OSA: Definition & Pathophysiology - Snore Wars Begins
- Definition: Recurrent upper airway obstruction during sleep.
- Apnea: Airflow cessation ≥10s.
- Hypopnea: Airflow ↓ ≥30% for ≥10s + ≥3% O₂ desat / arousal.
- RERA: Respiratory Effort-Related Arousal.
- AHI (Apnea-Hypopnea Index) Severity:
- Mild: 5-14.9/hr
- Moderate: 15-29.9/hr
- Severe: ≥30/hr
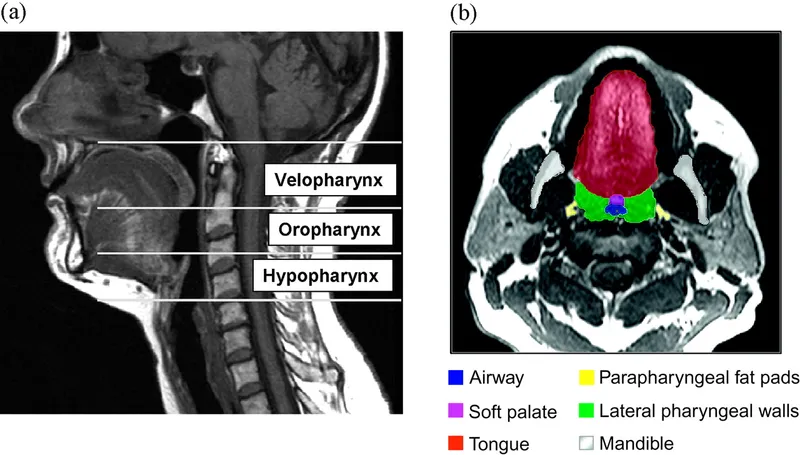
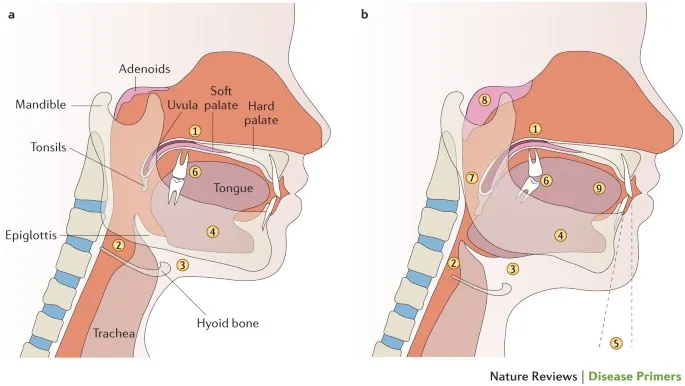
- Pathophysiology: Upper airway collapse (anatomical: retrognathia, tonsillar hypertrophy; non-anatomical: impaired muscle function) → intermittent hypoxia, hypercapnia, sleep fragmentation, ↑sympathetic activity.
- Sites: Palate, tongue base, lateral pharyngeal walls.
- Epidemiology: M>F, ↑age, obesity.
⭐ AHI is calculated as (total apneas + total hypopneas) / total sleep time in hours.
OSA: Risk Factors & Etiology - The Choke Artists
Key predisposing factors narrow the airway:
- Obesity: Most critical. BMI >30 kg/m², central adiposity, ↑ neck circumference (>43cm M, >40cm F).
- Anatomic: Male gender, Age >40-65 yrs, craniofacial abnormalities (retrognathia, micrognathia, adenotonsillar hypertrophy - esp. children), family history.
- Lifestyle/Other: Smoking, alcohol/sedatives (pre-sleep), supine sleep position, nasal obstruction.
- Associated Conditions: Hypothyroidism, Acromegaly, PCOS.
⭐ Obesity is the single most significant modifiable risk factor for OSA.
OSA: Clinical Features & Complications - Night & Day Woes
- Nocturnal Symptoms:
- Loud habitual snoring, witnessed apneas/gasps.
- Choking/gasping awakenings, restless sleep, nocturia.
- Daytime Symptoms:
- Excessive Daytime Sleepiness (EDS) - Epworth Scale >10.
- Morning headaches, fatigue, impaired concentration/memory.
- Mood disturbances (irritability, depression).
- Key Complications (Systemic Impact):
- Cardiovascular: Hypertension (systemic & pulmonary), CAD, MI, Arrhythmias (AF), Stroke, CHF.
- Metabolic: Insulin resistance, Type 2 DM, Metabolic syndrome.
- Neurocognitive: Impaired vigilance, ↑MVA risk.
- Others: GERD, NAFLD.
⭐ Untreated OSA significantly increases the risk of cardiovascular morbidity and mortality.
OSA: Diagnosis - The Sleep Sleuth
- Screening Tools:
- Epworth Sleepiness Scale (ESS)
- STOP-BANG (Snoring, Tired, Observed apnea, Pressure, BMI, Age, Neck, Gender)
- Berlin Questionnaire
- Diagnostic Tests:
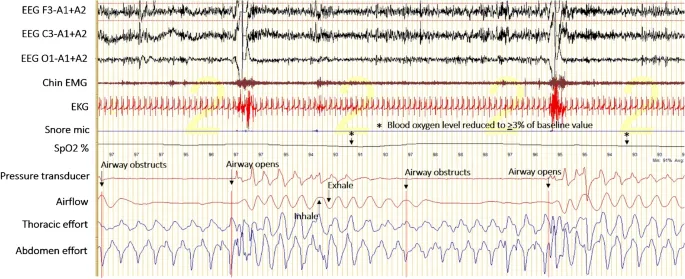
- Polysomnography (PSG): Gold standard. In-lab, attended. Monitors EEG, EOG, EMG, ECG, airflow, effort, SaO2.
