Aspiration Syndromes - Gut Gone Wrong
- Aspiration of gastric contents → pulmonary injury. Types:
- Chemical pneumonitis (Mendelson's): Gastric acid ($pH < \textbf{2.5}$, volume $ > \textbf{0.4} \text{ ml/kg}$ or $ > \textbf{25} \text{ ml}$). Rapid onset (1-2 hrs).
- Bacterial pneumonia: Infected aspirate. Slower onset (24-48 hrs).
- Particulate aspiration: Airway obstruction.
- Risk Factors: Full stomach, emergency surgery, GERD, obesity, pregnancy, ↓LOC, difficult airway.
- Prevention: Fasting (solids 6-8h, clears 2h), RSI, cricoid pressure, prokinetics, antacids, H2 blockers, PPIs.
- Management: Airway suction, O₂, PEEP, bronchodilators. Antibiotics for pneumonia, not routine for pneumonitis.
⭐ Mendelson's: chemical pneumonitis from gastric aspirate (pH < 2.5, volume > 0.4 ml/kg or > 25 ml).
Airway Obstruction - Choke Hold Horrors
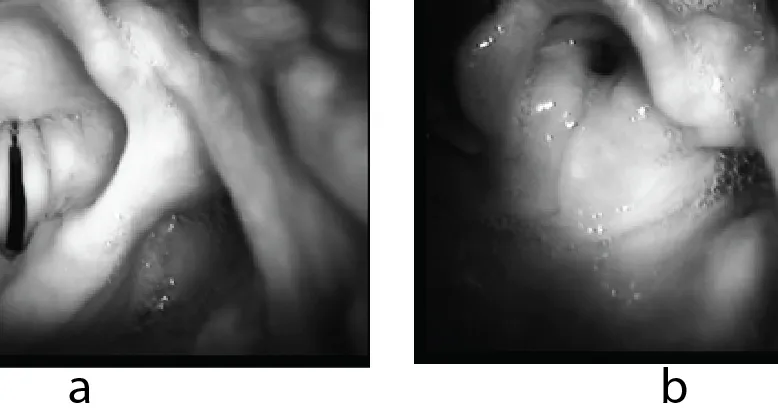
- Laryngospasm: Reflex glottic closure.
- Causes: Irritation (secretions, blood), light anesthesia, pain.
- Signs: Stridor, "rocking horse" breathing, ↓SpO₂.
- 📌 Mnemonic: Larson's maneuver, Oxygen (100%), Suction, Suxamethonium.
- Mgmt: 100% O₂, PPV, Larson's maneuver, deepen anesthesia (Propofol 10-30mg), Succinylcholine 0.1-1 mg/kg IV or 4-5 mg/kg IM.
- Bronchospasm: Lower airway smooth muscle contraction.
- Causes: Asthma, COPD, allergy, aspiration, drugs.
- Signs: Wheeze, ↓SpO₂, ↑Peak Airway Pressure, ↑EtCO₂ (early) then ↓.
- Mgmt: 100% O₂, deepen anesthesia (volatiles, ketamine), β₂-agonists (Salbutamol), IV Hydrocortisone 100-200 mg. Consider Aminophylline, MgSO₄.
⭐ Laryngospasm is most common in children during Stage 2 anesthesia or with airway irritation.
Lung Collapse & Fluid - Soggy Sponges
- Atelectasis (Collapse): Alveolar collapse, ↓ lung volume.
- Types: Resorption (post-op mucus plug), compression, adhesive (↓surfactant).
- Risks: Anesthesia (↓FRC), surgery, immobility.
- Signs: ↓Breath sounds, dull percussion, hypoxemia.
- Prevention/Tx: Incentive spirometry, PEEP, mobilization. 📌 SIGH - Spirometry, Inspiration (deep), Get moving, Hydration.
- Pulmonary Edema (Fluid): Excess fluid in alveoli/interstitium.
- Cardiogenic: ↑Hydrostatic pressure (LV failure, fluid overload).
- Non-cardiogenic: ↑Permeability (ARDS, sepsis, TRALI).
- Negative Pressure Pulmonary Edema (NPPE): Forceful inspiration against obstructed airway.
- Signs: Dyspnea, crackles, pink frothy sputum.
- Tx: O2, PEEP, diuretics (cardiogenic), address cause.

⭐ Negative Pressure Pulmonary Edema (NPPE) can occur within minutes to hours after relief of acute upper airway obstruction_
Barotrauma & Hypoxia - Pressure Problems
- Barotrauma: Lung injury from excessive positive pressure during mechanical ventilation.
- Manifestations: Pneumothorax, pneumomediastinum, subcutaneous emphysema, pneumoperitoneum.
- Risk factors: High Peak Inspiratory Pressure (PIP), Plateau Pressure (Pplat) > 30 cm H₂O, large tidal volumes ($V_T$).
- Prevention: Lung Protective Ventilation (LPV): $V_T$ 4-8 ml/kg Ideal Body Weight (IBW), Pplat < 30 cm H₂O.
- Hypoxia: Arterial $O_2$ saturation ($SpO_2$) < 90% or $PaO_2$ < 60 mmHg.
- Key Causes: 📌 Hypoventilation, V/Q mismatch (e.g., atelectasis, PE), Shunt, Low $FiO_2$, Diffusion limitation.
- Management: ↑ $FiO_2$, ensure patent airway, optimize ventilation (PEEP), treat specific cause.
⭐ Plateau pressure (Pplat), reflecting alveolar pressure, is a more critical determinant of barotrauma than PIP. Keep Pplat < 30 cm H₂O.

High‑Yield Points - ⚡ Biggest Takeaways
- Aspiration pneumonitis: high risk with full stomach, GERD. Mendelson's syndrome: pH < 2.5, volume > 0.4 mL/kg.
- Atelectasis: most common post-op pulmonary complication, often from hypoventilation.
- Bronchospasm: triggered by airway irritation, drugs, or reactive airway disease.
- Negative Pressure Pulmonary Edema (NPPE): follows laryngospasm or upper airway obstruction.
- Pneumothorax: risk with central line insertion, supraclavicular block, barotrauma.
- Post-op hypoxemia: common causes include atelectasis, diffusion hypoxia (N2O).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

