) for complex cases or prior failed surgery.
- Counseling & Consent: Discuss risks, benefits, alternatives, realistic expectations.
- Optimization: Treat UTIs, manage comorbidities, smoking cessation, weight management.
⭐ Preoperative urodynamics are indicated for recurrent SUI or complex voiding dysfunction, especially if invasive surgery is planned.
Surgical Management of SUI - SUI: Stop That Leak!
Primary goal: Restore urethral support and continence.
- Mid-Urethral Slings (MUS): Gold standard, synthetic mesh.
- Retropubic (TVT): Passes behind pubic bone.
- Transobturator (TOT): Through obturator foramen (avoids retropubic space).
- 📌 TVT: ↑Bladder injury risk; TOT: ↑Groin pain/neuropathy risk.
- Burch Colposuspension: Abdominal/laparoscopic; sutures vagina to Cooper's ligament.
- Autologous Fascial Sling: Patient's fascia (rectus/fascia lata). For complex/recurrent SUI.
- Urethral Bulking Agents: Periurethral injection. Less invasive, ↓efficacy; for poor surgical candidates.
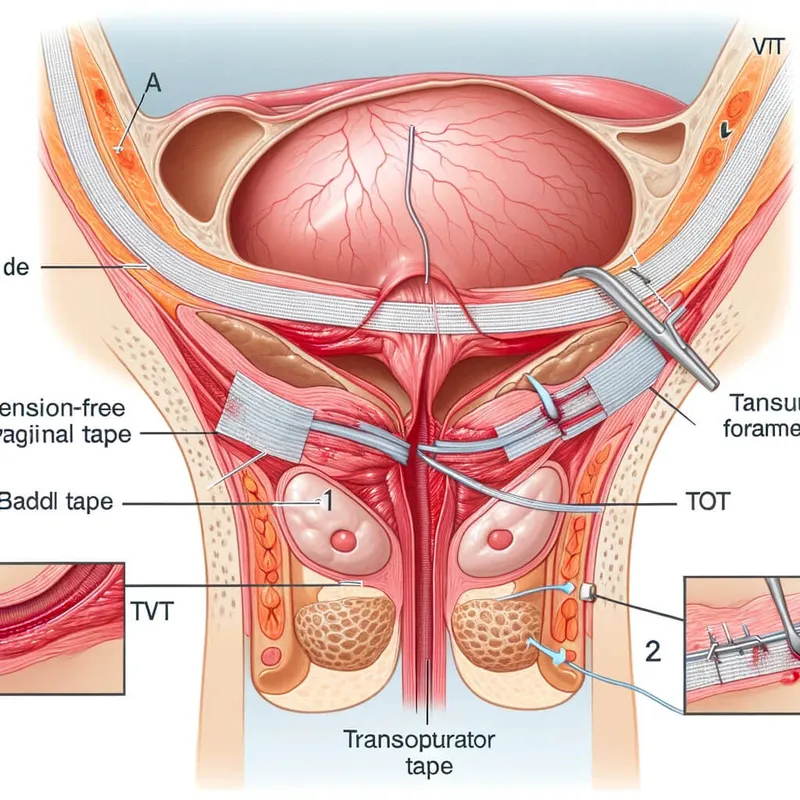
⭐ Mid-urethral slings (TVT/TOT) demonstrate long-term cure rates of approximately 80-90% for SUI.
Surgical Management of POP - POP: Hoist the Sails!
- Principles: Restore normal anatomy, alleviate symptoms, preserve/restore organ function (urinary, bowel, sexual).
- Approaches:
- Vaginal: Preferred for anterior/posterior repairs, some apical.
- Abdominal (laparoscopic/robotic/open): Often for apical prolapse (e.g., sacrocolpopexy).
- Key Procedures:
- Anterior Colporrhaphy: For cystocele.
- Posterior Colporrhaphy & Perineorrhaphy: For rectocele, perineal defects.
- Apical Suspensions:
- Vaginal: Sacrospinous Fixation (SSF), Uterosacral Ligament Suspension (USLS).
