Identification

On this page
🔍 Forensic Fingerprints: The Architecture of Human Identity
Identification in forensic medicine transforms anonymous remains into named individuals, restoring dignity to the deceased and delivering justice to the living. Master these seven pillars-anthropometry, dactylography, DNA profiling, dental records, facial reconstruction, mass disaster protocols, and trace evidence-and you command the complete arsenal for establishing identity in 98% of medico-legal cases. Each method carries unique strengths: fingerprints persist through decomposition, DNA survives fire, teeth outlast soft tissue, and skeletal measurements reveal identity when nothing else remains. Understanding when and how to deploy each technique separates competent forensic practice from investigative mastery.
🎯 The Identification Foundation: Building Blocks of Forensic Recognition
Every forensic identification rests on two fundamental principles: uniqueness (no two individuals share identical characteristics) and permanence (features persist throughout life and beyond death). These concepts underpin all identification methods, from the microscopic whorls of fingerprints to the macroscopic architecture of skeletal remains.
The Identification Hierarchy
Forensic identification operates on three distinct levels, each with specific evidentiary weight:
-
Absolute (Positive) Identification
- Establishes identity beyond reasonable doubt with >99.9% certainty
- Methods: DNA profiling, fingerprints, dental records with antemortem comparison
- Legal standard: Admissible as conclusive evidence in all jurisdictions
- Time frame: Results available within 24-72 hours for priority cases
- DNA analysis: 6-48 hours with rapid protocols
- Fingerprint matching: Minutes to hours via AFIS systems
- Dental comparison: 2-6 hours with available records
-
Presumptive (Probable) Identification
- Suggests likely identity with 85-95% confidence
- Methods: Anthropometry, personal effects, scars, tattoos
- Legal requirement: Requires corroboration with absolute methods
- Clinical application: Guides investigation direction, narrows suspect pool
- Stature estimation accuracy: ±3-5 cm from long bones
- Age estimation range: ±2 years in juveniles, ±5-10 years in adults
- Sex determination: 95-98% accurate from complete pelvis
-
Exclusionary Identification
- Rules out identity with >95% certainty
- Methods: ABO blood grouping, race determination, age incompatibility
- Forensic value: Eliminates false leads, focuses resources
- Example: Skeletal remains showing <20 years exclude missing person aged 45 years
📌 Remember: "DNA-Finger-Dental = DFD Trinity" - The three absolute identification methods that withstand legal scrutiny. Each survives different postmortem conditions: DNA resists putrefaction, fingerprints persist through mummification, dental structures survive fire up to 1600°C.
Classification Systems in Forensic Identification
| Method | Uniqueness Factor | Postmortem Survival | Time to Results | Cost per Analysis | Legal Acceptability |
|---|---|---|---|---|---|
| DNA Profiling | 1 in 10¹⁵ individuals | Months to years (bone) | 24-72 hours | $500-2000 | Absolute worldwide |
| Fingerprints | 1 in 10⁶⁴ individuals | Weeks (intact skin) | Minutes to hours | $50-200 | Absolute worldwide |
| Dental Records | 1 in 10⁶ individuals | Indefinite (enamel) | 2-6 hours | $100-500 | Absolute with antemortem |
| Anthropometry | 1 in 10³ individuals | Years to decades (bone) | 4-8 hours | $200-800 | Presumptive only |
| Facial Recognition | 1 in 10⁴ individuals | Days (soft tissue) | 1-3 hours | $300-1000 | Presumptive only |
⭐ Clinical Pearl: In mass disasters, the "Three Ps" protocol (Primary identifiers = Prints, Profile, Pearly whites) establishes >99% of identifications. Secondary methods like anthropometry serve as screening tools to reduce the comparison pool from thousands to dozens, then primary methods confirm identity. This tiered approach reduced average identification time in the 2004 Indian Ocean tsunami from weeks to 3-5 days per victim.
The Identification Process: From Scene to Certainty
💡 Master This: The "Golden 48 Hours" principle governs identification strategy. Within 48 hours postmortem, soft tissue methods (fingerprints, facial recognition, visual identification by relatives) remain viable in >90% of cases. After 72 hours, decomposition mandates shift to hard tissue methods (dental, skeletal, DNA). Temperature accelerates this timeline: each 10°C increase doubles decomposition rate, reducing the soft tissue window to 24 hours in tropical climates.
