General Principles & CINV Intro - Chemo's Cruel Kickbacks
- Chemotherapy targets rapidly dividing cells: impacts cancer & normal tissues (bone marrow, GIT, hair follicles).
- Management Pillars:
- Prophylaxis: Anticipate & prevent predictable toxicities.
- Dose Modification: Adjust or delay based on severity of side effects.
- Supportive Care: Hydration, nutrition, growth factors (e.g., G-CSF for neutropenia, EPO for anemia).
- Symptom Management: Tailored to specific adverse events.
- CINV (Chemotherapy-Induced Nausea & Vomiting):
- Common, distressing; significantly impacts patient's quality of life.
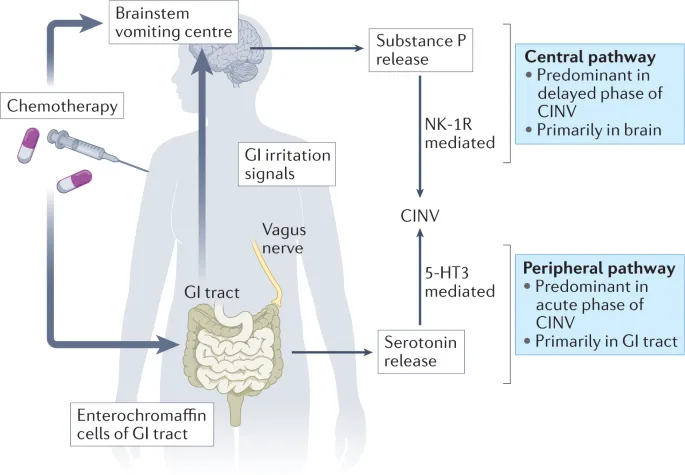
- Key Pathways: Central (chemoreceptor trigger zone - CTZ) & peripheral (gut vagal afferents).
- Neurotransmitters: Serotonin (5-HT₃), Substance P (NK₁).
- Types: Acute (<24h), Delayed (>24h), Anticipatory, Breakthrough, Refractory.
⭐ CTCAE (Common Terminology Criteria for Adverse Events) is widely used for grading toxicity and guiding management decisions across clinical trials and practice.
CINV Management - Vomit Veto
- Goal: Prevent CINV by targeting key neurotransmitters (Serotonin, Substance P, Dopamine).
- Risk Assessment: Crucial for regimen selection (High, Moderate, Low, Minimal emetogenic risk).
- CINV Phases:
- Acute: <24 hrs post-chemo.
- Delayed: >24 hrs post-chemo, up to 5 days.
- Anticipatory: Before chemo, conditioned response.
- Core Drug Classes:
- 5-HT3 Antagonists: (Ondansetron, Granisetron). Palonosetron (long-acting, good for delayed).
- NK1 Receptor Antagonists: (Aprepitant, Fosaprepitant). Key for HEC; target Substance P.
- Corticosteroids: (Dexamethasone). Synergistic, broad antiemetic.
- Olanzapine: Atypical antipsychotic; multi-receptor antagonist for breakthrough/refractory.
- Benzodiazepines: (Lorazepam). For anticipatory CINV.
⭐ NK1 receptor antagonists (e.g., aprepitant) are crucial for preventing delayed CINV with highly emetogenic chemotherapy.
Myelosuppression Mayhem - Blood Cell Blues
Bone marrow suppression by chemo → pancytopenia. Nadir: 7-14 days post-chemo.
-
Neutropenia (↓ Neutrophils): ANC < 1500/mm³ (Severe < 500/mm³).
- Manage: G-CSF (Filgrastim, Pegfilgrastim). 📌 Mnemonic: "Grandma Fil Needs Pegs for her Low Neutrophils."
- Prophylaxis: G-CSF if Febrile Neutropenia (FN) risk > 20%.
⭐ Febrile neutropenia (ANC < 500/mm³ + fever) is a medical emergency requiring prompt broad-spectrum antibiotics.
-
Anemia (↓ RBCs): Fatigue, pallor.
- Manage: ESAs (Epoetin, Darbepoetin; Target Hb 10-12 g/dL). Transfusion if Hb < 7-8 g/dL / symptomatic.
-
Thrombocytopenia (↓ Platelets): Platelets < 150,000/mm³ (Severe < 50,000/mm³).
- Spontaneous bleed risk < 10,000-20,000/mm³.
- Manage: Platelet transfusions. Oprelvekin (IL-11) - limited use.
Other Common Toxicities - Systemic Sucker Punches
- Cardiotoxicity:
- Anthracyclines (Doxorubicin): Cumulative; LVEF monitoring. Prevent: Dexrazoxane.
- Trastuzumab: Reversible LVEF dysfunction.
- Pulmonary Toxicity:
- Bleomycin: Pneumonitis/fibrosis (max 400 units).
- Busulfan: "Busulfan lung".
- Methotrexate: Acute pneumonitis.
- Nephrotoxicity:
- Cisplatin: ATN. Hydration, Amifostine. Monitor GFR.
- Methotrexate (high dose): Crystalluria. Alkalinize urine, Leucovorin, hydration.
- Neurotoxicity:
- Vincristine: Peripheral neuropathy (sensory, motor, autonomic).
- Cisplatin: Peripheral neuropathy, ototoxicity.
- Ifosfamide: Encephalopathy. Antidote: Methylene blue.
- Cytarabine (high dose): Cerebellar toxicity.
- Hemorrhagic Cystitis: (Cyclophosphamide, Ifosfamide - Acrolein)
- Prevention: Hydration, MESNA.
⭐ MESNA (Sodium 2-mercaptoethane sulfonate) is crucial for preventing hemorrhagic cystitis with cyclophosphamide/ifosfamide by neutralizing acrolein.
- Mucositis/Stomatitis: (5-FU, MTX, Doxorubicin)
- Management: Oral hygiene, cryotherapy, Palifermin.
- Hand-Foot Syndrome: (Capecitabine, 5-FU, Liposomal Doxorubicin)
- Management: Dose modification, cooling, emollients, Pyridoxine. oka
High‑Yield Points - ⚡ Biggest Takeaways
- Nausea/Vomiting: Key drugs: 5-HT3 antagonists (ondansetron), NK1 antagonists (aprepitant).
- Myelosuppression: Use G-CSF (neutropenia), EPO (anemia), Oprelvekin (thrombocytopenia).
- Hemorrhagic Cystitis (cyclophosphamide/ifosfamide): Prevent with Mesna and good hydration.
- Cardiotoxicity (doxorubicin): Dexrazoxane offers protection; monitor LVEF.
- Mucositis: Palifermin (KGF) promotes healing; good oral hygiene essential.
- Tumor Lysis Syndrome: Manage with hydration, allopurinol, or rasburicase.
- Diarrhea (irinotecan, 5-FU): Treat with loperamide; octreotide for severe cases.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

