Definition & Pathophysiology - Nerve Wreckage 101
- Definition (IASP): Pain caused by a lesion or disease of the somatosensory nervous system.
- Key Mechanisms:
- Peripheral Sensitization: ↑ responsiveness, ↓ threshold of nociceptive neurons in the periphery.
- Central Sensitization: ↑ excitability of neurons in the CNS (spinal cord, brain); involves wind-up, long-term potentiation.
- Ectopic Discharges: Spontaneous pathological firing from damaged primary afferent neurons or their axons.
- Channelopathy: Altered expression/function of ion channels (e.g., Na⁺, Ca²⁺ channels like Nav1.7, Nav1.8).
- Neuroinflammation: Activation of glia (microglia, astrocytes) releasing pro-inflammatory mediators.
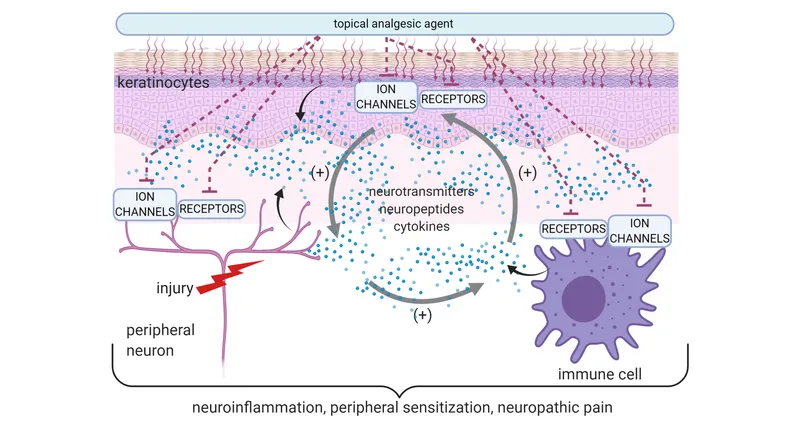
⭐ Allodynia (pain due to a stimulus that does not normally provoke pain) is a hallmark feature of neuropathic pain, often indicating central sensitization mechanisms at play_._
Clinical Features & Diagnosis - Pinpointing the Pain
- Key Symptoms: Burning, shooting, electric shocks, pins & needles, numbness. Often worse at night.
- Key Signs:
- Allodynia (pain from light touch).
- Hyperalgesia (↑ pain response).
- Sensory deficits (touch, vibration).
- Clinical Examination: Assess sensory modalities (light touch, pinprick, temperature, vibration), reflexes, and motor strength.
- Screening Tools:
Tool NP if Score DN4 ≥ 4 LANSS ≥ 12 PainDETECT ≥ 19 (likely NP)
⭐ Painful diabetic neuropathy is the most common type of neuropathic pain.
First-Line Pharmacotherapy - The Go-To Arsenal
| Feature | TCAs (e.g., Amitriptyline) | SNRIs (e.g., Duloxetine, Venlafaxine) | Gabapentinoids (e.g., Pregabalin, Gabapentin) |
|---|---|---|---|
| MOA | NE & 5-HT reuptake ↓; receptor blockade | NE & 5-HT reuptake ↓ | Bind $\alpha_2\delta$-1 Ca$^{2+}$ channel subunit |
| Starting Dose | Amitriptyline: 10-25 mg HS | Duloxetine: 30 mg OD; Venlafaxine XR: 37.5 mg OD | Pregabalin: 25-75 mg BID; Gabapentin: 100-300 mg HS/TID |
| Common SE | Anticholinergic, sedation, orthostasis | Nausea, dizziness, insomnia, ↑BP (Venlafaxine) | Dizziness, somnolence, edema, weight gain |
| Considerations | Cardiotoxicity risk (📌 Tri-C's); many interactions | Monitor BP (Venlafaxine); Duloxetine for DPNP | Renal dose adjustment needed |
Second & Third-Line Agents - Backup Brigade
-
Opioids (Use with caution):
- Tramadol: Weak µ-opioid agonist; serotonin-norepinephrine reuptake inhibitor (SNRI). Risks: Serotonin syndrome, ↓seizure threshold.
