Indications & Goals - Why We Ventilate
Indications (Why):
- Acute Respiratory Failure (ARF)
- Hypoxemic: PaO2 < 60 mmHg despite FiO2 > 0.6 (e.g., ARDS, pneumonia, pulmonary edema)
- Hypercapnic: PaCO2 > 50 mmHg with pH < 7.30 (e.g., COPD exacerbation, neuromuscular disease)
- Airway Protection
- ↓ Glasgow Coma Scale (GCS) ≤ 8
- Risk of aspiration (e.g., bulbar palsy)
- Apnea or Inadequate Respiratory Effort
- Control of Ventilation (e.g., head injury to manage ICP)
- Prophylactic (e.g., major surgery, trauma)
Goals (What we aim for):
- Improve Gas Exchange
- Correct hypoxemia (↑PaO2)
- Correct respiratory acidosis (↓PaCO2, ↑pH)
- Reduce Work of Breathing (WOB)
- Reverse Respiratory Muscle Fatigue
- Permit Sedation/Neuromuscular Blockade
- Stabilize Chest Wall
⭐ Acute respiratory acidosis (pH < 7.25, PaCO2 > 50 mmHg) despite non-invasive measures is a strong indication for intubation and mechanical ventilation.
Key Terms & Physiology - Talking the Talk
- Tidal Volume ($V_t$): Air per breath (target 6-8 mL/kg IBW).
- PEEP (Positive End-Expiratory Pressure): Pressure at end-exhalation; prevents alveolar collapse.
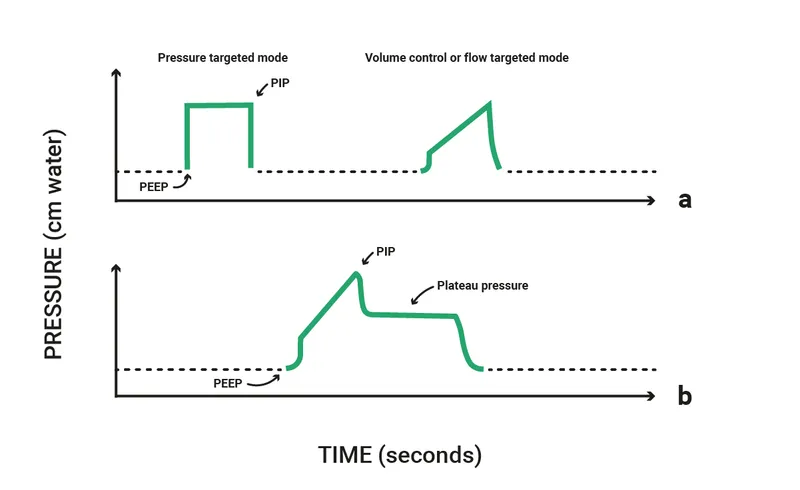
- PIP (Peak Inspiratory Pressure): Max pressure during inspiration; reflects airway resistance + elastic recoil.
- $P_{plat}$ (Plateau Pressure): Inspiratory hold pressure (no flow); reflects alveolar pressure. Aim < 30 cmH₂O.
- Compliance ($C$): Lung/chest wall distensibility; $C = \Delta V / \Delta P$.
- Static Compliance is given by the formula: $C_{stat} = V_t / (P_{plat} - PEEP)$.
⭐ Static Compliance reflects the elastic properties of the lung and chest wall. It is characteristically decreased in conditions like ARDS and pneumonia.
- Resistance ($R$): Airway opposition to gas flow; $R = (PIP - P_{plat}) / \text{flow}$. ↑ in asthma, COPD.
- Minute Ventilation ($V_E$): Total air exhaled per minute ($V_t \times \text{RR}$).
- I:E Ratio: Ratio of inspiratory time to expiratory time (e.g., 1:2).
- FiO₂: Fraction of Inspired Oxygen delivered to the patient.