- Home Sleep Apnea Testing (HSAT): For high pre-test probability, uncomplicated cases.
- Key Criteria: Apnea-Hypopnea Index (AHI) / Respiratory Disturbance Index (RDI)
- Mild: AHI 5-14.9/hr
- Moderate: AHI 15-29.9/hr
- Severe: AHI ≥30/hr
- Other: ENT exam, Cephalometry, Drug-Induced Sleep Endoscopy (DISE) for surgical planning.
⭐ STOP-BANG score: ≥3 indicates high risk of OSA; ≥5 is very high risk.
OSA: Management - Breathing Easy Again
- General/Behavioral: Weight loss (target 10%), positional therapy (avoid supine), exercise, avoid alcohol/sedatives pre-bedtime, smoking cessation, manage nasal obstruction.
- PAP Therapy:
- CPAP: First-line for moderate-severe OSA.
- APAP/BiPAP: For CPAP intolerance or comorbid hypoventilation.
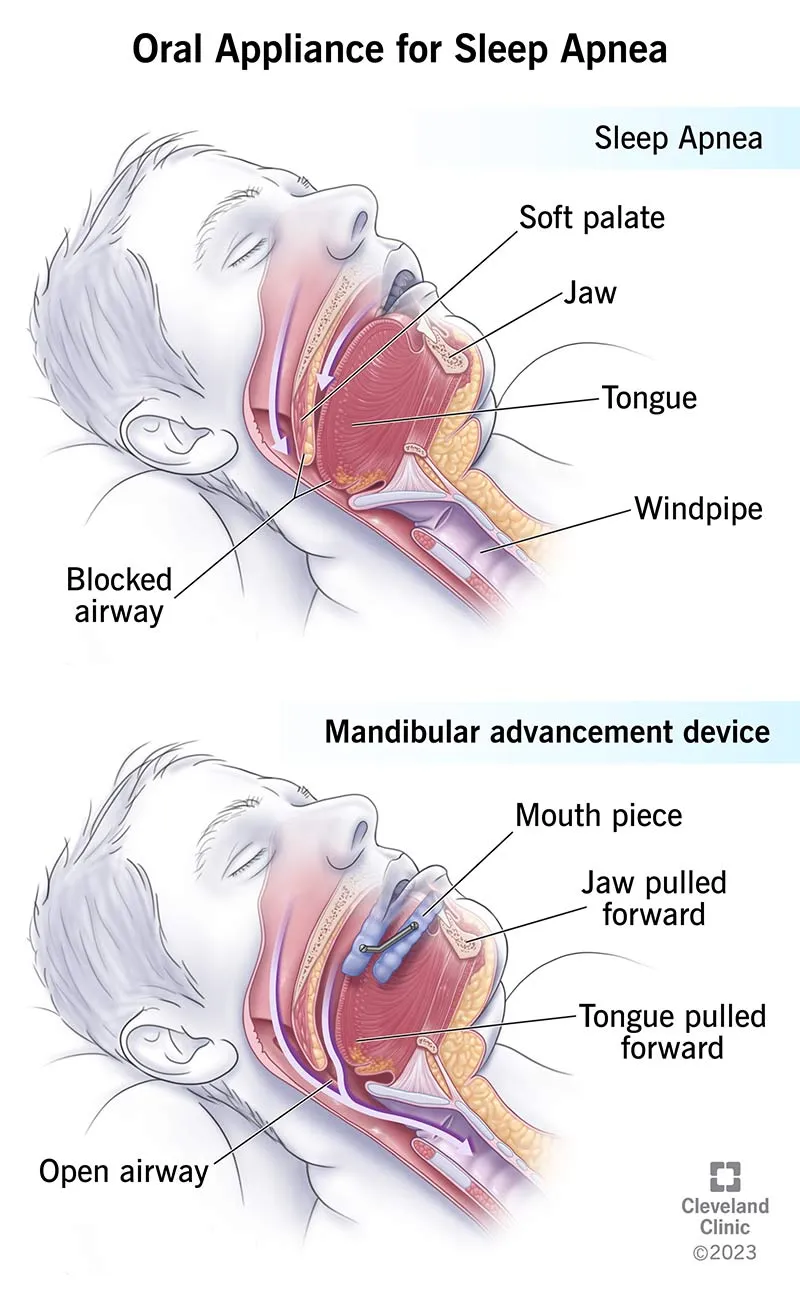
- Oral Appliances (OAs): For mild-moderate OSA or CPAP intolerance. (e.g., MADs).
- Surgery (Site-specific, selected patients): UPPP, MMA, HGNS. Tracheostomy for refractory severe OSA.
⭐ CPAP adherence is critical: ≥4 hours/night on ≥70% of nights for effectiveness.
High-Yield Points - ⚡ Biggest Takeaways
- OSA involves recurrent upper airway obstruction during sleep, causing hypoxia and sleep fragmentation.
- Obesity is the strongest risk factor; others include male gender, ↑age, and large neck circumference.
- Excessive daytime sleepiness (EDS) is a hallmark symptom; use Epworth Sleepiness Scale for subjective assessment.
- Polysomnography (PSG) is the gold standard for diagnosis, with AHI ≥5 events/hour being diagnostic.
- Continuous Positive Airway Pressure (CPAP) is the first-line treatment; weight loss is crucial.
- Major complications include systemic hypertension, cardiac arrhythmias, stroke, and pulmonary hypertension.
- The STOP-BANG questionnaire is a common screening tool for OSA risk assessment.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

