ARM Intro - Embryo's Oopsie
- ARM: A spectrum of congenital defects involving an absent or abnormally located anus, and an improperly developed rectum.
- Embryo's Hiccup:
- Failure of the cloaca to correctly divide into urogenital sinus and anorectum.
- This crucial separation by the urorectal septum happens between weeks 5-7 of gestation.
- Associated Syndromes:
- VACTERL association is a significant co-occurrence.
- Look for spinal (tethered cord) and genitourinary malformations.
⭐ Incidence: Affects roughly 1 in 5000 live births.
oka
ARM Spectrum - Classifying the Chaos
ARMs present a spectrum of defects; precise classification is key for management and prognosis. The Krickenbeck classification is the standard.
⭐ The Krickenbeck classification is based on the fistula's location and is crucial for surgical planning.
Key Determinant: The presence and anatomical site of the fistula. "Low" lesions generally have better functional prognosis than "High" lesions.
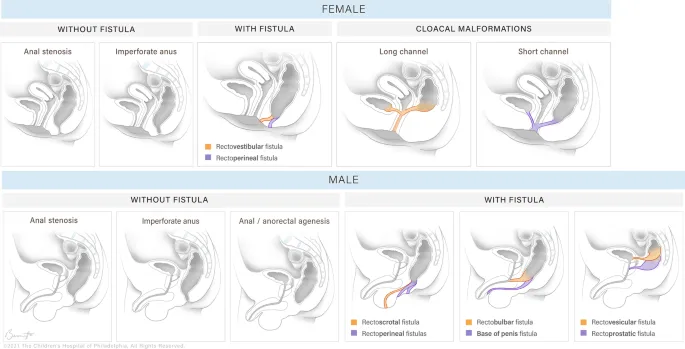
- Krickenbeck Categories:
- Males:
- Perineal Fistula (PF): Opening on perineal skin.
- Rectourethral Fistula (RUF): Connection to urethra.
- Bulbar (lower)
- Prostatic (higher)
- Rectovesical (Bladder Neck) Fistula: Connection to bladder; highest, most complex.
- ARM without Fistula
- Rectal Atresia/Stenosis
- Females:
- Perineal Fistula (PF): Opening on perineal skin.
- Vestibular Fistula: Opening in vulvar vestibule; most common in females.
- Cloaca: Single perineal opening for urinary, genital, and rectal tracts. Common channel length > 3 cm implies ↑ complexity.
- ARM without Fistula
- Rectal Atresia/Stenosis
- Rectovaginal Fistula (very rare)
- Males:
ARM Diagnosis - Uncovering Clues
- Clinical Presentation:
- Absent/ectopic anal opening (perineal, vestibular).
- Flat "bottom", single perineal dimple.
- Meconium from vagina, urethra, or perineum.
- Failure to pass meconium (24-48 hrs); abdominal distension.
- Key Investigations:
- Perineal Inspection: Essential initial step.
- Prone Cross-table Lateral X-ray: Done 18-24 hrs post-birth.
- Measures gas bubble to skin marker distance.
- High: > 1 cm; Low: < 1 cm.
- Perineal Ultrasound (USG): Accurate pouch-perineal distance, usable < 24 hrs.
- Distal Colostogram: Pre-definitive repair; defines pouch anatomy/fistula.
- VCUG: For suspected rectourinary fistula.
- MRI: Complex ARMs, cloaca, tethered cord.
- Screening for Associated Anomalies (📌 VACTERL):
- Vertebral: Spinal X-ray/USG.
- Cardiac: Echocardiogram.
- Tracheo-Esophageal: NG tube passage, CXR.
- Renal: Abdominal USG.
- Limb: Clinical exam, X-rays if needed.

⭐ Associated anomalies are common, with VACTERL association seen in up to 70% of cases.
ARM Management - Surgical Solutions
- Initial Management (High/Intermediate ARM):
- Stabilize patient.
- Diverting colostomy (sigmoid) within 24-48 hours if high/intermediate anomaly or no perineal fistula.
- Allows bowel decompression & growth.
- Definitive Repair:
- Posterior Sagittal Anorectoplasty (PSARP) is standard for most high/intermediate ARMs.
- Performed at 1-3 months (or ~5-10 kg).
- Laparoscopic-assisted PSARP (LASARP) for higher lesions.
- Low ARM Management:
- Primary perineal procedures (e.g., anoplasty, fistuloplasty) in neonatal period.
- Colostomy usually avoided for simple perineal fistulas.
⭐ Posterior Sagittal Anorectoplasty (PSARP) is the standard surgical approach for most intermediate and high ARMs.

High‑Yield Points - ⚡ Biggest Takeaways
- Anorectal Malformations (ARM) are a spectrum, from imperforate anus to complex cloaca.
- Strongly associated with VACTERL syndrome; look for other anomalies.
- Prone cross-table lateral X-ray or invertogram assesses pouch height and fistula.
- High lesions typically need initial colostomy, then PSARP (Posterior Sagittal Anorectoplasty).
- Low lesions may allow primary anoplasty or minimal PSARP.
- Fistula location (perineal, vestibular, urethral, vesical) is key for surgical planning.
- Post-op challenges include constipation and fecal incontinence requiring long-term follow-up.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

