CAD & Angina Basics - Heart's Cry for Help
- Coronary Artery Disease (CAD): Atherosclerosis of epicardial coronary arteries leading to reduced myocardial perfusion.
- Angina Pectoris: Symptomatic, transient myocardial ischemia; typically chest discomfort/pressure due to O₂ supply < demand.
- Supply ↓: Atherosclerosis (most common, >70% stenosis often symptomatic), coronary spasm, arteritis.
- Demand ↑: Exercise, emotional stress, HTN, aortic stenosis.
- Pathophysiology: Endothelial dysfunction → lipid accumulation → atheromatous plaque formation → progressive luminal narrowing.
- Major Risk Factors:
- Non-Modifiable: Age (Male >45y, Female >55y), Male sex, Family Hx (1st degree relative with premature CAD: M <55y, F <65y).
- Modifiable: Smoking, Hypertension, Diabetes Mellitus, Dyslipidemia (↑LDL, ↓HDL, ↑Triglycerides), Obesity, Sedentary lifestyle.
📌 Mnemonic (Modifiable): "SHODDS" - Smoking, Hypertension, Obesity, Diabetes, Dyslipidemia, Sedentary.

⭐ Stable angina typically manifests when a coronary artery is narrowed by >70% of its luminal diameter (critical stenosis).
Angina Varieties - Chest Pain Flavors
- Stable Angina (Effort Angina)
- Predictable, exertional pain; relieved by rest/NTG (<5 min).
- Fixed coronary stenosis (>70%).
- Unstable Angina (UA)
- New onset, crescendo, or rest angina (>20 min).
- High-risk ACS; plaque rupture/thrombosis.
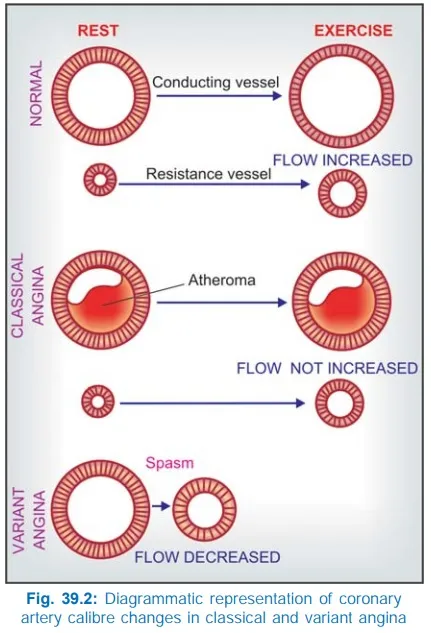
- Prinzmetal (Variant) Angina
- Coronary artery spasm; often at rest, nocturnal.
- Transient ST ↑ on ECG during pain.
- Rx: CCBs, nitrates. ⚠️ Avoid non-selective β-blockers.
- Microvascular Angina (Syndrome X)
- Angina with normal epicardial coronaries; microvascular dysfunction.
- Silent Ischemia
- Asymptomatic ischemia; detected by ECG/stress test.
- Common in diabetics, elderly.
⭐ Prinzmetal angina uniquely shows transient ST-segment elevation during chest pain episodes, unlike other anginas.
Diagnostic Toolkit - Peeking at Pipes
- Electrocardiogram (ECG):
- Resting: ST↓, T-inversion, Q-waves (old MI). Often normal in stable angina (~50%).
- Stress ECG (TMT): Provokes ischemia; monitors for ST changes.
- Cardiac Biomarkers (for ACS):
- Troponin I/T: ↑ 3-6 hrs, peak 12-24 hrs. Highly sensitive/specific.
- CK-MB: ↑ 4-6 hrs, normalizes 48-72 hrs (reinfarction).
- Non-Invasive Imaging:
- Stress Echocardiography/MPI: Detect ischemia (wall motion/perfusion defects).
- CCTA (Coronary CT Angiography): Anatomical assessment. High Negative Predictive Value.
- Invasive Coronary Angiography (CAG):
- Gold standard. Defines anatomy, guides revascularization (PCI/CABG).
- Fractional Flow Reserve (FFR) < 0.80 or iFR < 0.89 indicates significant stenosis.
⭐ CAG is indicated in patients with high pre-test probability, positive stress tests with high-risk features, or inconclusive non-invasive tests.
Treatment Strategies - Calming the Storm
Goals: Relieve angina, prevent MI & death.
- Medical Therapy (ABCDE Approach):
- Antiplatelets: Aspirin (75-150mg), Clopidogrel. DAPT crucial post-PCI.
- Beta-blockers: 1st line stable angina (e.g., Metoprolol).
- Cholesterol-lowering (Statins): High-intensity (Atorvastatin 40-80mg). Target LDL < 55 mg/dL (very high risk).
- Drugs for symptoms & Diet:
- Nitrates (GTN SL 0.3-0.6mg PRN, ISMN/ISDN): Vasodilators (SE: headache, tolerance).
- CCBs (Amlodipine; Verapamil/Diltiazem for rate control if β-blockers C/I).
- Others: Ranolazine, Nicorandil, Ivabradine (for HR control if β-blockers not tolerated/sufficient).
- ECE Inhibitors/ARBs: If HTN, DM, LV dysfunction, or post-MI.
- Revascularization:
- PCI (stenting) or CABG for severe/refractory disease or high-risk anatomy.
- 📌 Acute Management (ACS): MONA-BASH (Morphine, $O_2$, Nitrates, Aspirin, β-blocker, ACEi, Statin, Heparin).
⭐ Beta-blockers are C/I in Prinzmetal angina (risk of unopposed α-spasm); CCBs/nitrates are mainstay.
High‑Yield Points - ⚡ Biggest Takeaways
- Stable angina: Exertional chest pain, relieved by rest/nitrates; ECG: ST depression.
- Prinzmetal angina: Coronary spasm, ST elevation at rest; Rx: CCBs, nitrates; β-blockers contraindicated.
- Unstable angina: Rest angina or crescendo pattern; high MI risk, urgent management.
- Atherosclerosis: Most common cause of CAD.
- Coronary angiography: Gold standard diagnosis for CAD.
- Acute angina: Sublingual nitroglycerin is key.
- CAD medical therapy: Aspirin, statins, β-blockers (avoid in Prinzmetal).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

