Definition & Diagnosis - Pressure Points ID'd
- Definition: BP ≥ 95th percentile for age, sex, & height on ≥ 3 separate occasions.
- Classification (<13 yrs):
- Elevated: ≥ 90th to < 95th %ile
- Stage 1: ≥ 95th %ile to < (95th %ile + 12 mmHg)
- Stage 2: ≥ (95th %ile + 12 mmHg)
- Classification (≥13 yrs):
- Elevated: 120/<80 to 129/<80 mmHg
- Stage 1: 130/80 to 139/89 mmHg
- Stage 2: ≥ 140/90 mmHg
- Diagnostic Steps:
- Accurate auscultatory measurement (correct cuff).
- Ambulatory BP Monitoring (ABPM) to confirm.
⭐ Renal parenchymal disease is the most common cause of secondary HTN in children.

Etiology - Root Cause Roundup
- Primary (Essential) HTN:
- Increasingly common, especially in adolescents.
- Key associations: Obesity, positive family history, metabolic syndrome.
- Secondary HTN: More common in younger children; suspect if severe or <6 yrs.
- Renal (Most common, ~70-80%):
- Parenchymal Disease: Glomerulonephritis, reflux nephropathy, CAKUT, HUS, PKD.
- Renovascular Disease: Renal artery stenosis (e.g., FMD, NF1, Williams syndrome).
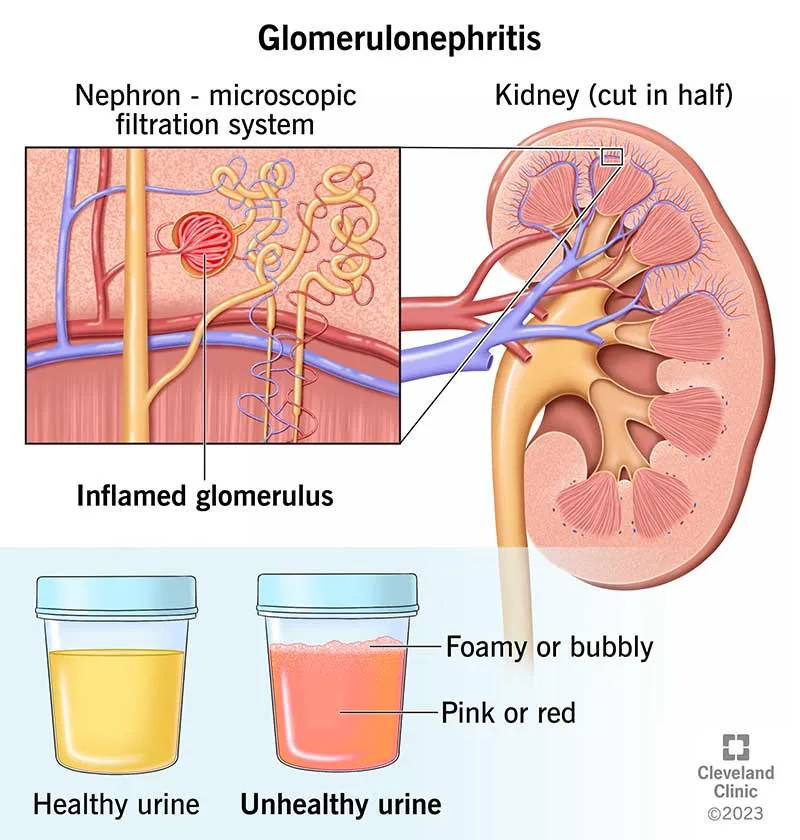
- Endocrine: Pheochromocytoma, neuroblastoma, CAH, hyperthyroidism, Cushing's.
- Cardiac: Coarctation of aorta (check femoral pulses!).
- Drugs: Corticosteroids, sympathomimetics, NSAIDs, OCPs.
- Genetic: Liddle, Gordon, AME.
- Renal (Most common, ~70-80%):
⭐ Renal parenchymal disease is the most common cause of secondary hypertension in children.
Clinical Clues & Consequences - Signs & System Stress
- Often asymptomatic. Symptoms (if present): headache, fatigue, visual changes, epistaxis.
- Severe HTN: seizures, VII nerve palsy, signs of heart failure, FTT (infants).
- Clues to etiology:
- Abdominal bruit (Renovascular HTN)
- Radio-femoral delay, BP discrepancy (Coarctation of Aorta)
- Target Organ Damage (TOD):
- CNS: Hypertensive encephalopathy, retinopathy (Keith-Wagener grades).
- CVS: Left Ventricular Hypertrophy (LVH), CHF.
- Renal: Proteinuria, progressive renal insufficiency.