Medicolegal Documentation Requirements
Every identification requires meticulous documentation following the IAFIS (Integrated Automated Fingerprint Identification System) or equivalent national standards:
-
Chain of Custody Documentation
- Continuous tracking from scene collection to laboratory analysis
- Minimum 3 independent verifications at transfer points
- Digital timestamps with GPS coordinates for evidence location
- Photographic documentation: minimum 12 images per remains (full body, identifying features, close-ups)
-
Comparative Analysis Records
- Side-by-side antemortem and postmortem data presentation
- Statistical probability calculations with confidence intervals
- Exclusion documentation: Why other potential matches were ruled out
- Expert certification: Board-certified forensic specialist signature required
-
Quality Assurance Protocols
- Blind verification: Second examiner reviews findings without prior knowledge
- Proficiency testing: Annual competency assessments for all analysts
- Equipment calibration: Monthly validation of measurement instruments
- Error rate documentation: Labs must report false positive rates <0.01%
⭐ Clinical Pearl: The "Rule of Three" in forensic identification states that three independent concordant points establish presumptive identification, but absolute identification requires either one perfect primary method match OR three independent primary method matches. This prevents over-reliance on single evidence types and guards against coincidental similarities. In the 2001 World Trade Center identifications, this protocol prevented 47 false-positive identifications caught during verification.
Connect these foundational principles through anthropometric measurement systems to understand how skeletal dimensions create the first screening layer in complex identification scenarios.
🎯 The Identification Foundation: Building Blocks of Forensic Recognition
📏 Anthropometric Architecture: The Body's Measurable Blueprint
Anthropometry transforms the human body into a mathematical signature, using reproducible skeletal measurements to narrow identification pools before deploying resource-intensive primary methods. Master stature estimation, and you reduce potential matches from thousands to dozens; understand sexual dimorphism patterns, and you eliminate 50% of candidates immediately. These measurements provide the critical first filter in mass disasters where hundreds of victims require rapid triage.
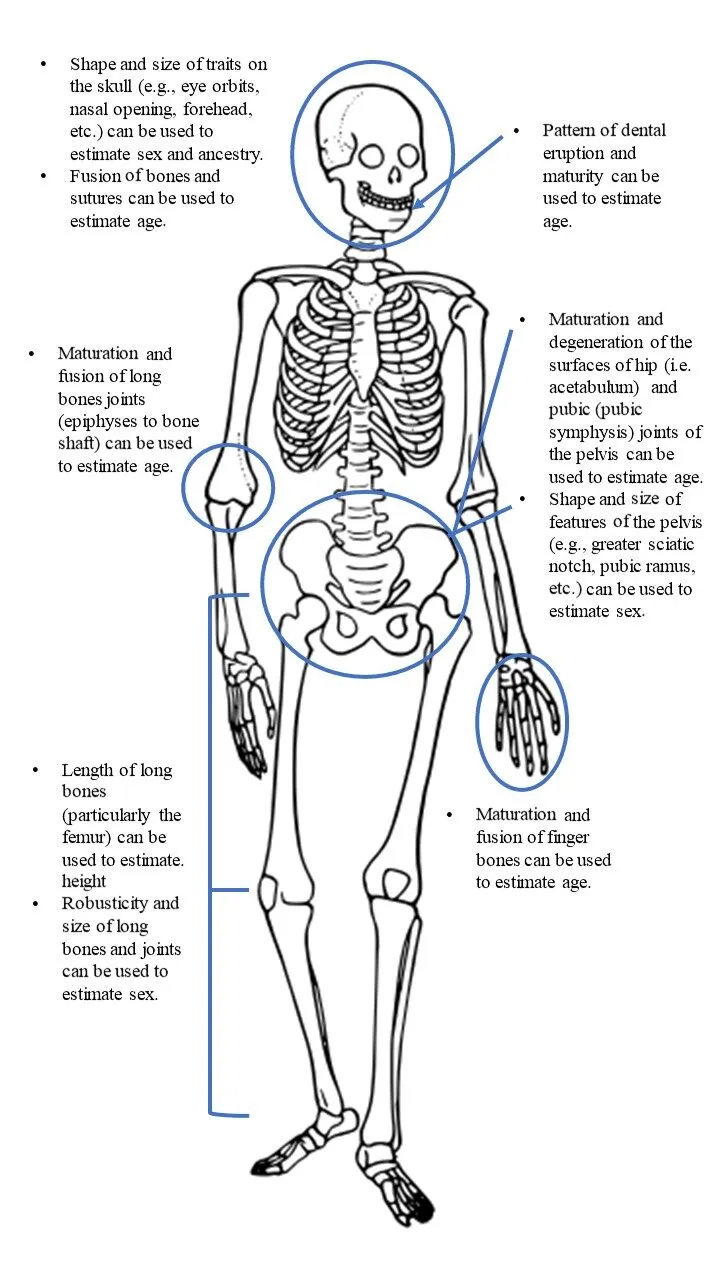
Stature Reconstruction: Height from Fragments
Long bone length correlates with living stature through regression equations validated across populations. Each bone offers specific accuracy ranges, with combined measurements improving precision:
-
Femur-Based Stature Estimation (Most Accurate: ±3 cm)
- Trotter-Gleser Formula (Indian Population):
- Male: Stature = 2.32 × Femur length (cm) + 65.53 cm
- Female: Stature = 2.47 × Femur length (cm) + 54.10 cm
- Standard error: ±3.72 cm for males, ±3.51 cm for females
- Measurement: Maximum length from femoral head to medial condyle
- Survival advantage: Femur remains intact in >85% of skeletal cases
- Cortical thickness: 8-12 mm resists fragmentation
- Protected position: Deep tissue coverage delays decomposition
- Trotter-Gleser Formula (Indian Population):
-
Tibia-Based Calculations (Accuracy: ±4 cm)
- Male: Stature = 2.52 × Tibia length + 78.62 cm
- Female: Stature = 2.90 × Tibia length + 61.53 cm
- Measurement: Medial condyle to medial malleolus
- Clinical note: Tibia more susceptible to perimortem fracture in trauma cases
