Endometrial Cycle & AUB - Phases & Bleed Clues
- Endometrial Cycle (Menstrual Cycle): Governed by ovarian hormones.
- Proliferative Phase (Follicular): Estrogen-driven (E₂).
- Endometrial glands & stroma proliferate; glands are straight, tubular.
- Secretory Phase (Luteal): Progesterone-driven (P₄) post-ovulation.
- Glands become tortuous ("saw-tooth"), coiled; subnuclear glycogen vacuoles appear, then luminal secretions. Spiral arteries lengthen & coil. Stromal edema, predecidual changes.
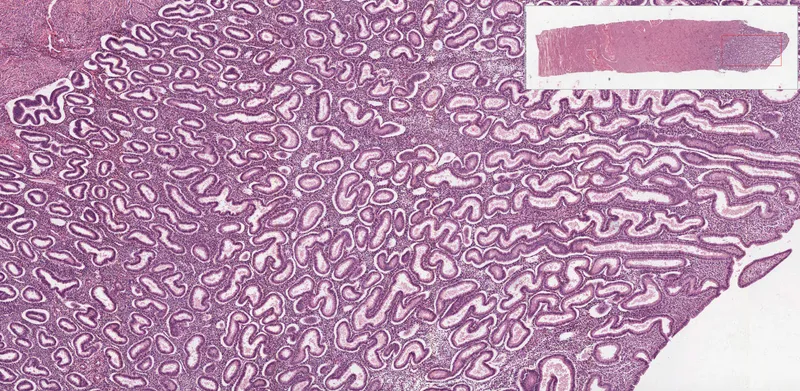
- Glands become tortuous ("saw-tooth"), coiled; subnuclear glycogen vacuoles appear, then luminal secretions. Spiral arteries lengthen & coil. Stromal edema, predecidual changes.
- Proliferative Phase (Follicular): Estrogen-driven (E₂).
- Abnormal Uterine Bleeding (AUB):
- 📌 PALM-COEIN classifies causes:
- Structural (PALM): Polyp, Adenomyosis, Leiomyoma, Malignancy/hyperplasia.
- Non-structural (COEIN): Coagulopathy, Ovulatory dysfunction, Endometrial, Iatrogenic, Not yet classified.
- Key endometrial AUB links: Polyps, hyperplasia/malignancy, ovulatory dysfunction (e.g., anovulation → unopposed estrogen).
- 📌 PALM-COEIN classifies causes:
⭐ In anovulatory cycles, persistent estrogen stimulation without progesterone opposition leads to continuous endometrial proliferation, resulting in fragile, unstable endometrium prone to irregular and often heavy bleeding (dysfunctional uterine bleeding).
Endometrial Hyperplasia - Overgrowth Alarms
- Definition: Abnormal proliferation of endometrial glands relative to the stroma, leading to an increased gland-to-stroma ratio.
- Risk Factors: Chronic unopposed estrogen exposure.
- Obesity (peripheral conversion of androgens).
- Polycystic Ovarian Syndrome (PCOS), anovulatory cycles.
- Exogenous estrogen therapy (without progestin).
- Tamoxifen (estrogenic effect on endometrium).
- WHO 2014 Classification & Progression Risk:
Category Key Feature Progression to Carcinoma Hyperplasia without Atypia Glandular crowding, no atypia Low risk (~1-3%) Atypical Hyperplasia / EIN Cytological atypia present High risk (~25-45%) - Molecular: PTEN tumor suppressor gene inactivation is a common early event in EIN.
- Clinical: Often presents as abnormal uterine bleeding (AUB).
⭐ Atypical hyperplasia/EIN is considered a direct precursor to endometrioid endometrial adenocarcinoma.
- Progression Pathway:
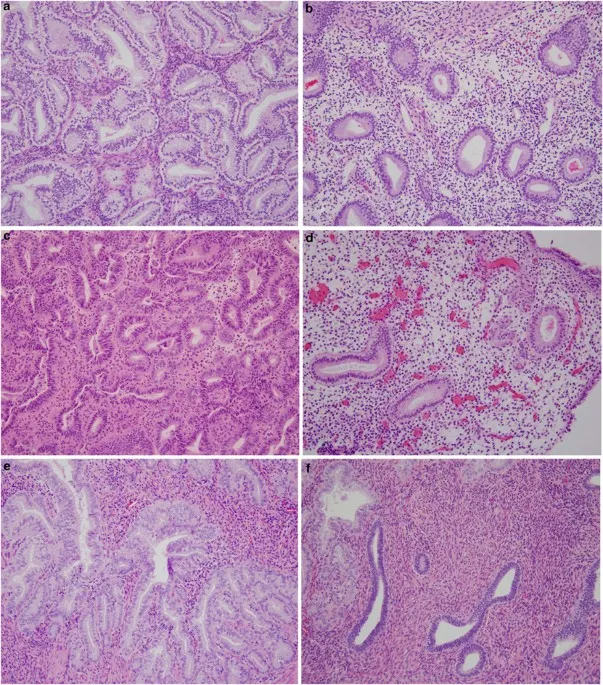
Endometrial Carcinoma - Cancerous Chaos
- Most common gynecologic malignancy in developed countries.
