Defining One Health - All for One Health!
- Definition: A collaborative, multisectoral, and transdisciplinary approach - working at local, regional, national, and global levels.
- Core Idea: Recognizes that the health of people is closely connected to the health of animals and our shared environment.
- Goal: To achieve optimal health outcomes for people, animals, and ecosystems.
- Key Areas Addressed:
- Zoonotic diseases (e.g., Rabies, Influenza, Nipah)
- Antimicrobial Resistance (AMR)
- Food safety and security
- Vector-borne diseases
- Environmental contamination

⭐ The Tripartite alliance (WHO, FAO, WOAH - World Organisation for Animal Health), now expanded to the Quadripartite with UNEP (United Nations Environment Programme), spearheads global One Health initiatives.
The One Health Triad - People, Pets, Planet
- Core Principle: Interconnectedness of health between humans, animals (domestic/wild), and their shared environment.
- Components & Interactions:
- Human Health ("People"): Affected by zoonoses, food safety, and environmental contaminants.
- Animal Health ("Pets"/Livestock): Animals act as disease reservoirs, sentinels of environmental toxins, and contribute to food security.
- Environmental Health ("Planet"): Factors like climate change, deforestation, and pollution impact pathogen emergence and vector distribution.
- Significance: Diseases often emerge at the interface of these three components, necessitating a collaborative approach.

⭐ Approximately 75% of recent emerging infectious diseases affecting humans are of animal origin (zoonotic).
EID Catalysts - One Health Under Siege
-
Core Drivers Fueling EIDs:
- Microbial Adaptation: Genetic changes (e.g., antigenic drift/shift in Influenza).
- Human Factors: ↑Population density & mobility, risky behaviors, altered host susceptibility (e.g., immunosuppression).
- Environmental Changes: Deforestation, climate change (vector shifts), urbanization, habitat loss (↑human-wildlife interface).
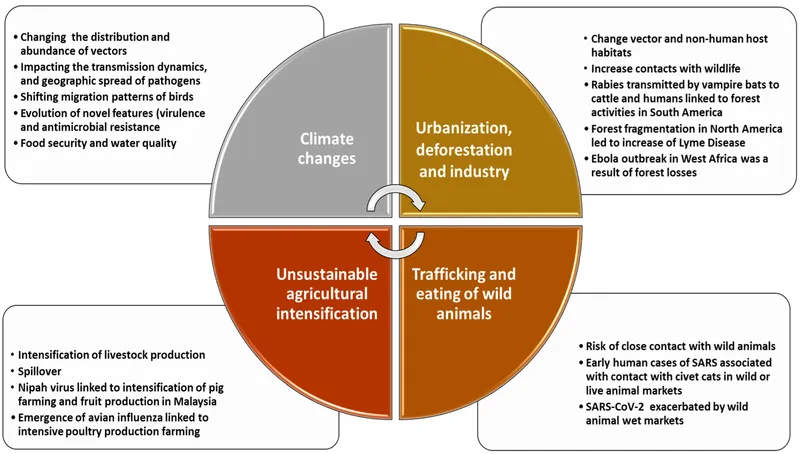
- Public Health & Governance: Weak surveillance, poor sanitation/hygiene, ↓healthcare access, conflict.
- Agricultural Practices: Intensive farming, live animal markets, wildlife trade, antimicrobial overuse.
-
Zoonotic Spillover: A Simplified Pathway
- Challenges Impeding One Health:
- Siloed Systems: Poor coordination between human, animal, & environmental health sectors.
- Resource Gaps: Insufficient funding, workforce, & infrastructure for integrated surveillance & response.
- Policy & Political Will: Lack of robust policies, enforcement, & sustained commitment.
- Antimicrobial Resistance (AMR): A pervasive threat complicating EID management. ⭐ > Approximately 75% of recently emerging infectious diseases in humans are of animal origin.
One Health in Practice - India's United Front
- Apex Body & Frameworks:
- National Standing Committee on Zoonoses (NSCZ): Guides policy, inter-sectoral coordination.
- Integrated Disease Surveillance Programme (IDSP): Links human & animal health surveillance.
- National Action Plan on Antimicrobial Resistance (NAP-AMR).
- Key Programmes & Initiatives:
- National Rabies Control Programme (NRCP).
- Programme for Control of Brucellosis.
- Emerging
High‑Yield Points - ⚡ Biggest Takeaways
- One Health: A unified, collaborative approach linking human, animal, and environmental health.
- Core Principle: Recognizes the interdependence of these domains for optimal health outcomes.
- Key threats addressed: Zoonotic diseases (e.g., Rabies, Nipah, KFD), Antimicrobial Resistance (AMR), and food safety.
- Involves multisectoral collaboration: physicians, veterinarians, environmental scientists, and policymakers.
- Crucial for early disease detection, outbreak prevention/response, and AMR containment strategies.
- India's National Action Plan on AMR and zoonoses control programs utilize this approach_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

