Oral Microbiome Overview - Mouth's Tiny Tenants

- Definition: Diverse, dynamic microbial community (bacteria, fungi, viruses, archaea) inhabiting the oral cavity.
- Composition: Primarily bacteria; over 700 species identified. Dominant phyla: Firmicutes, Bacteroidetes, Proteobacteria, Actinobacteria, Fusobacteria.
- Biofilms: Microbes form structured communities (dental plaque) on teeth and mucosal surfaces.
- Eubiosis (Health): Contributes to homeostasis, initial digestion, pathogen defense.
- Dysbiosis (Disease): Imbalance leads to caries, periodontal diseases, and can influence systemic health.
⭐ Streptococcus mutans is a key cariogenic bacterium, producing acid from dietary sugars, leading to enamel demineralization.
Key Oral Microbes & Niches - Microbial Hotspots
- Supragingival Plaque (Enamel):
- Early (aerobic/facultative): S. sanguinis, S. gordonii, A. naeslundii.
- Caries: S. mutans (acidogenic/aciduric), Lactobacillus spp.
- Other: Veillonella spp. (lactate utilizer).
- Subgingival Plaque (Crevice/Pocket): Anaerobic.
- Key bridging species: Fusobacterium nucleatum.
- Periodontitis:
- Red Complex: P. gingivalis, T. forsythia, T. denticola (major periodontopathogens).
- Aggregatibacter actinomycetemcomitans (LAP, leukotoxin).
- Tongue Dorsum:
- VSC production (halitosis): Solobacterium moorei, Atopobium parvulum.
- Buccal Mucosa:
- Streptococcus salivarius (BLIS producer).
- Saliva:
- Transient microbes, host defense (sIgA, lysozyme).
- Fungi:
- Candida albicans (thrush, denture stomatitis).
- Viruses:
- HSV (latency), EBV (hairy leukoplakia), HPV (warts, cancer risk).
⭐ Streptococcus mutans, a key cariogen, uses sucrose for adherent glucans (biofilm) & lactic acid, causing enamel demineralization.
Dental Plaque & Biofilms - Sticky Situations
- Dental Plaque: Resilient, organized microbial biofilm. Bacteria in self-produced Extracellular Polysaccharide (EPS) matrix, adhering to tooth surfaces.
- Composition: Bacteria (Streptococci, Actinomyces), salivary glycoproteins, food debris, EPS (glucans, fructans for matrix).
- Key Bacteria & Roles:
- Early colonizers: S. sanguinis, S. mitis, A. naeslundii.
- Bridging: F. nucleatum.
- Caries: S. mutans (acid/EPS), Lactobacillus spp. (aciduric).
- Periodontal: Red complex (📌 PG Took Tooth: P. gingivalis, T. forsythia, T. denticola).
- Significance: Etiology of caries (demineralization), gingivitis, periodontitis (destruction), calculus formation.
⭐ S. mutans is a keystone pathogen in caries; it metabolizes sucrose using glucosyltransferases (GTFs) to produce sticky, insoluble glucans (EPS). These glucans are vital for strong bacterial adhesion, biofilm matrix integrity, and high cariogenic potential.
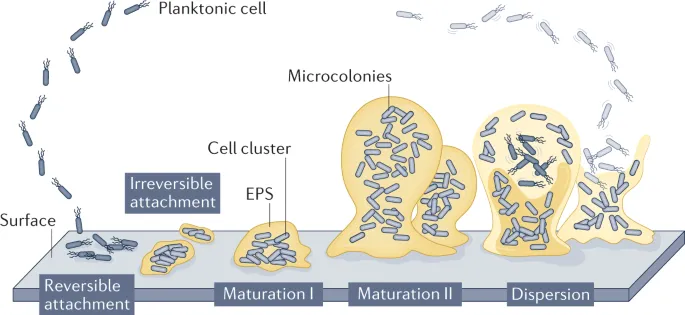
Oral Dysbiosis & Diseases - When Bugs Go Bad
Oral dysbiosis: Microbial imbalance (↑pathogens, ↓commensals) → disease.
- Dental Caries:
- Bugs: S. mutans (initiator, acidogenic/aciduric), Lactobacillus spp. (progression).
- Path: Sugars → Lactic acid → Enamel demineralization (pH <5.5).
- Periodontal Diseases:
- Shift: Predominantly Gram(+) aerobes/facultative → Gram(-) strict anaerobes.
- 📌 Red Complex: P.T.T. (P. gingivalis, T. forsythia, T. denticola).
- Gingivitis (reversible inflammation) → Periodontitis (irreversible bone loss).
- Oral Candidiasis:
- Candida albicans overgrowth.
- Risks: Immunosuppression, antibiotics, xerostomia, dentures.
- Halitosis:
- Anaerobes (e.g. P. gingivalis) → Volatile Sulfur Compounds (VSCs).
⭐ P. gingivalis is a keystone pathogen in chronic periodontitis, dysregulating host immunity even at low abundance.
Dysbiosis Triggers: High sugar diet, poor oral hygiene, smoking, systemic diseases (e.g., diabetes), xerostomic medications.

High‑Yield Points - ⚡ Biggest Takeaways
- Oral cavity: diverse microbial community, second most complex after gut.
- Streptococcus mutans: key cariogenic bacterium, produces acid from sugars, causing caries.
- Red complex (P. gingivalis, T. forsythia, T. denticola): strongly associated with periodontitis.
- Biofilm (dental plaque): essential for microbial colonization and oral disease pathogenesis.
- Saliva: crucial for oral homeostasis, providing nutrients, buffering, and antimicrobial factors.
- Oral dysbiosis: linked to dental caries, periodontal disease, and various systemic conditions.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