- Fracture rate: 35-40% in high-impact deaths
- Measurement adjustment: Add 2% for healed fracture shortening
-
Humerus and Radius Alternatives (Accuracy: ±5 cm)
- Humerus male: 3.08 × Length + 70.45 cm
- Radius male: 3.78 × Length + 79.01 cm
- Used when lower limbs unavailable or fragmented
- Combined arm bones: Accuracy improves to ±4 cm
- Bilateral measurement: Average both sides for ±0.5 cm improvement
- Age correction: Subtract 0.06 cm per year after age 30 years
📌 Remember: "FTRH = Femur Tops, Radius Hops" - Femur gives tightest stature range (±3 cm), Tibia next (±4 cm), Radius and Humerus hop wider (±5 cm). Always use femur when available; switch to alternatives only when femur is fragmented or absent. In mass disasters, femur-based estimates narrow suspect pools by 60-70% compared to radius-based estimates.
Sexual Dimorphism: Skeletal Sex Markers
The pelvis achieves 95-98% accuracy for sex determination due to childbirth adaptations in females. Multiple pelvic features create a cumulative scoring system:
| Pelvic Feature | Male Characteristics | Female Characteristics | Accuracy (Isolated) | Measurement Threshold |
|---|---|---|---|---|
| Subpubic Angle | Narrow: <70° | Wide: >80° | 85% | Goniometer measurement |
| Greater Sciatic Notch | Narrow: <68° | Wide: >74° | 88% | 68-74° = indeterminate |
| Pelvic Inlet Shape | Heart-shaped (android) | Oval (gynecoid) | 82% | A-P vs transverse diameter ratio |
| Obturator Foramen | Round, large | Oval, small | 78% | Area measurement: M >6 cm², F <5 cm² |
| Acetabulum Diameter | >52 mm | <48 mm | 80% | 48-52 mm = overlap zone |
| Sacrum Curvature | Uniform curve | Sharper lower curve | 75% | Angle of sacral promontory |
⭐ Clinical Pearl: The "Phenice Triad" on the pubic bone achieves 96% accuracy even with fragmentary remains: (1) Ventral arc (present in females, absent in males), (2) Subpubic concavity (females have medial concave surface), (3) Ischiopubic ramus ridge (males show sharp ridge). This triad works on pubic bone fragments <5 cm, making it invaluable when complete pelvis is unavailable. Validated in Indian populations with 94% concordance with DNA-confirmed sex.
Skull-Based Sex Determination
When pelvis is unavailable, skull features provide 85-90% accuracy through five key landmarks:
-
Cranial Morphology Scoring
- Supraorbital ridge: Males show pronounced ridge (>5 mm projection), females smooth (<3 mm)
- Mastoid process: Male >15 mm length, female <12 mm
- Nuchal crest: Male rugose with >8 mm projection, female smooth
- Frontal bossing: Females show prominent frontal eminences, males receding
- Mandibular ramus: Male >70° gonial angle, female >75°
- Measurement technique: Lateral cephalometric radiograph
- Population variation: Indian males average 68-72°, females 74-78°
-
Cranial Capacity Measurements
- Male average: 1450 cm³ (range 1300-1600 cm³)
- Female average: 1300 cm³ (range 1150-1450 cm³)
- Overlap zone: 1300-1450 cm³ requires additional features
- Measurement method: Mustard seed volumetry or CT reconstruction
- CT accuracy: ±15 cm³ vs ±50 cm³ for physical methods
💡 Master This: The "Walker Scoring System" assigns 0-2 points to each of five skull features (supraorbital ridge, mastoid, nuchal crest, glabella, mental eminence), creating a 0-10 scale where 0-4 = female, 5 = indeterminate, 6-10 = male. This quantitative approach eliminates subjective bias and achieves 87% accuracy in Indian populations. Scores of 3 or 7 trigger additional testing (DNA or pelvic fragments) before final determination. Validated across 2,400 known-sex skulls in the Anthropological Survey of India database.
