RDS: Intro & Assessment - Gasping for Air
Respiratory Distress (RD) in newborns: labored breathing post-birth. Prompt recognition of key signs is vital for timely intervention.
- Clinical Presentation: Observe for:
- Tachypnea: Persistent respiratory rate > 60/min.
- Expiratory grunting: Audible sound, exhalation.
- Retractions: Intercostal, subcostal, suprasternal sinking.
- Nasal flaring: Widening nostrils during inspiration.
- Cyanosis: Bluish discoloration (central: lips, tongue).
- Severity Assessment: Quantify distress.
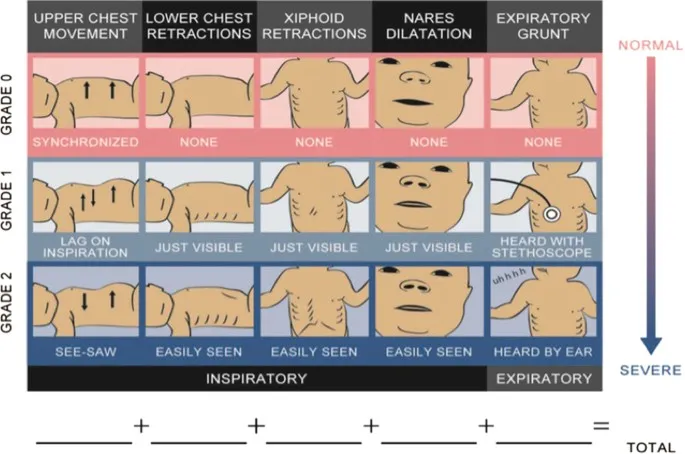
- Silverman-Andersen Score: Grades severity 0 (none) to 10 (severe). Higher score = worse.
⭐ The Silverman-Andersen score (assessing retractions, grunting, nasal flaring, etc.) is crucial for objectively grading the severity of respiratory distress in newborns.
RDS: Causes (HMD & TTN) - Surfactant Shortfall
- Hyaline Membrane Disease (HMD/RDS): Primary surfactant deficiency.
- Risks: Prematurity (< 34 wks), maternal diabetes, perinatal asphyxia.
- Patho: Immature Type II pneumocytes → ↓ surfactant (key: DPPC, SP-B) → ↑ alveolar surface tension → atelectasis, ↓ compliance.
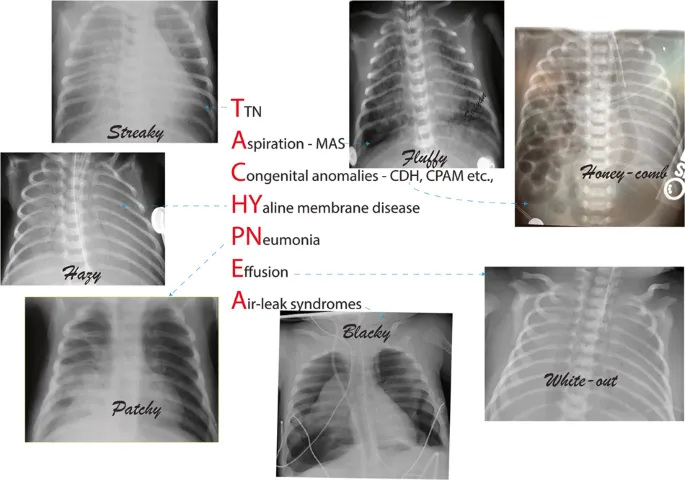
- CXR: Ground-glass pattern, air bronchograms.
- 📌 Mnemonic: Respiratory Distress in Small babies.
- Transient Tachypnea of Newborn (TTN):
- Risks: Term/late preterm, C-section, precipitous birth, maternal sedation.
- Patho: Delayed lung fluid clearance; self-resolving.
- CXR: Perihilar streaks, fissural fluid, hyperinflation. Resolves <72 hrs.
- Surfactant Insufficiency Details:
- Components: DPPC (Lecithin), SP-B (critical).
- Deficiency → HMD. L/S ratio < 2:1 = immaturity.
⭐ Antenatal administration of corticosteroids to mothers at risk of preterm delivery (typically between 24-34 weeks gestation) significantly reduces the incidence and severity of Respiratory Distress Syndrome (Hyaline Membrane Disease) in newborns.
