SDB Spectrum & Definitions - Snore Wars Saga
- SDB (Sleep-Disordered Breathing): Spectrum of disorders; abnormal respiration during sleep.
- Key Definitions:
- OSA (Obstructive Sleep Apnea): Recurrent upper airway collapse.
- CSA (Central Sleep Apnea): ↓/absent ventilatory effort.
- UARS (Upper Airway Resistance Syndrome): Airflow limitation; no frank apnea/hypopnea.
- OHS (Obesity Hypoventilation Syndrome): Obesity + daytime hypercapnia.

⭐ Apnea-Hypopnea Index (AHI) is the total number of apneas and hypopneas per hour of sleep.
Pathophysiology of OSA - The Choking Point
- OSA: Recurrent upper airway collapse (partial/complete) during sleep → apnea/hypopnea, intermittent hypoxia, hypercapnia, sleep fragmentation.
- Key Factors:
- Anatomical narrowing: e.g., retrognathia, tonsillar hypertrophy, obesity (fat deposition).
- Neuromuscular: ↓ pharyngeal dilator muscle activity (e.g., genioglossus) during sleep.
- Inspiratory negative pressure overcomes airway stability.
- CSA (contrast): Impaired central ventilatory effort, not obstruction.
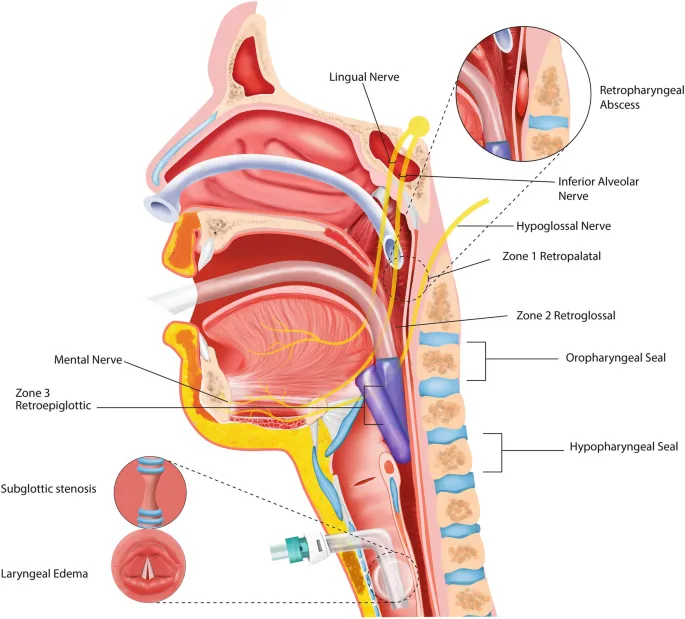
⭐ The velopharynx (soft palate area) and oropharynx (tongue base area) are the most common sites of airway collapse in OSA.
Clinical Clues & Risks - The Sleepiness Scale
- Symptoms: Loud snoring, witnessed apneas, EDS, morning headaches, nocturnal choking/gasping.
- Signs: Obesity (BMI >30), ↑Neck circ. (>43cm M, >40cm F), Mallampati III/IV, retrognathia.
- Key Risks: Male, Age >50, family Hx, alcohol/sedatives, craniofacial anomalies.
- Screening:
- ESS (Epworth Sleepiness Scale): Assesses EDS. Score >10 = significant sleepiness.
- STOP-BANG: (Snoring, Tired, Observed apnea, Pressure, BMI >35, Age >50, Neck, Gender).
⭐ STOP-BANG score ≥3 indicates high risk of OSA; Neck circumference >43cm (M) or >40cm (F) is a key risk factor.
Diagnostic Deep Dive - Decoding Sleep Tests
- Polysomnography (PSG): Gold standard (Type I). Comprehensive in-lab evaluation.
- Monitors multiple channels: EEG, EOG, EMG, ECG, airflow, respiratory effort, SaO2.
- Key Metrics: AHI, RDI, ODI, SaO2 nadir (lowest O2 saturation).
- Home Sleep Apnea Test (HSAT): Portable (Type III/IV) for suspected moderate-severe uncomplicated OSA.
⭐ Polysomnography (PSG) is gold standard. OSA AHI severity: Mild 5-14.9, Moderate 15-29.9, Severe ≥30 events/hr.
Treatment Blueprints - Breathing Easy Again
- Conservative:
- Weight loss (target BMI < 25).
- Positional therapy (non-supine).
- Avoid alcohol/sedatives pre-sleep.
- Medical Therapy:
- CPAP: First-line for moderate (AHI 15-30) to severe (AHI >30) OSA.
- Oral Appliances (MADs): For mild-moderate OSA or CPAP intolerance.
- Surgical Options (if CPAP fails/intolerated or specific anatomy):
- UPPP (Uvulopalatopharyngoplasty).
- MMA (Maxillomandibular Advancement) - highly effective.
- T&A (Adenotonsillectomy) - primary for pediatric OSA.
⭐ CPAP is first-line for moderate-severe OSA; surgical options considered for CPAP failure/intolerance or specific anatomical issues.
High‑Yield Points - ⚡ Biggest Takeaways
- OSA involves recurrent upper airway collapse during sleep, causing hypoxia and fragmented sleep.
- Polysomnography (PSG) is gold standard for diagnosis; severity based on Apnea-Hypopnea Index (AHI).
- AHI: Mild 5-15, Moderate 15-30, Severe >30 events/hour.
- Major risk factors: obesity (BMI >30), male gender, adenotonsillar hypertrophy (children).
- CPAP is first-line for moderate-severe adult OSA; adenotonsillectomy for most children.
- Excessive Daytime Somnolence (EDS) is a key symptom of OSA and significantly impacts quality of life.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


