Imaging Modalities - Pixel Power Play
Key imaging techniques for the female pelvis:
| Modality | Primary Use (Female Pelvis) | Strength | Weakness |
|---|---|---|---|
| TVS | Endometrial/ovarian detail, early preg. | ↑Resolution, no radiation | Limited Field of View (FOV), operator-dependent |
| TAS | Global pelvic survey, large masses | Wide FOV, non-invasive | ↓Resolution vs TVS, needs full bladder |
| MRI | Staging, complex masses, anomalies | Superior soft tissue, multiplanar | Cost, time, contraindications (metal) |
| CT | Trauma, acute pain, advanced Ca staging | Fast, widely available, bone detail | Radiation, ↓soft tissue contrast vs MRI |
| HSG | Infertility (tubal/uterine cavity eval) | Uterine/tubal morphology, dynamic | Radiation, discomfort, C/I (PID, preg) |
oka
Uterine Wonders & Woes - Womb Room Review
Müllerian Duct Anomalies (MDA) 📌 ASRM MDA (I-VII): "A Unique Doctor Brings Sweet Apples Daily."
- ASRM Classification:
ASRM Anomaly Key Feature I Hypoplasia/Agenesis Absent/rudimentary uterus II Unicornuate Single horn ± rud. horn III Didelphys 2 uteri, 2 cervices IV Bicornuate 2 horns, 1 cervix, cleft >1cm V Septate Cavity septum, normal ext. VI Arcuate Mild fundal indent <1cm VII DES Related T-shaped cavity
Fibroids (Leiomyomas)
- Types by location:
- Subserosal: Outer uterine wall; may be pedunculated.
- Intramural: Within myometrium (most common).
- Submucosal: Project into endometrial cavity; often symptomatic.
Endometrial Pathologies
- Endometrial Thickness (ET) - Transvaginal Ultrasound (TVS):
- Premenopausal: Variable (up to 16 mm secretory phase).
- Postmenopausal (with bleeding): >4-5 mm suspicious.
- Postmenopausal (no bleeding, no HRT): <5 mm generally normal.
- Postmenopausal (on HRT): <8 mm generally normal.
- Tamoxifen: Can be thicker (e.g., >8 mm), cystic changes common.
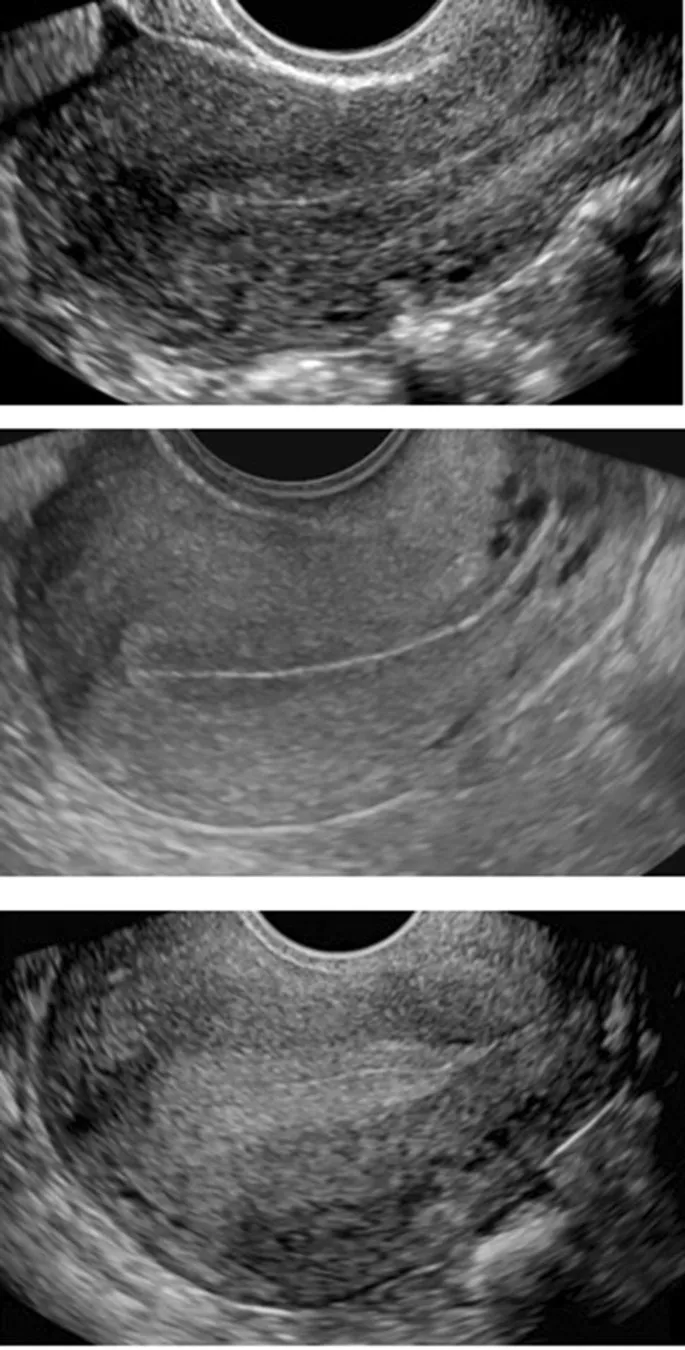
Adenomyosis
- Diffuse myometrial infiltration by endometrial glands/stroma.
⭐ Junctional zone (JZ) thickness >12 mm on T2W MRI is highly suggestive of adenomyosis (normal JZ <5 mm).
Ovarian & Adnexal Adventures - Ovary Odyssey
-
Polycystic Ovary Syndrome (PCOS) - Rotterdam Criteria (≥2 of 3):
- Oligo/anovulation
- Hyperandrogenism (clinical/biochemical)
- Polycystic ovaries on USG: ≥12 follicles (2-9mm)/ovary OR ovarian volume >10mL

-
Pelvic Inflammatory Disease (PID) Complications:
- Hydrosalpinx / Pyosalpinx
- Tubo-ovarian Abscess (TOA)
- Fitz-Hugh-Curtis syndrome (perihepatitis)

⭐ Fat, calcification, or Rokitansky nodule (dermoid plug) are pathognomonic for mature cystic teratoma (dermoid cyst) on imaging.
Ovarian Mass: Benign vs. Malignant (IOTA Simple Rules)
| Aspect | IOTA B-Rules (Benign if ALL present, NO M-Rules) | IOTA M-Rules (Malignant if ANY present) |
|---|---|---|
| Overall | Unilocular cyst | Irregular solid tumor; Ascites |
| Solid Comp. | Largest < 7mm | ≥4 papillary structures |
| Size/Contour | Smooth multilocular < 100mm | Irregular multilocular ≥100mm |
| Shadowing | Acoustic shadows present | - |
| Vascularity | No blood flow (Score 1) | Very strong blood flow (Score 4) |
Adnexal Mass Management (Simplified Algorithm):
High‑Yield Points - ⚡ Biggest Takeaways
- TVUS: Initial modality for most female pelvic pathologies.
- MRI: Superior for staging cervical & endometrial cancer.
- Ovarian torsion: Enlarged ovary, stromal edema, peripheral follicles; Doppler may show ↓/absent flow.
- PID: Can lead to tubo-ovarian abscess (TOA), a complex adnexal mass.
- Endometriomas: Unilocular cysts with homogenous low-level ("ground glass") echoes on US.
- Dermoid cysts: Often show Rokitansky nodule (dermoid plug) & fat-fluid levels.
- HSG: Evaluates tubal patency & uterine cavity in infertility.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


