PH Basics - Pressure Cooker Lungs
- Defined by mean pulmonary arterial pressure ($mPAP$).
⭐ The 2022 ESC/ERS guidelines redefine pulmonary hypertension as $mPAP$ > 20 mmHg at rest.
- Normal $mPAP$: $14 \pm 3$ mmHg.
- Pathophysiology: ↑ Pulmonary Vascular Resistance (PVR) leads to Right Ventricular (RV) pressure overload ("pressure cooker" effect), causing potential RV failure.
- WHO Clinical Classification (5 Groups):
- Group 1: PAH (Pulmonary Arterial Hypertension)
- Group 2: PH due to Left Heart Disease
- Group 3: PH due to Lung Diseases/Hypoxia
- Group 4: CTEPH (Chronic Thromboembolic PH)
- Group 5: PH with unclear/multifactorial mechanisms
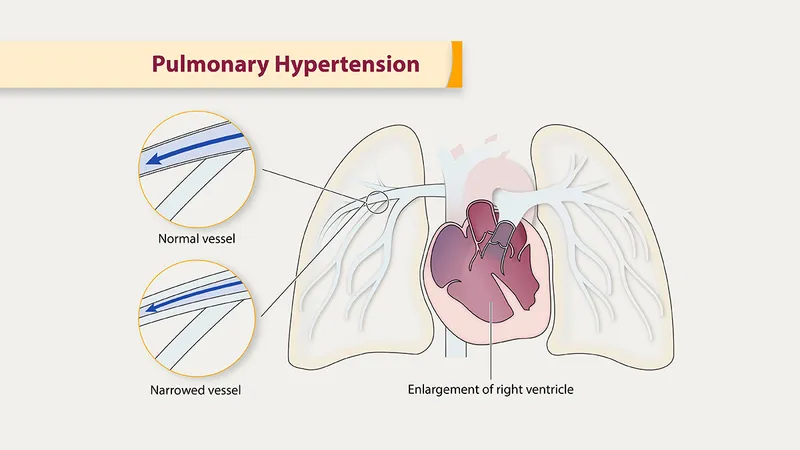
Vessel Chaos - Why Lungs Squeeze
- Primary Insults:
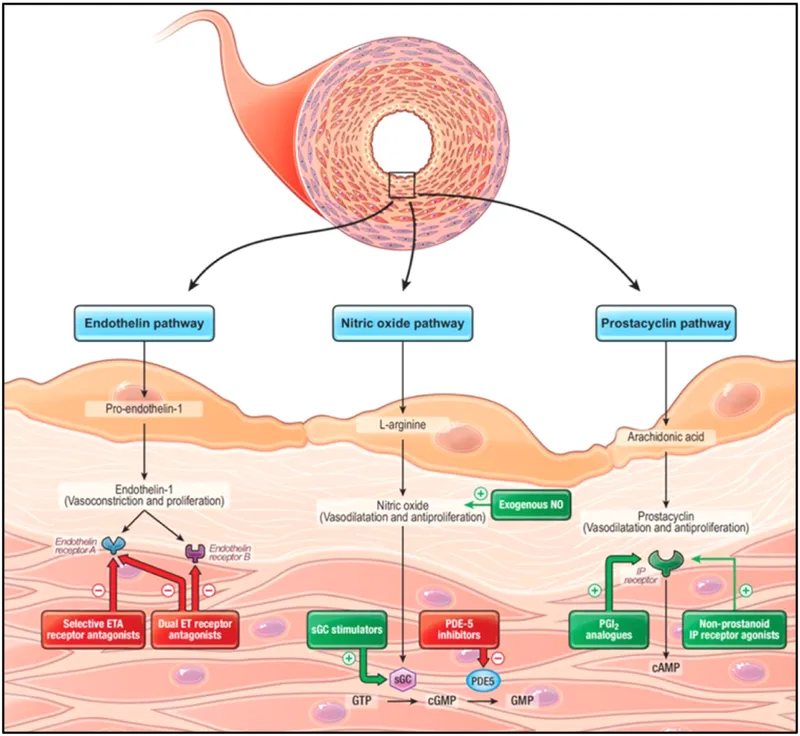
- Endothelial dysfunction: ↓NO, ↓Prostacyclin; ↑Endothelin-1.
- Vascular Smooth Muscle (VSM) proliferation & hypertrophy.
- Inflammation & immune dysregulation.
- Abnormal coagulation (in-situ thrombosis).
