Cerebral Blood Flow & Metabolism - Brain's Balancing Act
- Cerebral Blood Flow (CBF):
- Normal: 50 mL/100g/min (≈15% Cardiac Output).
- Thresholds: EEG changes <20-25; Irreversible damage <10 mL/100g/min.
- Formula: $CBF = CPP / CVR$. (CPP = MAP - ICP or CVP).
- Cerebral Metabolic Rate (CMRO2):
- Normal: 3.0-3.8 mL O2/100g/min.
- Coupled with CBF (flow-metabolism coupling).
- Temperature: CMRO2 ↓ by 7% per 1°C ↓ in body temperature.
- Anesthetics: Most ↓ CMRO2 (e.g., propofol, barbiturates); Ketamine ↑ CMRO2.
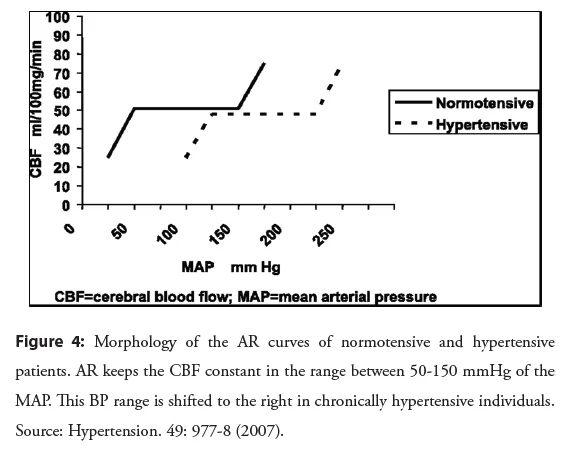
- Autoregulation:
- Maintains CBF constant over MAP range 50-150 mmHg.
- Curve shifts right in chronic hypertension.
- Key CBF Modulators:
- $PaCO_2$: Most potent. CBF changes 1-2 mL/100g/min per 1 mmHg $PaCO_2$ change (effective range 20-80 mmHg).
- $PaO_2$: Significant CBF↑ only if $PaO_2$ < 50 mmHg.
⭐> Hyperventilation (↓$PaCO_2$) rapidly ↓CBF and can be used to acutely ↓Intracranial Pressure (ICP), but prolonged use risks cerebral ischemia.
Intracranial Pressure Dynamics - Skull's Squeeze
- Intracranial Pressure (ICP): Pressure within the cranium. Normal: 5-15 mmHg.
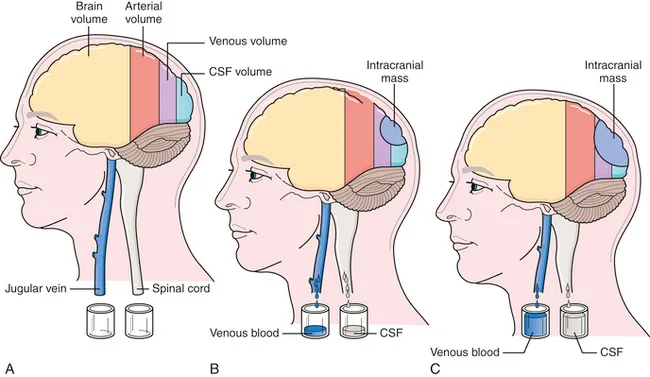
- Monro-Kellie Doctrine: Skull is a rigid box. $V_{Total} = V_{Brain} + V_{Blood} + V_{CSF} = Constant$.
- Increase in one component requires decrease in another(s) to maintain normal ICP.
- Compensation: CSF displacement, ↓ venous blood.
- Decompensation: Small volume ↑ → large ICP ↑.
- Intracranial Hypertension (ICH): Sustained ICP > 20-25 mmHg.
- Leads to ↓ Cerebral Perfusion Pressure (CPP), ischemia, herniation.
- ICP Waveform: P1 (percussion), P2 (tidal), P3 (dicrotic). P2 > P1 indicates ↓ compliance.
- Cushing's Triad: Hypertension, Bradycardia, Irregular Respirations. 📌 Mnemonic: HBI.
⭐ Cushing's triad is a LATE sign of severely increased ICP, indicating brainstem compression.
Cerebral Protection - Brain Shield Tactics
- Core Goal: Preserve neuronal integrity, prevent secondary brain injury.
- Key Strategies (Brain SHIELD 📌):
- Supply Oxygen & Optimize Perfusion:
- CPP: Target $CPP = MAP - ICP > \textbf{60-70 mmHg}$.
- Oxygenation: PaO₂ $>\textbf{100 mmHg}$; Normocapnia (PaCO₂ 35-40 mmHg).
- Hypothermia (Therapeutic):
- Mild (32-34°C) for specific conditions (e.g., post-cardiac arrest).
- ICP Control:
- Osmotic agents: Mannitol (0.25-1 g/kg), hypertonic saline.
- CSF drainage (EVD); surgical decompression.
- Electrical Stability & Glucose:
- Seizure prophylaxis (TBI).
- Glycemic control.
- Lower Metabolic Demand (↓CMRO₂):
- Sedatives: Barbiturates, propofol (burst suppression).
- Drugs (Specific):
- Lidocaine: blunts ICP rise (airway).
- Supply Oxygen & Optimize Perfusion:
⭐ Barbiturates (e.g., thiopental) induce "pharmacological coma," maximally reducing CMRO₂ by ~50%, decreasing excitotoxicity, offering potent neuroprotection.
Neuro-Pathophysiology Snippets - Anesthetic Alerts
- Raised ICP (>20 mmHg)
- Normal: 5-15 mmHg.
- Signs: Headache, vomiting, papilledema, ↓GCS.
- Cushing's Triad (late): Hypertension, bradycardia, irregular respirations.
- Anesthetic: Maintain CPP ($CPP = MAP - ICP$), avoid ICP spikes (smooth induction/extubation, no coughing).
- Cerebral Edema
- Types: Vasogenic, Cytotoxic.
- Rx: Head up, mannitol, hypertonic saline, hyperventilation (PaCO2 30-35 mmHg, transient).
- Cerebral Vasospasm
- Post-SAH (days 4-14).
- Rx: Maintain normovolemia, induced hypertension.
- Seizures
- Intraop Rx: Propofol, thiopental, benzodiazepines.
- EEG if high risk.
⭐ Cushing's triad (hypertension, bradycardia, irregular respirations) is a late sign of severely raised ICP, indicating brainstem compression.
High‑Yield Points - ⚡ Biggest Takeaways
Error: Failed to generate content for this concept group.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