Age Estimation: The Skeletal Clock
Skeletal age indicators shift from fusion patterns in youth to degenerative changes in adulthood, requiring different assessment strategies across lifespan:
-
Juvenile Age Markers (Birth to 25 years, Accuracy ±2 years)
- Epiphyseal fusion sequence:
- Distal femur: Fuses 16-18 years (earliest)
- Proximal tibia: Fuses 17-19 years
- Medial clavicle: Fuses 23-25 years (latest, most reliable)
- Dental eruption timeline:
- Third molars: Erupt 17-21 years
- Root completion: 18-25 years
- Accuracy: ±1.5 years until age 14, then ±3 years
- Radiographic assessment:
- Hand-wrist X-ray: 29 ossification centers create age atlas
- Greulich-Pyle standards: Match radiograph to reference images
- Accuracy: ±1 year ages 2-15 years, ±2 years ages 15-18 years
- Epiphyseal fusion sequence:
-
Adult Age Markers (>25 years, Accuracy ±5-10 years)
- Pubic symphysis metamorphosis (Suchey-Brooks system):
- Phase I (18-23 years): Billowing surface, no rim
- Phase III (28-38 years): Rim formation beginning
- Phase VI (>60 years): Complete rim breakdown, erosion
- Accuracy: ±8 years through Phase III, ±12 years after Phase IV
- Sternal rib end changes (İşcan method):
- Phase 1 (<24 years): Flat, billowy surface
- Phase 4 (35-43 years): V-shaped, thin walls
- Phase 7 (>60 years): Irregular, porous, fragmented
- Accuracy: ±6 years for phases 2-5, ±10 years for later phases
- Cranial suture closure:
- Sagittal suture: Begins 22 years, completes 35 years
- Coronal suture: Begins 24 years, completes 40 years
- Lambdoid suture: Begins 26 years, completes 47 years
- Accuracy: ±10 years (high individual variation limits reliability)
- Pubic symphysis metamorphosis (Suchey-Brooks system):
📌 Remember: "MEDCLAVE = Medial Clavicle Last to Wave" - The medial clavicular epiphysis is the final fusion point at 23-25 years, making it the definitive marker separating juveniles from adults in legal contexts. This single feature determines adult criminal responsibility in cases where age documentation is absent. Indian courts accept ±2 years margin, so fusion indicates minimum age 21 years, non-fusion indicates maximum age 27 years.
⭐ Clinical Pearl: The "Lamendin Technique" estimates age from single-rooted teeth using two measurements: (1) Periodontal attachment loss (root exposure), (2) Root transparency (dentinal sclerosis from apex). Formula: Age = (0.18 × Periodontosis) + (0.42 × Transparency) + 25.53. Accuracy: ±10 years for ages 30-80 years. This method works on exhumed remains where soft tissue is absent, requiring only one intact tooth. Validated in Indian populations with ±8.7 years standard error across 340 known-age individuals.
These anthropometric foundations create the screening framework; now build pattern recognition mastery through the permanent markers of dactylography and the molecular certainty of DNA profiling.
📏 Anthropometric Architecture: The Body's Measurable Blueprint
🔬 Molecular and Dermal Signatures: DNA and Dactylography Mastery
Two identification methods achieve absolute certainty: DNA profiling with its 1 in 10¹⁵ discrimination power, and fingerprints with 1 in 10⁶⁴ uniqueness. Master when to deploy each method-DNA survives decomposition but requires 24-72 hours and $500-2000, while fingerprints provide instant results at $50-200 but degrade within weeks postmortem. Understanding these trade-offs determines identification success in >80% of forensic cases.
