EEA Basics - Scope & Skyways
- Definition: Minimally invasive surgery using endoscopes via nasal corridors for skull base/intracranial lesions, avoiding external incisions.
- Goals: Maximize resection, minimize morbidity, preserve neurological function.
- Advantages (vs. Open): ↓ Blood loss, ↓ hospital stay, no external scars, superior magnified visualization, direct access.
- Indications:
- Pituitary tumors (adenomas).
- CSF leak repairs (sphenoid, ethmoid).
- Select sinonasal malignancies (esthesioneuroblastoma).
- Anterior skull base lesions (meningiomas, craniopharyngiomas, chordomas).
- Contraindications:
- Extensive lateral extension beyond Internal Carotid Artery (ICA).
- Significant vascular encasement by tumors.
- Inadequate team expertise/instrumentation.
-
⭐ The "two-nostril, four-hands" technique is pivotal in complex EEA, allowing two surgeons bimanual operation, enhancing dissection, hemostasis, and removal.
Anatomic Avenues - Skull Base Highways
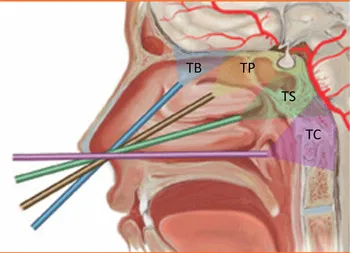
Endoscopic skull base surgery uses sinonasal corridors as highways to deep targets, demanding precise anatomical navigation.
| Corridor | Target Area (Pathology) | Key Landmarks | Structures at Risk |
|---|---|---|---|
| Transsphenoidal | Sella, parasellar (Pituitary Ad.) | Sphenoid ostia, sella, tuberculum sellae, OCR, cavernous sinus | Optic N., ICA, pituitary, CN III-VI |
| Transcribriform | Ant. cranial fossa (Esthesioneuro.) | Cribriform plate, A/P ethmoidal arteries, olfactory groove, crista galli | Olfactory Ns., dura, frontal lobes, CSF leak |
| Transclival | Post. cranial fossa (Chordoma) | Clivus (upper/mid/lower), paraclival ICA, Dorello's canal, foramen magnum | Basilar/vertebral arteries, CN VI, IX-XII, brainstem |
⭐ The Opticocarotid Recess (OCR) is a paramount landmark in transsphenoidal surgery; its lateral wall is formed by the prominence of the optic nerve and carotid artery, dictating safe dissection limits.
Max-Level Modules - Expert Extensions
- Transpterygoid Approach:
- Accesses infratemporal fossa (ITF), Meckel's cave, lateral sphenoid, petrous apex.
- Indications: Juvenile Nasopharyngeal Angiofibroma (JNA) with ITF extension, trigeminal schwannomas, selected skull base tumors.
- Transorbital Approach:
- Corridor to orbital apex, superior orbital fissure, medial cavernous sinus.
- Indications: Orbital apex tumors (e.g., optic nerve sheath meningioma), fungal granulomas, selected vascular lesions.
- Endoscopic Denker's (Anterior Maxillectomy):
- Wide access to anteroinferior maxillary sinus, pterygopalatine fossa (PPF), nasopharynx.
- Indications: Inverted papilloma, sinonasal malignancies involving anterior/inferior maxilla.
- Modified Endoscopic Lothrop (MELP) / Draf III:
- Creates a common median frontal sinus drainage pathway.
- Indications: Refractory chronic frontal sinusitis, extensive polyposis, frontal sinus mucoceles/tumors.
⭐ The Draf III procedure involves removing the inter-frontal sinus septum, the superior nasal septum, and the frontal sinus floor bilaterally.
Tools, Troubles & Triumphs
- Tools & Tech:
- Endoscopes (0°, 30°, 45°, 70°), specialized long instruments, high-speed drills.
- Neuronavigation (IGS) for precision, intra-op imaging (CT/MRI).
- Troubles & Fixes:
- CSF Leak: Most common serious. Manage: meticulous multilayered closure (e.g., fascia lata, fat, nasoseptal flap). 📌 "FFF" - Fascia, Fat, Flap for repair layers.
- Vascular Injury: Internal Carotid Artery (ICA) - critical risk! Requires immediate control.
- Nerve Palsies: Cranial Nerves II, III, IV, V, VI; often transient.
- Others: Meningitis (prophylactic antibiotics), sinusitis, anosmia, mucocele.
⭐ The nasoseptal flap (Hadad-Bassagasteguy flap) is the versatile workhorse for skull base reconstruction in EEA, significantly reducing CSF leak rates (reported <5% with its use).
- Triumphs (Post-Op Care):
- Nasal packing/stents, systemic antibiotics, steroids (tapered).
- Regular debridement crucial. Lumbar drain (selective for high-risk/confirmed leaks).
High‑Yield Points - ⚡ Biggest Takeaways
- Extended endoscopic approaches offer minimally invasive access to complex skull base lesions.
- Transsphenoidal approach targets pituitary tumors; transcribriform for anterior skull base.
- The Nasoseptal flap (Hadad-Bassagasteguy flap) is crucial for reconstruction and preventing CSF leaks.
- Image-guided navigation and neurosurgical collaboration are essential for safety and success.
- Key complications include CSF rhinorrhea, carotid artery injury, and cranial nerve deficits.
- Transpterygoid approach provides access to pterygopalatine and infratemporal fossae.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

