Laryngomalacia - Floppy Larynx Intro
- Definition: Congenital flaccidity of laryngeal tissues, leading to inward collapse during inspiration.
- Also known as "floppy larynx".
- Most common congenital laryngeal anomaly (60-75% of cases).
- Results in intermittent, partial airway obstruction.

⭐ Laryngomalacia is the most common cause of stridor in infants and newborns.
- Typically presents in the first few weeks of life.
- Stridor is usually inspiratory, worse when supine, agitated, or feeding.
Pathophysiology - Why So Wobbly?
-
Immature, floppy laryngeal cartilages (epiglottis, arytenoids) leading to ↑ collapsibility.
-
Redundant supraglottic soft tissues (e.g., aryepiglottic folds, arytenoid mucosa).
-
Possible neuromuscular incoordination or hypotonia affecting laryngeal support.
-
During inspiration, negative intrathoracic pressure causes these lax supraglottic structures to prolapse inward, obstructing the airway.
-
This dynamic collapse leads to turbulent airflow and characteristic inspiratory stridor.
-
Common patterns of collapse:
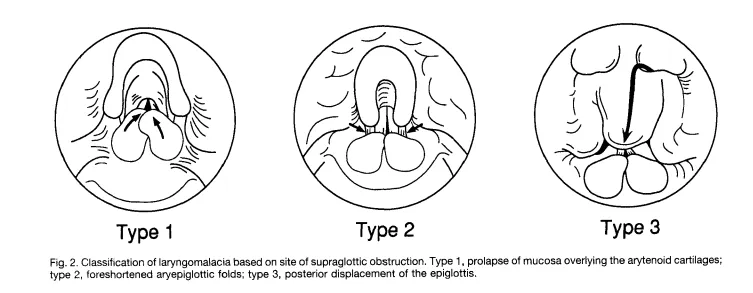
- Type 1: Inward collapse of arytenoid cartilages and redundant mucosa (most common).
- Type 2: Shortened aryepiglottic folds pulling epiglottis posteroinferiorly.
- Type 3: Posterior and/or lateral collapse of an elongated, omega-shaped epiglottis.
⭐ Laryngomalacia is the most common congenital laryngeal anomaly and cause of stridor in infants; symptoms typically worsen with agitation, feeding, or supine positioning due to increased inspiratory effort and gravitational effects on floppy tissues.
Clinical Signs - Noisy Breather Baby
- Onset: Typically within first 2 weeks of life, often by 4-6 weeks.
- Stridor:
- Predominantly inspiratory, high-pitched, fluttering.
- Intermittent; worsens with supine position, agitation, feeding, URIs.
- Improves with prone position or neck extension.
- Voice & Cry: Usually normal.
- Feeding: Generally unaffected; severe cases may show poor weight gain, choking.
- Course: Symptoms peak around ~6 months, typically resolve by 18-24 months.
⭐ Stridor in laryngomalacia is classically inspiratory and characteristically worsens in the supine position and with agitation.
Diagnosis - Scope The Larynx
- Gold Standard: Flexible Fiberoptic Laryngoscopy (FFL).
- Performed on an awake, spontaneously breathing child.
- Allows direct visualization of dynamic laryngeal collapse during inspiration.
- Key Findings (Inspiratory Supraglottic Collapse):
- Type 1: Inward collapse of arytenoid cartilages/redundant mucosa.
- Type 2: Medial collapse of short aryepiglottic folds.
- Type 3: Posterior and inferior collapse of an omega-shaped (Ω) epiglottis.
⭐ Laryngomalacia is the most common congenital laryngeal anomaly and the primary cause of stridor in infants.
Management - Fixing The Flop
- Conservative (Most cases: 90%):
- Observation, reassurance.
- Positioning: Prone or upright after feeds.
- Feeding modification: Small, frequent, thickened feeds.
- Medical:
- Anti-reflux (PPIs, H2 blockers) if GERD suspected.
- Surgical (Severe cases: 10-20%): Aryepiglottoplasty / Supraglottoplasty.
- Indications: Failure to thrive (FTT), severe dyspnea, cyanosis, apneas, cor pulmonale, feeding difficulties.
⭐ Supraglottoplasty is the gold standard surgical treatment for severe laryngomalacia, involving trimming of redundant aryepiglottic folds or arytenoid mucosa.
High‑Yield Points - ⚡ Biggest Takeaways
- Laryngomalacia: most common congenital laryngeal anomaly and cause of stridor in infants.
- Inspiratory stridor is characteristic, worsening with crying, feeding, supine position; improves when prone.
- Diagnosis via flexible fiberoptic laryngoscopy (FFL), showing an omega-shaped epiglottis or arytenoid prolapse.
- Typically benign and self-resolves by 18-24 months.
- Management: Observation for mild cases; supraglottoplasty for severe symptoms like failure to thrive (FTT) or apnea.
- Frequently associated with Gastroesophageal Reflux Disease (GERD).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