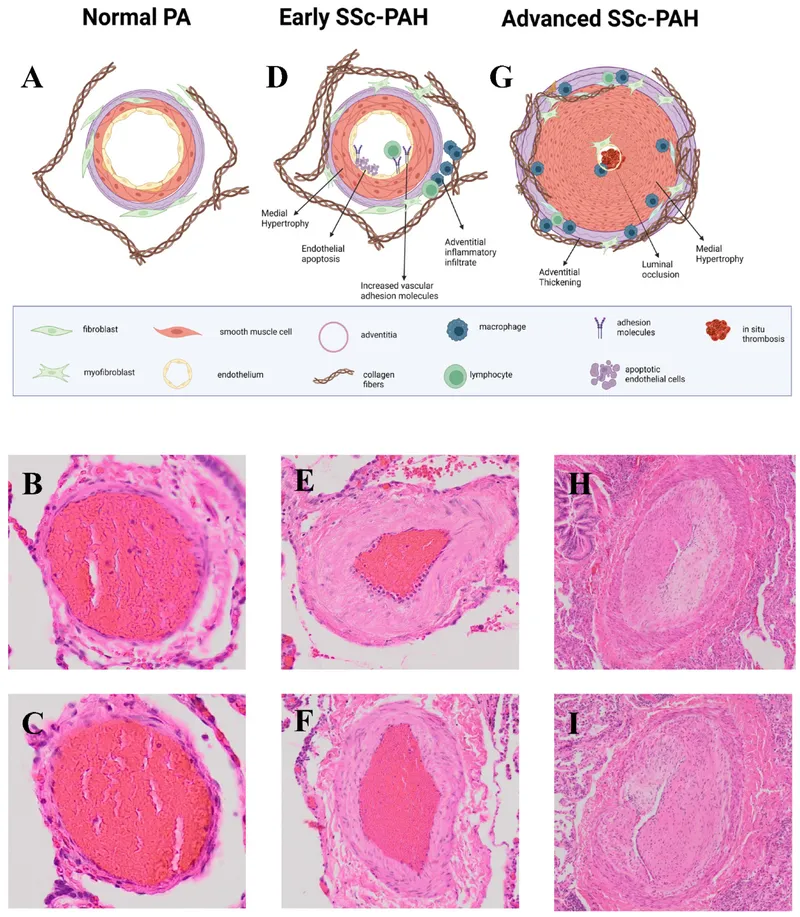
- Structural Changes (Remodeling):
- Medial hypertrophy, intimal proliferation, adventitial thickening.
- Plexiform lesions (pathognomonic for severe PAH).
- Genetic Predisposition:
- BMPR2 gene mutations (esp. in Heritable PAH).
- Hemodynamic Consequence: ↑PVR → ↑PAP → RV overload → RV failure.
⭐ Key pathogenic pathways include endothelial dysfunction (↓NO, ↓prostacyclin, ↑endothelin-1), vascular smooth muscle proliferation, and in-situ thrombosis. BMPR2 mutations are common in heritable PAH.
 oka
oka
Spotting PH - Breathless Clues
- Symptoms:
- Progressive exertional dyspnea (key)
- Fatigue, weakness
- Angina-like pain, exertional syncope
- Peripheral edema, ascites (RHF signs)
- Signs:
- Loud, palpable P2
- RV heave (parasternal lift)
- ↑ JVP (prominent 'a'/'cv' waves)
- Murmurs: TR (LLSB, ↑ insp.), Graham Steell (PR, LUSB, ↑ insp.)
- Initial Workup:
-
ECG: RVH (RAD, RBBB, P pulmonale), RV strain
-
CXR: Enlarged central PAs, RV prominence, clear lungs
-
Echocardiography (TTE):
- Estimates RVSP (TR jet > 2.8 m/s suggests PH)
- Formula: RVSP $\approx 4 \times (TRV_{max})^2$ + RAP
- Assesses RV size/function (TAPSE < 17mm, S' < 9.5 cm/s), PA dilation
-
6MWD: Functional status (< 300m poor prognosis)
-
⭐ RHC: gold standard. Confirms mPAP > 20 mmHg. Pre-capillary PH: PAWP ≤ 15 mmHg & PVR > 2 Wood Units.
Easing Pressure - Treatment Tactics
- General: Diuretics (RHF), O2 (PaO2 < 60 mmHg), anticoagulation (PAH, CTEPH), exercise, vaccines.
- PAH (WHO Group 1):
- RHC + Acute Vasoreactivity Test (AVT).
⭐ Acute vasoreactivity testing during RHC is crucial for WHO Group 1 PAH; positive responders (mPAP drop ≥10 mmHg to reach mPAP ≤40 mmHg, with ↑/unchanged CO) may benefit from CCBs.
- AVT (+): High-dose CCBs (Nifedipine, Diltiazem).
- AVT (-) / CCB failure: Risk-stratified targeted therapies.
- 📌 ERAs (BAM!): Bosentan, Ambrisentan, Macitentan.
- 📌 PDE-5i (Fill!): Sildenafil, Tadalafil.
- 📌 Prostacyclin pathway (EITS!): Epoprostenol, Iloprost, Treprostinil, Selexipag.
- sGC stimulator: Riociguat.
- Initial/sequential combination therapy common. Lung transplant if refractory.
- RHC + Acute Vasoreactivity Test (AVT).
- Other PH Groups: Treat underlying cause.
- Group 2: LHD management.
- Group 3: Lung disease Rx, O2.
- Group 4 (CTEPH): Anticoagulation; PEA/BPA; Riociguat.
- Group 5: Address specific etiology.
High‑Yield Points - ⚡ Biggest Takeaways
- Pulmonary Hypertension (PH): Defined by mPAP >20 mmHg at rest, confirmed by RHC.
- Group 1 (PAH) treatment involves targeted therapies: prostanoids, ERAs, PDE5 inhibitors.
- Most common overall PH cause: Left heart disease (WHO Group 2).
- Group 3 PH: Caused by lung diseases or chronic hypoxia (e.g., COPD, ILD).
- Gold Standard Diagnosis: Right Heart Catheterization (RHC) for definitive assessment.
- Key ECG findings: Right Ventricular Hypertrophy (RVH), P pulmonale, right axis deviation.
- Auscultation: A loud P2 heart sound is a characteristic clinical sign.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