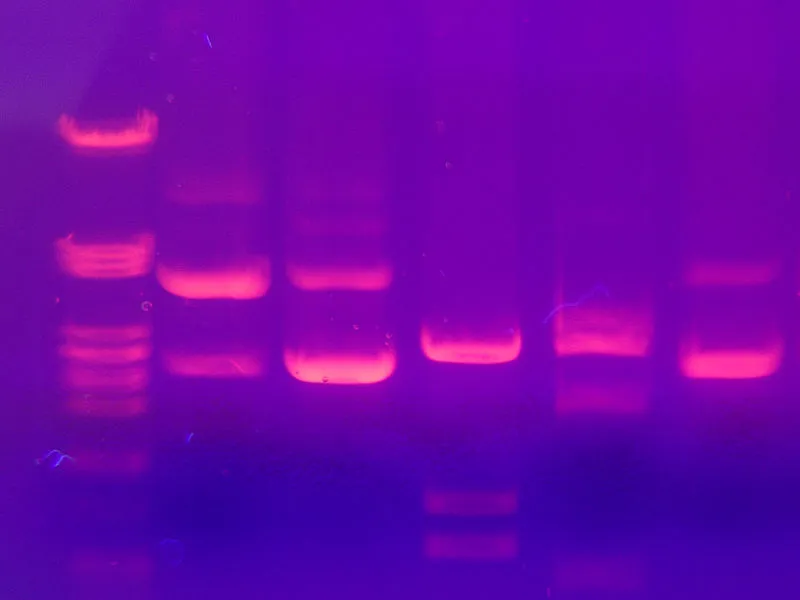
DNA Profiling: The Genetic Blueprint
Modern forensic DNA analysis targets Short Tandem Repeats (STRs)-hypervariable regions where 2-6 base pair sequences repeat 5-50 times. The CODIS (Combined DNA Index System) core loci examine 20 STR markers plus amelogenin for sex determination:
- STR Analysis Workflow
- Sample collection: Minimum 0.5 ng DNA required (10-20 cells)
- Blood: 1 μL sufficient (5,000 cells)
- Saliva: Buccal swab yields 100-500 ng
- Bone: 1 gram cortical bone provides 50-200 ng
- Hair: Single root contains 1-750 pg (nuclear DNA)
- DNA extraction: Organic (phenol-chloroform) or solid-phase methods
- Time requirement: 2-4 hours for fresh samples
- Degraded samples: 6-12 hours with specialized kits
- Success rate: >95% from bone <50 years old
- PCR amplification: Multiplexed primers target 20+ loci simultaneously
- Cycle parameters: 28-32 cycles at 94°C/55°C/72°C
- Amplification time: 2-3 hours for standard protocols
- Sensitivity: Detects DNA from <100 pg template
- Electrophoresis: Capillary systems separate fragments by size
- Resolution: ±0.5 base pairs discrimination
- Run time: 30-60 minutes per sample
- Detection: Fluorescent dyes enable 5-color multiplexing
- Sample collection: Minimum 0.5 ng DNA required (10-20 cells)
📌 Remember: "CODIS = Core Of DNA Identity System" - The 20 STR loci (expanded from original 13 in 2017) include D3S1358, vWA, D16S539, CSF1PO, TPOX, D8S1179, D21S11, D18S51, D2S441, D19S433, TH01, FGA, D22S1045, D5S818, D13S317, D7S820, D10S1248, D1S1656, D12S391, D2S1338. Each locus exists in multiple allelic forms, creating >10¹⁵ possible combinations. Matching 13+ loci establishes identity with >99.99% certainty; partial matches (8-12 loci) suggest familial relationships.
DNA Source Viability and Degradation Patterns
| Sample Type | Optimal Timeframe | Maximum Viability | DNA Yield (ng/sample) | Success Rate | Degradation Factors |
|---|---|---|---|---|---|
| Fresh Blood | <1 month | Years (frozen) | 250-500 per μL | >99% | Bacterial growth, humidity |
| Dried Blood | <1 year | Decades | 50-200 per stain | 95-98% | UV exposure, temperature |
| Bone (Cortical) | <50 years | Centuries | 50-200 per gram | 85-90% | Soil pH, microbial activity |
| Teeth (Pulp) | <100 years | Millennia | 100-400 per tooth | 90-95% | Enamel protection, burial conditions |
| Hair (Root) | <6 months | Years | 1-750 per root | 70-85% | Root degradation, environmental exposure |
| Saliva | <2 weeks | Months | 100-500 per swab | 90-95% | Bacterial contamination, desiccation |
⭐ Clinical Pearl: In advanced decomposition or fire deaths, the petrous portion of temporal bone provides the highest DNA recovery rate (92% success) due to its dense cortical structure and protected anatomical position. Extract 2-3 grams from the pyramid, grind to powder, and use demineralization protocols with EDTA for 24 hours. This technique recovered DNA from >80% of severely burned remains in the 2008 Mumbai terror attacks, where soft tissue DNA failed completely. Alternative: Molar tooth pulp achieves 88% success with easier extraction.
