Photoreactions: Basics - Sun's Double Trouble
- Phototoxicity
- Non-immunologic; direct cell damage by UV-activated agent.
- Dose-dependent (agent & UV). Rapid onset (min-hrs).
- Resembles exaggerated sunburn.
- Agents: Tetracyclines, Amiodarone, Psoralens.
- Photoallergy
- Immunologic (Type IV); UV forms allergen from agent.
- Requires prior sensitization. Delayed onset (24-72 hrs).
- Eczematous, itchy; may spread beyond exposed areas.
- Agents: Topical NSAIDs, sunscreens, fragrances.
⭐ Phototoxic reactions are non-immunological and dose-dependent, while photoallergic reactions are immunological (Type IV hypersensitivity) and require prior sensitization.
Phototoxicity Details - Rapid Rash Reaction
- Mechanism: Non-immunologic; light (esp. UVA) activates a chemical, causing direct cellular damage.
- No prior sensitization required.
- Onset: Rapid, within minutes to hours of sun exposure.
- Clinical Features: Resembles exaggerated sunburn.
- Erythema, edema, pain, burning.
- Vesicles or bullae in severe cases.
- Strictly confined to sun-exposed skin.
- Dose-Related: Severity depends on drug/chemical dose and light intensity.
- Outcome: Heals with hyperpigmentation; no immunologic memory or cross-reactions.
⭐ Common phototoxic drugs include tetracyclines (especially doxycycline), NSAIDs, amiodarone, and psoralens (PUVA therapy). Phytophotodermatitis (e.g., from lime juice containing furocoumarins) is a classic example.

Photoallergy Details - Itchy Delayed Reaction
- Mechanism: Type IV (delayed) hypersensitivity. UV radiation (UVA > UVB) transforms a chemical (hapten) into an allergen. Requires prior sensitization.
- Onset: Delayed, 24-72 hours post sun exposure.
- Clinical Features:
- Intensely itchy (pruritic) eczematous eruption.
- Lesions: Papules, vesicles, scaling; may lichenify chronically.
- Distribution: Sun-exposed areas, may spread to non-exposed sites.
- Morphology: Resembles allergic contact dermatitis.
- Common Photoallergens:
- Sunscreens: PABA derivatives, oxybenzone, cinnamates.
- Fragrances: Musk ambrette, sandalwood oil.
- Topical NSAIDs: Ketoprofen, piroxicam.
- Antimicrobials: Sulfonamides, FQs.
- 📌 Mnemonic: "Some Fine New Agents" (Sunscreens, Fragrances, NSAIDs, Antimicrobials)
- Diagnosis: Photopatch testing (gold standard).
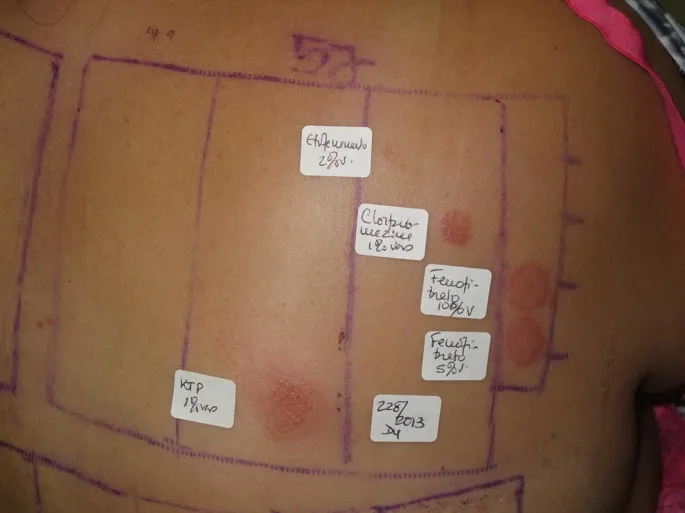
- Management: Identify & avoid allergen; topical/systemic corticosteroids.
⭐ Photopatch testing is the gold standard for diagnosing photoallergy, identifying the specific photoallergen. Common photoallergens include fragrances, sunscreens (e.g., PABA derivatives, oxybenzone), and topical NSAIDs.
Phototoxicity vs. Photoallergy - Twin Teardown Table
| Feature | Phototoxicity | Photoallergy |
|---|---|---|
| Mechanism | Direct cellular damage (Non-immune) | Immune-mediated (Type IV Hypersensitivity) |
| Incidence | High (any individual if dose sufficient) | Low (requires prior sensitization) |
| Onset | Minutes to hours | 24-72 hours (Delayed) |
| Clinical | Exaggerated sunburn (pain, edema, bullae) | Eczematous (pruritus, papules, vesicles) |
| Distribution | Sun-exposed areas, sharply demarcated | May spread beyond exposed areas; ill-defined |
| Histology | Epidermal necrosis, dermal edema | Spongiosis, acanthosis, lymphocytic infiltrate |
| Key Agents | Doxycycline, Amiodarone, NSAIDs, Psoralens | Sulfonamides, Fragrances, Sunscreens (PABA), Ketoprofen |
High‑Yield Points - ⚡ Biggest Takeaways
- Phototoxicity: Non-immunologic, rapid onset (minutes-hours), like exaggerated sunburn, often painful.
- Photoallergy: Type IV hypersensitivity (immune), delayed onset (24-72h), eczematous, itchy rash.
- Phototoxicity is dose-dependent (drug & UV) and affects anyone; no prior sensitization needed.
- Photoallergy requires prior sensitization; rash can spread beyond sun-exposed areas.
- Key phototoxic drugs: Doxycycline, Amiodarone, Psoralens, Thiazides, Piroxicam.
- Key photoallergic agents: Topical Ketoprofen, sunscreens (PABA), fragrances, Phenothiazines.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