Modes & Settings - Choosing Wisely
- Common Modes:
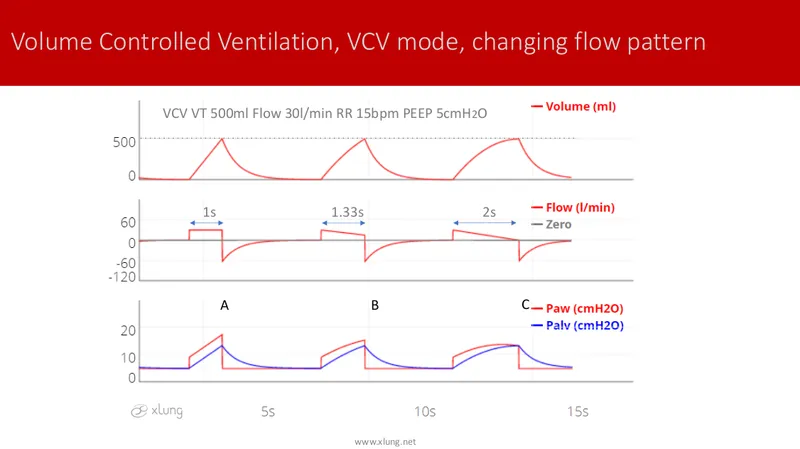
- Volume Control (VC/ACVC): Set $V_t$; pressure varies. Risk: Volutrauma.
⭐ In Assist-Control Volume Cycled (ACVC) mode, every breath (patient-triggered or time-triggered) delivers the preset tidal volume, risking volutrauma if not monitored.
- Pressure Control (PCV): Set PIP; $V_t$ varies. Risk: Hypoventilation (if compliance ↓ / resistance ↑).
- Pressure Support (PSV): Patient-triggered, pressure-limited, flow-cycled. Aids weaning.
- SIMV: Mandatory breaths (VC/PC) + spontaneous breaths (PSV).
- Volume Control (VC/ACVC): Set $V_t$; pressure varies. Risk: Volutrauma.
- Initial Settings (Adult):
- $V_t$: 6-8 mL/kg IBW (ARDS: 4-6 mL/kg).
- RR: 12-16/min (adj. for $PaCO_2$, pH).
- PEEP: Start 5 cm H₂O (titrate for $O_2$, lung protection).
- $FiO_2$: Start 1.0, titrate to $SpO_2$ >92% ($PaO_2$ 60-80 mmHg).
- I:E Ratio: 1:2-1:3 (obstructive: prolong E-time, e.g., 1:4).
Complications & Weaning - The Escape Plan
- Complications:
- VAP: Prevent (HOB 30-45°, oral care, cuff 20-30 cmH₂O).
- Barotrauma/Volutrauma (e.g., pneumothorax).
- O₂ Toxicity: FiO₂ > 0.6 for > 24-48h.
- Cardio: ↓CO (high PEEP).
- VIDD (Ventilator-Induced Diaphragmatic Dysfunction).
- Weaning:
- Readiness: Cause improving, stable, PaO₂/FiO₂ > 150-200, PEEP ≤ 5-8, FiO₂ ≤ 0.4-0.5.
- SBT: 30-120 min (T-piece, PSV 5-7 cmH₂O, CPAP 5 cmH₂O).
⭐ A Rapid Shallow Breathing Index (RSBI = RR/Vt in Liters) < 105 breaths/min/L is a good predictor of successful weaning.
- Key Parameters (📌):
- RSBI: $RR/V_T$ < 105.
- MIP/NIF: < -20 cmH₂O.
- RR < 35/min, $V_T$ > 5 mL/kg.
- SBT Failure: RR > 35, SpO₂ < 90%, HR > 140, distress. Extubate if SBT success + airway protected.
High‑Yield Points - ⚡ Biggest Takeaways
- ARDS: Use low tidal volume (6 mL/kg IBW) to prevent VILI.
- PEEP: Improves oxygenation, recruits alveoli, prevents atelectasis.
- PCV: Decelerating flow aids lung protection in non-compliant lungs.
- VCV: Guarantees minute volume; risk of barotrauma with changing compliance.
- Weaning: RSBI < 105 is a key predictor for extubation success.
- Complications: Monitor for VAP, barotrauma, volutrauma, oxygen toxicity.
- Oxygenation: Target SpO2 88-95% (PaO2 55-80 mmHg) with lowest FiO2.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