- Tapentadol: µ-opioid agonist & norepinephrine reuptake inhibitor (MOR-NRI). Fewer GI side effects than typical opioids.
-
Topical Agents:
Agent MOA Key Uses & Application Lidocaine 5% Patch Blocks Na+ channels, ↓ectopic firing Post-herpetic neuralgia (PHN). Max 3 patches; 12h on/12h off. Capsaicin Cream/Patch TRPV1 agonist, desensitizes C-fibers PHN, diabetic neuropathy. Apply with gloves. -
Other Anticonvulsants:
- Lamotrigine: Na+ channel blocker. Adjunct for refractory pain.
- Carbamazepine: Na+ channel blocker.
⭐ Carbamazepine is the drug of choice for trigeminal neuralgia.
Non-Pharma & Interventions - Holistic Help
- Non-Pharmacological:
- Physiotherapy: Enhances mobility, reduces pain.
- TENS (Transcutaneous Electrical Nerve Stimulation): For localized relief.
- CBT (Cognitive Behavioral Therapy): Modifies pain perception & coping.
- Acupuncture: Traditional method, may modulate pain.
- Interventional (refractory pain):
- Nerve blocks: Diagnostic or therapeutic (e.g., local anesthetics).
- Spinal Cord Stimulation (SCS): Neuromodulation for persistent pain.
- Intrathecal drug delivery: Targeted CNS analgesia (e.g., opioids).
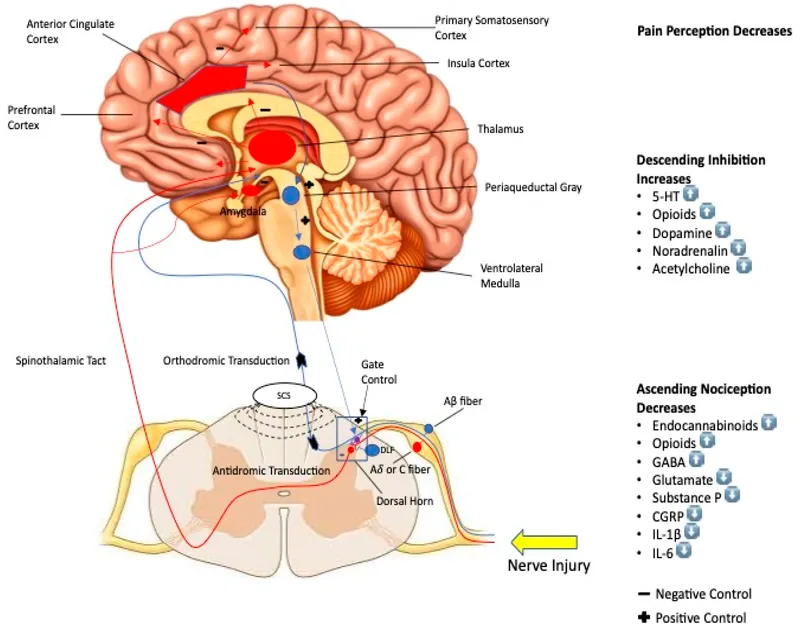
⭐ TENS is a commonly used non-invasive modality for localized neuropathic pain, often as an initial non-pharmacological approach.
High‑Yield Points - ⚡ Biggest Takeaways
- First-line: TCAs (Amitriptyline), SNRIs (Duloxetine), Gabapentinoids (Pregabalin, Gabapentin).
- Amitriptyline: Effective, but notable anticholinergic side effects, especially in elderly.
- Duloxetine: Good for painful diabetic neuropathy; also an antidepressant.
- Gabapentin/Pregabalin: Act on α2-δ Ca²⁺ channels; common side effects: sedation, dizziness.
- Carbamazepine: Drug of choice for trigeminal neuralgia.
- Tramadol/Tapentadol: Weak opioids with SNRI activity; second-line options.
- Topical Lidocaine: Useful for localized neuropathic pain.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