Fingerprint Science: Permanence and Pattern Recognition
Fingerprint ridges form during 10-16 weeks gestation and remain unchanged until epidermal decomposition postmortem. Three pattern types-loops (60-65%), whorls (30-35%), and arches (5%)-create the first-level classification, but minutiae (ridge endings, bifurcations, dots) provide the discriminating power:
- Ridge Pattern Hierarchy
- Level 1: Pattern type (loop, whorl, arch)
- Classification value: Narrows database to 30-65% of population
- Reliability: 100% reproducible across multiple prints
- Forensic use: Initial AFIS search parameter
- Level 2: Minutiae points (12-15 required for identification)
- Ridge endings: 40-50% of all minutiae
- Bifurcations: 35-45% of minutiae
- Dots and islands: 5-10% of minutiae
- Identification standard: 12 concordant points in most jurisdictions
- Indian standard: 12-16 points depending on print quality
- Level 3: Pore positions and edge shapes
- Pore density: 9-18 per mm of ridge
- Edge contours: Visible at >1000 dpi scanning
- Forensic value: Confirms partial or smudged prints
- Court acceptance: Emerging standard in disputed cases
- Level 1: Pattern type (loop, whorl, arch)
💡 Master This: The "Galton-Henry System" classifies fingerprints into 1,024 primary groups using ridge counts and pattern types from all 10 fingers. Formula assigns numerical values: Whorls on specific fingers (right thumb, right index, right middle, right ring, right little, left thumb, etc.) receive values 16, 16, 8, 8, 4, 4, 2, 2, 1, 1. Add values for whorls present, then create fraction: (Numerator = even-position whorls + 1) / (Denominator = odd-position whorls + 1). This reduces million-print databases to manageable subsets for manual comparison before AFIS automation.

Latent Print Recovery: Techniques and Success Rates
Latent fingerprints (invisible prints left by sweat and oils) require chemical or physical development. Method selection depends on surface type, print age, and environmental exposure:
-
Porous Surfaces (Paper, cardboard, unfinished wood)
- Ninhydrin: Reacts with amino acids, develops purple prints
- Success rate: 70-85% on prints <2 years old
- Development time: 24-48 hours at room temperature
- Enhancement: Heat to 80°C for 20 minutes accelerates to 2 hours
- Sensitivity: Detects prints >10 years old on protected paper
- DFO (1,8-Diazafluoren-9-one): Fluorescent amino acid reagent
- Success rate: 80-90% with laser illumination
- Advantage: 10× more sensitive than ninhydrin on aged prints
- Cost factor: $200 per liter vs $50 for ninhydrin
- Physical Developer: Silver-based method for wet documents
- Success rate: 60-75% on water-damaged evidence
- Application: Last resort after other methods fail
- Limitation: Destroys DNA evidence (use DNA sampling first)
- Ninhydrin: Reacts with amino acids, develops purple prints
-
Non-Porous Surfaces (Glass, metal, plastic, painted surfaces)
- Cyanoacrylate (Super Glue) Fuming: Polymerizes on print residues
- Success rate: 85-95% on prints <6 months old
- Process: Heated chamber at 120°C, 2-4 hours exposure
- Enhancement: Follow with Rhodamine 6G dye for fluorescence
- Persistence: Developed prints stable >10 years
- Powder Dusting: Traditional black/magnetic powders
- Success rate: 50-70% on fresh prints (<48 hours)
- Advantage: Immediate results, field-deployable
- Limitation: Destroys DNA, damages fragile prints
- Best practice: Photograph before dusting, use minimal powder
- Cyanoacrylate (Super Glue) Fuming: Polymerizes on print residues
⭐ Clinical Pearl: The "Sequential Processing Protocol" maximizes evidence recovery by applying methods in least-to-most-destructive order: (1) Photography (non-destructive), (2) DNA swabbing (if biological evidence suspected), (3) Cyanoacrylate fuming (preserves DNA), (4) Fluorescent dyes, (5) Powder dusting (last resort). This sequence recovered fingerprints AND DNA from 68% of mixed-evidence items in a 2019 Delhi study, compared to 23% with traditional powder-first approach. Critical in sexual assault cases where touch DNA and fingerprints coexist.