- Two main types:
| Feature | Type I (Endometrioid) | Type II (e.g., Serous) |
|---|---|---|
| Prevalence | ~80% | ~15-20% |
| Estrogen | Dependent (unopposed E2) | Independent |
| Precursor | Hyperplasia/EIN | Atrophy; Serous intraepithelial ca. (SEIC) |
| Age (Typical) | Perimenopausal | Postmenopausal (older) |
| Prognosis | Good | Poor |
| Mutations | PTEN, KRAS, ARID1A, PIK3CA, MSI | TP53 |
- FIGO Grading (Endometrioid): Based on % solid growth.
- Grade 1: ≤5% solid growth
- Grade 2: 6-50% solid growth
- Grade 3: >50% solid growth
- Lynch Syndrome (HNPCC):
- ↑ Risk of endometrioid type (MSI pathway).
⭐ TP53 mutations are characteristic of Type II (e.g., serous) endometrial carcinomas, associated with aggressive behavior and poor prognosis.
Benign & Inflammatory Issues - Polyps, Infections & Scars
- Endometrial Polyps
- Benign localized endometrial overgrowths; may cause Abnormal Uterine Bleeding (AUB).
- Histology: Thick-walled blood vessels, fibrous stroma.
- Associated with Tamoxifen.
- Endometritis (Inflammation of endometrium)
- Acute Endometritis
- Key: Neutrophilic infiltration of endometrial glands/stroma.
- Causes: Postpartum, post-miscarriage, Intrauterine Device (IUD).
- Chronic Endometritis
- Key: Plasma cells in endometrial stroma (diagnostic hallmark).
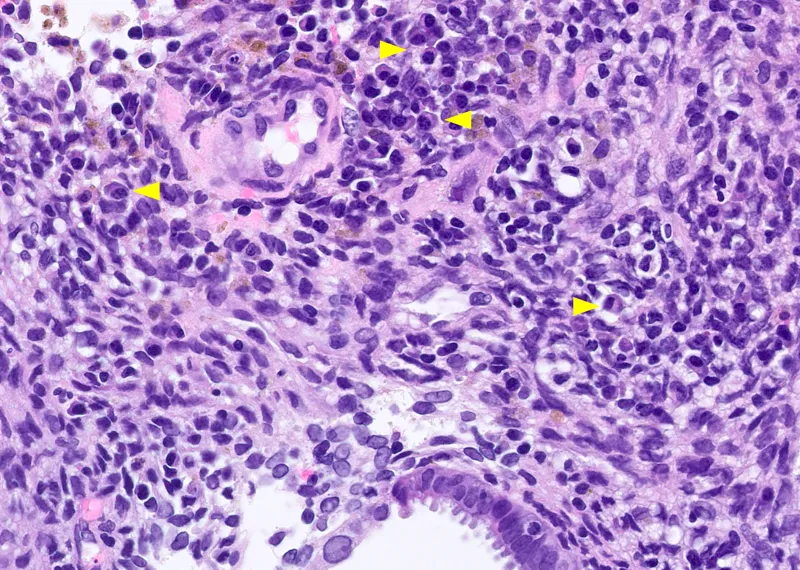
- Causes: Pelvic Inflammatory Disease (PID), Tuberculosis (TB), IUD, retained products of conception. 📌
- Tuberculous Endometritis (subtype): Caseating granulomas, acid-fast bacilli; common cause of infertility in India.
- Key: Plasma cells in endometrial stroma (diagnostic hallmark).
- Acute Endometritis
⭐ Plasma cells in endometrial stroma are the hallmark of chronic endometritis.
- Asherman Syndrome
- Intrauterine adhesions/synechiae (fibrous bands).
- Causes: Aggressive curettage (D&C), severe endometritis.
- Clinical: Amenorrhea/hypomenorrhea, infertility, recurrent pregnancy loss.
High‑Yield Points - ⚡ Biggest Takeaways
- Endometrial hyperplasia without atypia rarely progresses to cancer; atypia (EIN) is precancerous.
- Type I Endometrioid carcinoma: estrogen-driven, from hyperplasia, PTEN/KRAS mutations.
- Type II Serous carcinoma: aggressive, p53 mutation, in older women, atrophic endometrium.
- Asherman syndrome: intrauterine adhesions causing amenorrhea/infertility, post-curettage.
- Endometrial polyps: benign; can cause abnormal uterine bleeding (AUB).
- Adenomyosis: endometrial tissue in myometrium; causes dysmenorrhea, menorrhagia.
- Chronic endometritis: plasma cells in stroma; linked to PID, IUDs, TB.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