RDS: Causes (MAS & Pneumonia) - Murky Waters & Bugs
- Meconium Aspiration Syndrome (MAS)
- Occurs in term/post-term infants.
- Pathophysiology: Meconium passage in utero (fetal distress) → aspiration → airway obstruction, chemical pneumonitis, surfactant inactivation, PPHN.
- Clinical Signs: Respiratory distress, meconium staining, barrel chest.
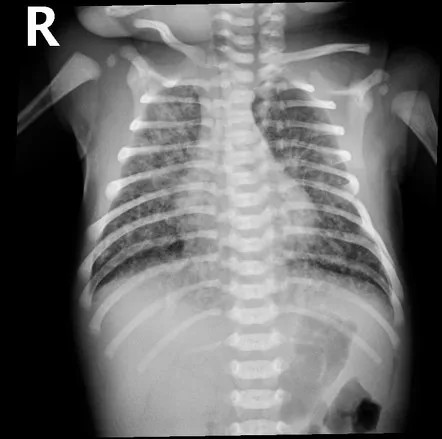
- CXR: Patchy infiltrates, hyperinflation.
- Neonatal Pneumonia
- Infection of lung parenchyma.
- Early-onset (≤ 72 hours): Group B Strep (GBS), E. coli, Listeria.
⭐ Group B Streptococcus (GBS) is the most common bacterial pathogen responsible for early-onset neonatal pneumonia and sepsis, presenting with respiratory distress.
- Late-onset (> 72 hours): Staphylococcus aureus, Pseudomonas.
- Risk factors: Prematurity, PROM > 18 hours, maternal GBS.
- Clinical Signs: Respiratory distress, apnea, temperature instability.
- CXR: Diffuse infiltrates, consolidation.
RDS: Other Causes & Mgmt - Beyond Usual Suspects
⭐ In newborns with Congenital Diaphragmatic Hernia (CDH), immediate endotracheal intubation and orogastric tube placement for gastric decompression are critical; bag-mask ventilation is contraindicated as it can worsen respiratory compromise by insufflating the herniated bowel.
- Key Differential Diagnoses:
- Pneumothorax: Sudden deterioration; transillumination +ve; needle aspiration.
- Meconium Aspiration Syndrome (MAS): Patchy infiltrates on CXR; may need surfactant.
- Transient Tachypnea of Newborn (TTN): Self-resolving (<72 hrs); supportive care.
- Persistent Pulmonary Hypertension (PPHN): Severe hypoxemia unresponsive to O2; ECHO diagnostic; iNO therapy.
- General Management Principles:
- Maintain ABCs (Airway, Breathing, Circulation).
- Supportive: Thermoregulation, IV fluids, glucose.
- Targeted therapy for specific cause.
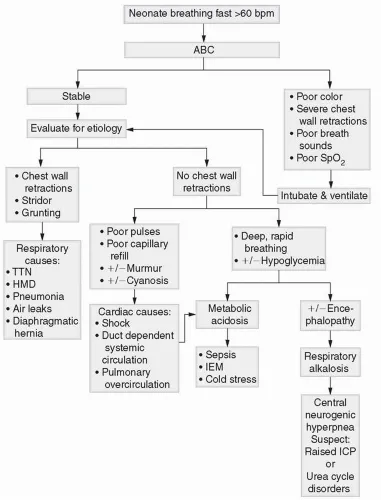
- Respiratory support escalation (see flowchart).
High-Yield Points - ⚡ Biggest Takeaways
- RDS (HMD): In preterms due to surfactant deficiency. CXR: ground-glass opacities, air bronchograms.
- TTN: In term/late preterm (post-C-section) from delayed lung fluid clearance. CXR: perihilar streaking. Resolves 24-72h.
- MAS: In post-term/stressed infants due to meconium aspiration. CXR: patchy infiltrates, hyperinflation.
- PPHN: Elevated pulmonary vascular resistance (R-L shunt). Echocardiography is diagnostic.
- Congenital Pneumonia: Early onset, often GBS. CXR variable.
- Apnea of Prematurity: Common <34 weeks. Breathing cessation >20s or with bradycardia/desaturation_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