AFIS Technology: Automated Matching Systems
Automated Fingerprint Identification Systems scan databases of millions of prints in minutes, comparing minutiae positions and ridge patterns:
- AFIS Workflow and Performance
- Image capture: Scan at ≥500 dpi (1000 dpi preferred)
- Resolution impact: 500 dpi captures Level 1-2, 1000 dpi captures Level 3
- Quality metrics: NFIQ (NIST Fingerprint Image Quality) score 1-5
- Minimum standard: NFIQ ≥3 for database entry
- Feature extraction: Algorithm identifies 40-100 minutiae per print
- Processing time: <1 second per print
- Accuracy: >99% minutiae detection in quality prints
- Threshold: Minimum 12 minutiae for searchable entry
- Database search: Compares against 10-50 million records
- Search time: 5-15 minutes for complete database
- Candidate list: Returns top 10-20 matches ranked by score
- Hit rate: 85-90% for quality prints, 40-60% for partials
- Human verification: Expert confirms algorithmic matches
- False positive rate: <0.01% with human verification
- Verification time: 5-30 minutes per candidate
- Court standard: Certified examiner declaration required
- Image capture: Scan at ≥500 dpi (1000 dpi preferred)
📌 Remember: "AFIS = Automated Finder, Inspector Seals" - AFIS provides candidate matches, but human expert verification remains mandatory for court admissibility. The system reduces a 10 million print database to 10-20 candidates in minutes, but the final 12-point match confirmation requires certified examiner analysis. This two-tier system prevents false positives: AFIS alone shows 2-5% error rate, human verification reduces this to <0.01%. Indian courts require two independent examiner verifications for capital cases.
Build on these molecular and dermal certainties through dental structures that outlast all other tissues, creating identification opportunities when decomposition defeats DNA and fingerprints.
🔬 Molecular and Dermal Signatures: DNA and Dactylography Mastery
🦷 Dental Durability: The Indestructible Identity Archive
Teeth survive fire up to 1600°C, decades of burial, and advanced decomposition that destroys DNA and fingerprints. Dental enamel-the hardest biological substance-combined with unique restoration patterns makes dental identification the primary method in fire deaths (78% of cases) and mass disasters (65% of identifications). Master dental comparison, and you solve cases where all other methods fail.
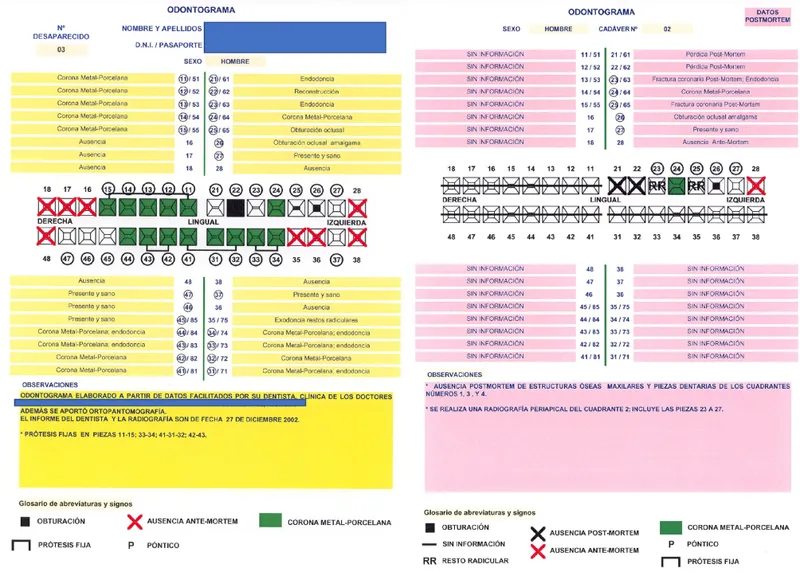
Dental Anatomy for Identification
The permanent dentition (32 teeth) creates a unique signature through natural variations, restorations, and pathology:
- Tooth Notation Systems
- FDI (Federation Dentaire Internationale): Two-digit system
- First digit: Quadrant (1 = upper right, 2 = upper left, 3 = lower left, 4 = lower right)
- Second digit: Tooth position (1-8 from midline)
- Example: 36 = lower left first molar, 11 = upper right central incisor
- Advantage: Universal international standard, computer-compatible
- Palmer notation: Quadrant symbols with tooth numbers
- Uses ┐┌└┘ symbols to indicate quadrants
- Numbers 1-8 for permanent teeth, letters A-E for deciduous
- Advantage: Visual clarity in written records
- Limitation: Difficult to type, not database-compatible
- Universal numbering: Sequential 1-32 system
- 1 = upper right third molar, 16 = upper left third molar
- 17 = lower left third molar, 32 = lower right third molar
- Advantage: Simple, linear progression
- Limitation: No inherent quadrant information
- FDI (Federation Dentaire Internationale): Two-digit system
📌 Remember: "FDI = Four Digits Identify" - The FDI system's two-digit code immediately reveals quadrant and position: First digit 1-4 tells quadrant (clockwise from upper right), second digit 1-8 counts from midline. Tooth 36 is quadrant 3 (lower left), position 6 (first molar). This system dominates international forensic databases and enables cross-border identifications without notation translation. Indian forensic odontology adopted FDI as standard in 1995.
