Tumor Antigens & Surveillance - Spotting Rogues
- Tumor Antigens (TA): Molecules on tumor cells recognized by immune system.
- TSA (Tumor-Specific Antigens): Unique to tumors.
- Mutated proteins (p53, RAS).
- Viral antigens (HPV E6/E7).
- TAA (Tumor-Associated Antigens): On normal cells; overexpressed/aberrant on tumors.
- Oncofetal (AFP, CEA).
- Differentiation (CD20, PSA).
- Overexpressed (HER2/neu).
- TSA (Tumor-Specific Antigens): Unique to tumors.
- Immune Surveillance: Immune system recognizes & destroys nascent transformed cells.
- Key cells: NK cells, CD8+ CTLs.
- Cytokine: IFN-γ.
- Immunoediting: Elimination → Equilibrium → Escape.

⭐ Loss of MHC Class I expression is a key tumor escape mechanism, evading CD8+ T cell detection.
Anti-Tumor Immune Mechanisms - Cancer's Immune Cops
Innate Immunity:
- NK Cells: Recognize ↓MHC-I (missing-self). Kill via perforin/granzymes, TRAIL. ADCC via CD16.
- M1 Macrophages: Phagocytose. Secrete TNF-α, IL-1, IL-12, ROS, NO.
- Dendritic Cells (DCs): Key APCs. Cross-present tumor antigens to CD8+ T cells.
Adaptive Immunity:
- CTLs (CD8+): Primary effectors. Recognize tumor antigens on MHC-I. Kill via perforin/granzymes, Fas-FasL.
- Th1 Cells (CD4+): Secrete IFN-γ (activates M1, ↑MHC-I), TNF-α, IL-2. Enhance CTL/NK activity.
- B Cells/Antibodies: Produce tumor-specific Abs. Mediate ADCC, CDC.
⭐ IFN-γ, from Th1/NK cells, is key in tumor immunity: ↑Ag presentation, M1 activation, CTL differentiation.
Tumor Immune Evasion - Cancer's Sly Tricks
- Antigen Presentation Failure:
- ↓ MHC Class I expression (e.g., via TAP, β2-microglobulin defects).
- Antigen loss variants or masking.
- Immunosuppressive Microenvironment:
- Secretion of TGF-β, IL-10, PGE2.
- Recruitment/expansion of regulatory T cells (Tregs) & Myeloid-Derived Suppressor Cells (MDSCs).
- Immune Checkpoint Upregulation:
- ↑ PD-L1 expression on tumor cells binds PD-1 on T-cells → T-cell exhaustion.
- Expression of CTLA-4 ligands (B7 molecules) by APCs or tumor cells.
- Induction of T-cell Apoptosis:
- Tumor cells express FasL (CD95L) → binds Fas (CD95) on T-cells.
- Physical Barriers: Dense stroma can limit T-cell infiltration.
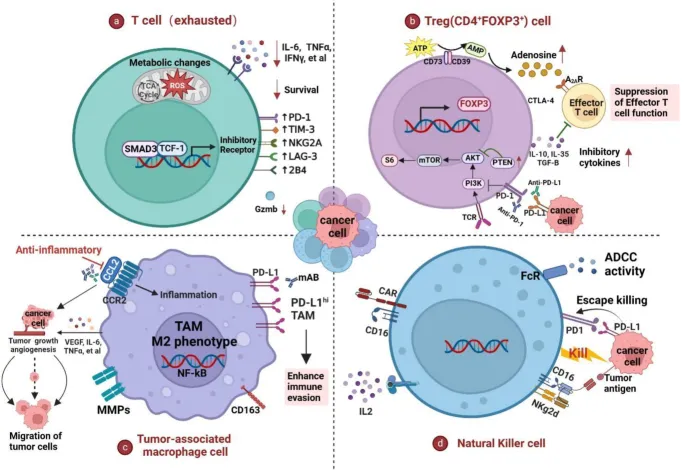
⭐ Many tumors exploit the PD-1/PD-L1 pathway to evade immune destruction; blocking this interaction with checkpoint inhibitors (e.g., Pembrolizumab, Nivolumab) can restore anti-tumor T-cell activity. This is a cornerstone of modern cancer immunotherapy. (NEET PG Favourite)
Cancer Immunotherapy - Immune System Unleashed
- Goal: Enhance host anti-tumor immunity.
- Strategies:
- Checkpoint Inhibitors (ICIs): Block T-cell "brakes" (CTLA-4, PD-1/PD-L1).
- Examples: Ipilimumab (anti-CTLA-4); Nivolumab, Pembrolizumab (anti-PD-1).
- Action: Restore T-cell killing. ⚠️ irAEs (colitis, pneumonitis).
- Adoptive Cell Therapy (ACT): Infuse modified/expanded immune cells.
- CAR T-cells: Engineered T-cells (anti-CD19 for B-cell ALL/lymphoma).
- TILs: Expanded Tumor-Infiltrating Lymphocytes.
- ⚠️ Cytokine Release Syndrome (CRS), ICANS.
- Cancer Vaccines: Prime tumor-specific immunity (Sipuleucel-T for prostate Ca).
- Oncolytic Viruses: Viruses lyse cancer cells (T-VEC for melanoma).
- Cytokine Therapy: IL-2 (RCC, melanoma), IFN-α.
- Checkpoint Inhibitors (ICIs): Block T-cell "brakes" (CTLA-4, PD-1/PD-L1).

⭐ Pembrolizumab (anti-PD-1) is approved for MSI-H/dMMR solid tumors, regardless of origin. 📌 PD-1 for MSI-H/dMMR Pan-tumor.
High‑Yield Points - ⚡ Biggest Takeaways
- TSAs are tumor-unique; TAAs are overexpressed self-antigens.
- Immunoediting involves Elimination, Equilibrium, and Escape phases of tumor-immune interaction.
- CTLs (CD8+ T cells) are key effectors, recognizing tumor antigens via MHC-I.
- NK cells mediate innate anti-tumor immunity, targeting cells with low MHC-I or stress signals.
- Tumor escape includes ↓MHC-I, immunosuppressive cytokines (TGF-β, IL-10), and PD-L1 expression.
- Checkpoint inhibitors (anti-PD-1, anti-CTLA-4) and CAR T-cell therapy are major immunotherapies.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