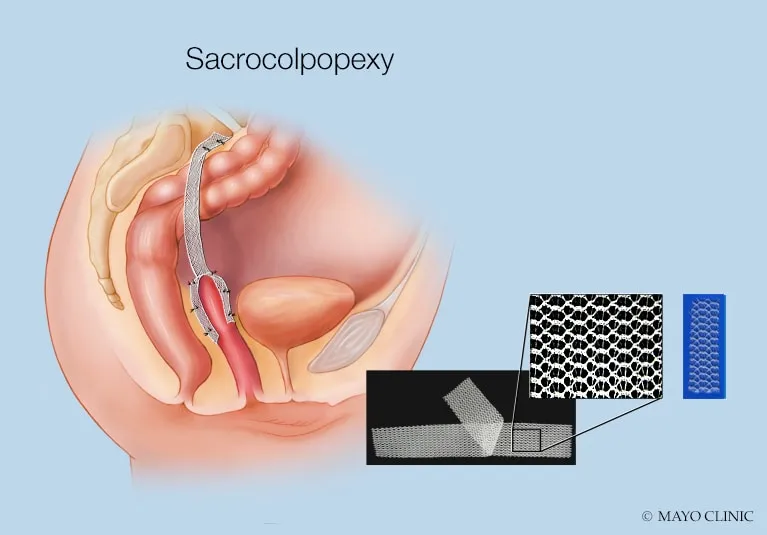
- Abdominal: Sacrocolpopexy (gold standard for vault prolapse).
- Obliterative: Colpocleisis (e.g., LeFort) for elderly/frail, not desiring sexual function.
- Mesh Use: Selective; native tissue repair often prioritized due to mesh-related complications.
⭐ > Sacrocolpopexy (abdominal) has the highest long-term success rates (often >90%) for correcting apical vaginal prolapse.
Surgical Management of Fistulas - Fistula Fix-Up Crew
- Principles: Delayed repair (3-6 months), layered closure, tension-free, good vascularity, bladder drainage.
- Vesicovaginal Fistula (VVF) Repair:
- Transvaginal (common): Latzko (partial colpocleisis for apical VVF), Flap-splitting techniques.
- Transabdominal: For complex, high, or recurrent fistulas.
- Interposition Grafts: Martius (bulbocavernosus fat pad), Gracilis muscle, Omental flap.
- Rectovaginal Fistula (RVF) Repair: Layered closure; consider sphincteroplasty if sphincter involved.
- Post-op: Indwelling catheter for 2-3 weeks, antibiotics.
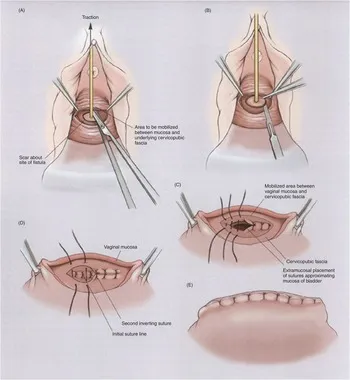
⭐ Martius graft is frequently used for complex or recurrent VVF to improve healing by providing a well-vascularized tissue layer. 📌 FISTULA Fix: Fresh edges, Interposition graft, Suture (tension-free), Tissue viability, Urinary diversion, Layered closure, Antibiotics/Antiseptics.
Postoperative Care & Complications - Post-Op Watchtower
- Key Monitoring: Pain (VAS), vitals, urine output, wound (REEDA scale).
- Prophylaxis: Antibiotics (if indicated), DVT prevention (early ambulation, SCDs/LMWH).
- Catheter Care: Aseptic technique; timely voiding trial (VT).
- Patient Education: Red flags (fever, ↑pain, discharge), activity restrictions.
- Complications:
- Early: Infection (UTI, SSI), hematoma, voiding dysfunction (VD).
- Late: Mesh erosion/exposure, chronic pain, recurrence, fistula.
⭐ Post-operative voiding dysfunction (POVD) is a key concern; failure of voiding trial (PVR > 100-150mL) needs active management.
High-Yield Points - ⚡ Biggest Takeaways
- Mid-urethral slings (TVT/TOT): gold standard for SUI, high efficacy, minimally invasive.
- Burch colposuspension: effective retropubic suspension for SUI, often with abdominal procedures.
- Sacrocolpopexy: most durable for apical prolapse (vaginal vault), abdominal or laparoscopic.
- Native tissue repairs (colporrhaphy): higher POP recurrence than mesh-augmented repairs.
- Mesh complications (erosion, pain): significant concerns in POP surgery, counsel patients.
- Colpocleisis: obliterative procedure for severe POP in frail, non-sexually active women.
- Ureteric injury: key iatrogenic risk in sacrocolpopexy and complex pelvic surgeries.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