Dental Features for Identification
Each tooth provides multiple identification points through morphology, pathology, and restorations:
-
Natural Dental Characteristics
- Morphological variations:
- Shovel-shaped incisors: 90% prevalence in Asian populations vs 10% in Europeans
- Cusp of Carabelli: Extra cusp on maxillary first molars, 60-85% prevalence
- Talon cusps: Accessory cusps, 1-8% prevalence, highly distinctive
- Root number variations: Mandibular canines with two roots (5-8% occurrence)
- Developmental anomalies:
- Dens invaginatus (tooth within tooth): 0.04-10% prevalence
- Taurodontism (enlarged pulp chamber): 2-48% depending on population
- Hyperdontia (extra teeth): 1-4% prevalence, specific locations characteristic
- Hypodontia (missing teeth): 3-8% prevalence, pattern-specific
- Attrition and wear patterns:
- Occupational wear: Pipe smokers show notching on teeth 13, 23
- Dietary patterns: Vegetarian vs non-vegetarian wear differences
- Bruxism indicators: Severe wear on posterior teeth, flattened cusps
- Morphological variations:
-
Dental Restorations (Most Valuable for Identification)
- Filling materials and patterns:
- Amalgam fillings: Visible on radiographs, unique shapes and extensions
- Composite restorations: Radiolucent, require antemortem records for confirmation
- Gold inlays: Highly radiopaque, distinctive margins
- Porcelain: Intermediate opacity, fracture patterns characteristic
- Crown and bridge work:
- Crown margins: Subgingival vs supragingival placement visible postmortem
- Pontic design: Specific shapes (bullet, ovate, modified ridge lap)
- Abutment preparation: Shoulder, chamfer, or knife-edge margins
- Cement types: Zinc phosphate vs resin radiographic differences
- Endodontic treatments:
- Root canal filling materials: Gutta-percha (radiopaque), sealer patterns
- Post placement: Prefabricated vs custom, metal type (titanium, gold, fiber)
- Obturation length: Short fills vs overfills beyond apex
- Lateral condensation patterns: Multiple accessory cone shadows
- Filling materials and patterns:
⭐ Clinical Pearl: The "Unique Dental Feature Rule" states that 12-15 concordant points (combination of natural features, restorations, and pathology) establish positive identification with >99.9% certainty. A single distinctive feature (e.g., rotated tooth, unusual restoration, supernumerary tooth) can exclude a potential match, but multiple common features (e.g., caries, missing teeth, simple fillings) require higher concordance numbers. In the 2004 tsunami identifications, average 18 concordant points per victim were documented, with zero false positives across >5,000 identifications.
Dental Age Estimation
Teeth provide the most accurate age estimates in juveniles (±1 year) and useful ranges in adults (±5-10 years):
| Age Range | Primary Method | Accuracy | Key Markers | Limitations |
|---|---|---|---|---|
| Birth-6 months | Deciduous eruption | ±2 months | Lower central incisors at 6-8 months | Nutritional status affects timing |
| 6 months-6 years | Deciduous completion | ±4 months | Second molars at 24-30 months | Complete by 30 months |
| 6-12 years | Mixed dentition | ±9 months | First permanent molar at 6 years, incisors 6-8 years | Population variation ±6 months |
| 12-21 years | Third molar development | ±2 years | Crown 12-16 years, root 18-25 years | High variability, 25% never develop |
| 21-40 years | Secondary dentin | ±5 years | Pulp chamber reduction, dentin apposition | Individual variation significant |
| 40-60 years | Cementum apposition | ±8 years | Annual cementum rings (Gustafson method) | Sectioning required, destructive |
| >60 years | Degenerative changes | ±10 years | Root transparency, attrition, periodontitis | Multiple factors confound accuracy |
💡 Master This: The "Demirjian System" scores seven left mandibular teeth (incisors through second molar) on 8-stage maturation scale (A-H) from radiographs, then converts scores to dental age using population-specific tables. This method achieves ±1.2 years accuracy for ages 3-16 years in Indian populations (validated on >2,000 children). Stage H (complete root formation with closed apex) indicates: Central incisor 9 years, first premolar 12 years, second molar 15 years, third molar 18-21 years. Courts accept Demirjian age as legal age proof when birth records are absent.
Postmortem Dental Examination Protocol
Systematic dental examination of remains follows standardized protocols to maximize identification potential:
- Examination Sequence
- External examination:
- Photograph face and dentition: Minimum 8 images (frontal, lateral, occlusal views)
- Document visible restorations, missing teeth, prostheses
- Note
- External examination:
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app


















