Ultrasound-Guided Neuraxial Anesthesia - Echoes & Spines
- Why USG? ↑ success rates, ↓ needle passes & complications. Essential for challenging anatomy (obesity, scoliosis, previous surgery).
- Indications: Predicted difficult access, coagulopathy (visualize epidural space depth), teaching tool.
- Probe Selection:
- Low-frequency (2-5 MHz) curvilinear: Adults, deeper penetration.
- High-frequency (10-13 MHz) linear: Pediatrics, superficial structures.
- Views & Structures:
- Transverse: Interspinous view (target window), articular processes.
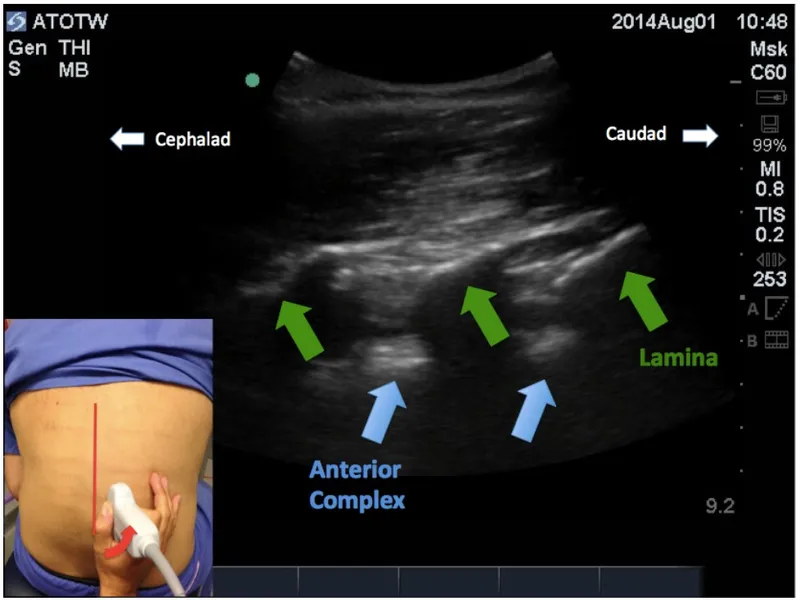
- Paramedian Sagittal: Interlaminar view ("sawtooth" laminae).
- Identify: Ligamentum flavum, posterior dura, epidural space, thecal sac.

⭐ The "paramedian sagittal oblique" (PSO) view is often optimal for visualizing the interlaminar space and guiding real-time needle insertion for neuraxial blocks in adults.
Ultrasound-Guided Neuraxial Anesthesia - Picture Perfect Punctures
- Goal: Precise needle placement, ↑ success, ↓ attempts, ↓ complications.
- Probe: Curvilinear (low frequency, deeper) or linear (high frequency, superficial).
- Views:
- Transverse Process View: Identifies spinous process & transverse processes.
- Sagittal Paramedian View: "Sawtooth" appearance of laminae; identifies interlaminar spaces.
- Key Structures (Hyperechoic → Hypoechoic):
- Bone (spinous process, laminae): Hyperechoic with posterior acoustic shadow.
- Ligamentum Flavum: Hyperechoic band.
- Dura Mater: Hyperechoic line (anterior to ligamentum flavum).
- Epidural Space: Hypoechoic, between ligamentum flavum & dura.
- Intrathecal Space (CSF): Anechoic.
- Posterior Longitudinal Ligament & Vertebral Body: Deeper hyperechoic lines.
- Techniques:
- Pre-procedural scanning: Mark skin entry point & trajectory.
- Real-time guidance: Needle visualized during insertion.
- Advantages: Identifies midline, depth to epidural/intrathecal space, intervertebral level, detects anatomical variations (e.g., scoliosis).
⭐ "Shamrock Sign" (Transverse view): Spinous process (stem) & two transverse processes (leaves) help identify the paramedian window for thoracic epidurals.
- Considerations: Thoracic spine challenging due to acute angulation of spinous processes; paramedian approach often preferred.
- 📌 Mnemonic: "TITS & LITS" - Transverse Interspinous Transverse Sagittal (views) & Ligamentum flavum Intrathecal Target Space (layers).
Ultrasound-Guided Neuraxial Anesthesia - Guided Needle Navigation
-
Pre-procedural Scanning:
- Identify midline (spinous processes).
- Determine optimal interspace (widest, easiest access).
- Measure depth to epidural/intrathecal space (ligamentum flavum, posterior dura).
- Plan needle trajectory: angle, entry point.
- Assess for scoliosis, previous surgery, or anatomical variations.
-
Real-Time Needle Guidance:
- In-Plane (Longitudinal):
- Needle shaft & tip visualized in the plane of ultrasound beam.
- Preferred for continuous visualization.
- Transducer aligned with needle path.
- Out-of-Plane (Transverse):
- Needle visualized as a hyperechoic dot (cross-section).
- Tip localization can be challenging; requires fanning transducer.
- Useful for initial angulation.
- In-Plane (Longitudinal):
-
Needle Visualization:
- Often challenging due to steep insertion angles.
- Techniques to improve: hydro-dissection, stylet movement, echogenic needles.
⭐ High-Yield: The paramedian sagittal oblique view is often superior for visualizing the needle tip and its path through the ligamentum flavum into the epidural space during in-plane guidance.
Ultrasound-Guided Neuraxial Anesthesia - Smooth Sailing Scans
- Benefits: ↑ success rates, ↓ needle passes & complications. Crucial for difficult neuraxial access (obesity, scoliosis, prior surgery).
- Views & Landmarks:
- Paramedian Sagittal (PMS): "Sawtooth" sign (laminae), ligamentum flavum-dura complex.
- Transverse Interlaminar (TI): "Flying bat" sign (spinous process, laminae).
- Technique: Pre-procedural marking or real-time needle guidance.
- Key Structures: Ligamentum flavum, epidural space, dura mater.
- Troubleshooting: Optimize probe (frequency, depth, gain), patient positioning; consider hydrodissection for difficult advancement.
⭐ Ultrasound guidance significantly reduces needle passes and improves first-attempt success in neuraxial blockade, especially in predicted difficult spinal anesthesia.
High‑Yield Points - ⚡ Biggest Takeaways
- Ultrasound guidance boosts neuraxial block success rates and reduces attempts.
- Crucial for obese patients and difficult spinal anatomy (e.g., scoliosis).
- Essential views: Paramedian Sagittal Oblique (PSO) and Transverse Median (TM).
- Accurate level identification via "counting up" from sacrum or "down" from T12.
- Pre-scan maps midline, depth to epidural space, and best needle path.
- Real-time needle tracking improves safety, minimizing traumatic punctures and reducing PDPH.
- Visualizes key structures: ligamentum flavum, epidural space, dura mater.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

