DKA & HHS - Sugar Storms
DKA vs HHS Criteria:
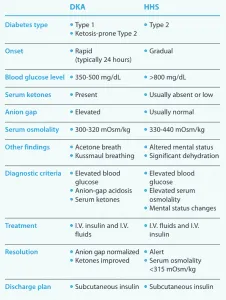
| Feature | DKA | HHS |
|---|---|---|
| Glucose (mg/dL) | > 250 | > 600 |
| Arterial pH | < 7.3 (Acidosis) | > 7.3 |
| HCO3 (mEq/L) | < 18 | > 18 |
| Ketones | ++/+++ | Minimal/Trace |
| Anion Gap | ↑ ($Na^+-(Cl^-+HCO_3^-)$) | Normal/Slight ↑ |
| Serum Osm (mOsm/kg) | Variable | > 320 ($2Na^++Gluc/18$) |
| Main Problem | Acidosis | Hyperosm, Dehydration |
- Fluids: Aggressive NS, then 0.45% NS. D5W at glucose ~200-250 (DKA) / 250-300 (HHS).
- Insulin: IV Regular 0.1 U/kg/hr (may bolus 0.1 U/kg).
- Potassium: Critical. If K+ <3.3 mEq/L, give K+ before insulin. Add K+ to IVF if K+ 3.3-5.2 mEq/L.
- Bicarb: Rarely, if pH <6.9 (DKA).
⭐ Euglycemic DKA (glucose <250mg/dL) with SGLT2i, pregnancy, starvation.
DKA/HHS Management Flow:
Hypoglycemia - Sugar Crash Crisis
- Definition: Whipple's Triad: 1. Symptoms of hypoglycemia. 2. Low plasma glucose (BG < 70 mg/dL; Severe: BG < 54 mg/dL). 3. Symptom relief with glucose.
- Causes:
- Diabetics: Insulin/sulfonylurea excess, ↓intake, ↑exercise, alcohol.
- Non-diabetics: Sepsis, liver/renal failure, insulinoma, adrenal insufficiency, illness.
- Clinical Features:
- Autonomic: Sweating, palpitations, tremor, anxiety, hunger.
- Neuroglycopenic: Confusion, weakness, dizziness, seizure, coma.
- Management: Rapid BG restoration. (📌 Rule of 15: 15g glucose, recheck 15 min).
⭐ Factitious hypoglycemia: Sulfonylurea use shows ↑ C-peptide; exogenous insulin use shows ↓ C-peptide.
Thyroid Turmoil - Storm & Coma
| Feature | Thyroid Storm | Myxedema Coma |
|---|---|---|
| Precipitating Factors | Infection, surgery, trauma, RAI, DKA, drug withdrawal. | Infection, CVA, CHF, sedatives, cold, non-compliance. |
| Key Clinical Features | Fever, tachycardia, agitation, GI upset. Burch-Wartofsky score > 45. | Hypothermia (<35.5°C), bradycardia, ↓LOC, hypoventilation. |
| Management | 📌 4 B's: Beta-blockers, Anti-thyroid drugs (PTU/MMI), Block release (Iodine), Block conversion/support (Steroids). Supportive. | IV Levothyroxine (300-500 mcg bolus), IV Hydrocortisone (100 mg q8h), supportive (warming, ventilation). |
Adrenal Alarm - Crisis & Catecholamines
- Adrenal Crisis: Life-threatening insufficiency.
- Causes: Addison's, steroid withdrawal, stress (infection, surgery).
- Features: Hypotension, shock, ↓Na, ↑K, ↓glucose, fever.
- Management: IV Hydrocortisone 100mg stat, then 50-100mg q6-8h or 200mg/24h infusion; IV fluids (NS, D5NS); IV glucose if needed.
- 📌 Mnemonic (5 S's): Salt (Saline), Sugar (Glucose), Steroids, Support, Search for cause.
- Pheochromocytoma Crisis: Catecholamine surge.
- Triggers: Surgery, trauma, certain drugs (e.g., unopposed β-blockers).
- Features: Paroxysmal HTN, headache, palpitations, sweating (classic triad).
- Management: Alpha-blockade (e.g., Phenoxybenzamine, Phentolamine IV for crisis) THEN Beta-blockade (e.g., Propranolol).
⭐ Always give alpha-blockers before beta-blockers in pheochromocytoma crisis to prevent unopposed alpha-adrenergic receptor stimulation, leading to paradoxical worsening of hypertension.
High‑Yield Points - ⚡ Biggest Takeaways
- DKA: Anion gap metabolic acidosis, Kussmaul breathing. Manage with IV fluids, insulin, and potassium monitoring.
- HHS: Extreme hyperglycemia (>600 mg/dL), severe dehydration, high osmolality, minimal ketones. Prioritize aggressive fluid resuscitation.
- Thyroid Storm: Fever, tachycardia, delirium. Treat with PTU/methimazole, beta-blockers, iodine, steroids.
- Myxedema Coma: Hypothermia, bradycardia, altered mental status. Administer IV levothyroxine and steroids.
- Adrenal Crisis: Hypotension, hyponatremia, hyperkalemia. Treat with IV hydrocortisone and fluids.
- Pheochromocytoma Crisis: Paroxysmal hypertension. Alpha-blockade before beta-blockade.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