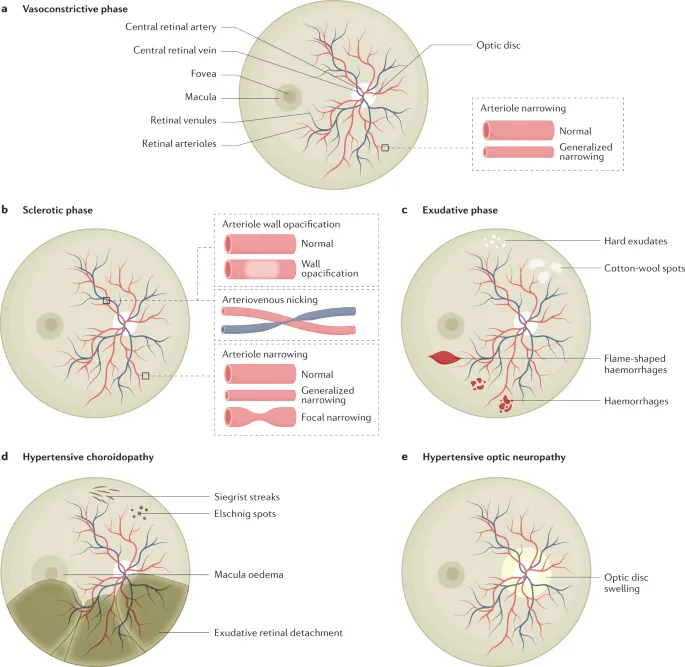
⭐ Left Ventricular Hypertrophy (LVH) is the most common early sign of target organ damage in children with chronic hypertension.
Workup & Management - The Takedown Plan
- Initial Workup:
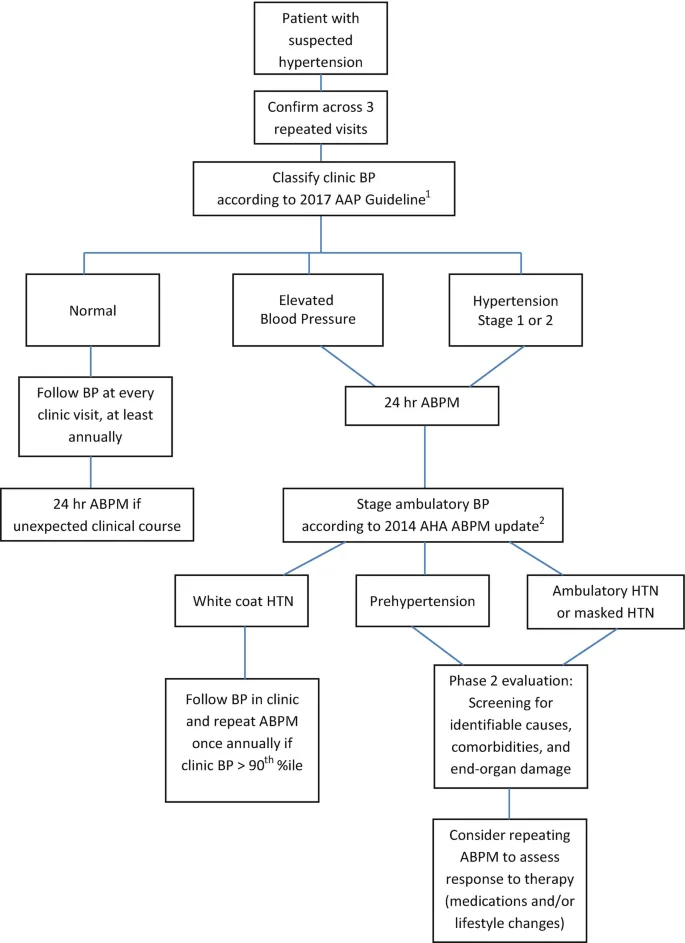
- Confirm BP: Multiple office visits or Ambulatory BP Monitoring (ABPM).
- Basic Labs: Urinalysis, RFT, electrolytes (K+), uric acid, fasting lipids.
- Renal Ultrasound with Doppler.
- Further tests (ECHO, endocrine studies) if secondary HTN suspected.
- Management Strategy:
- Non-pharmacological (cornerstone): Weight management, DASH diet (↓Na+, ↑K+), regular physical activity.
- Pharmacological: Indicated for symptomatic HTN, Stage **2** HTN, target organ damage (TOD), or failure of lifestyle changes.
- ACE inhibitors / ARBs (preferred in CKD, DM).
- Long-acting Calcium Channel Blockers (CCBs).
- Thiazide diuretics.
⭐ Ambulatory Blood Pressure Monitoring (ABPM) is the gold standard for diagnosing hypertension and assessing treatment efficacy in children.
Hypertensive Crisis - Emergency Pressure Drop
- Hypertensive Emergency: Severe HTN + acute end-organ damage (brain, heart, kidneys). Requires immediate, controlled BP ↓.
- Goal: ↓ Mean Arterial Pressure (MAP) or SBP/DBP by max 25% in first 8 hours.
- Then, gradual normalization over 24-48 hours.
- ⚠️ Avoid rapid/excessive BP fall → risk of hypoperfusion injury.
- IV Antihypertensives:
- Labetalol, Nicardipine
- Sodium Nitroprusside (SNP) (⚠️ toxicity)
- Hydralazine
- Flowchart:
- ⭐ > In children, hypertensive encephalopathy is the most common manifestation of hypertensive emergency.
High‑Yield Points - ⚡ Biggest Takeaways
- Renal parenchymal disease is the most common cause of secondary hypertension.
- Consider coarctation of aorta in infants with hypertension.
- Use appropriate cuff size (width 40%, length 80-100% arm circumference) for accurate BP.
- Hypertension: BP ≥95th percentile for age, sex, height on ≥3 occasions.
- Ambulatory BP Monitoring (ABPM) helps rule out white coat hypertension.
- Initial workup: Urinalysis, renal ultrasound, electrolytes, creatinine.
- Lifestyle modification is key; ACE inhibitors/ARBs for persistent/severe cases or proteinuria.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

