Laryngeal Imaging Intro - Vocal Cord Views
- Indications for Advanced Laryngeal Imaging (Stroboscopy, HSDI):
- Persistent dysphonia (e.g., >3 weeks)
- Suspected vocal fold pathology (nodules, polyps, cysts, paralysis)
- Pre- and post-phonosurgery evaluation
- Assessment of professional voice users
- Basic Principles:
- Light Source: Stroboscopic (flashing light, e.g., xenon) or continuous high-intensity light (for high-speed digital imaging - HSDI).
- Recording: Digital camera captures images of vocal fold vibration.
- Imaging Access - Endoscopy Types:
- Rigid (Transoral): Offers superior image magnification and clarity; may elicit gag reflex.
- Flexible (Transnasal): Better tolerated, allows assessment during dynamic tasks like speech or singing.
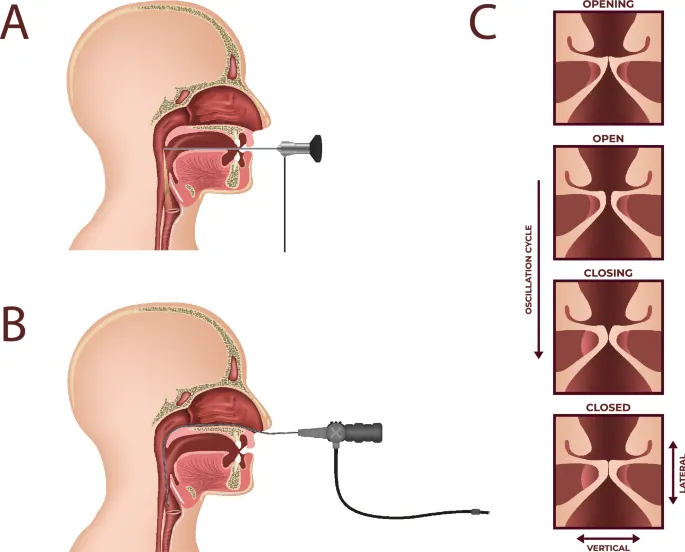
⭐ Stroboscopy is considered the clinical gold standard for evaluating vocal fold vibratory characteristics in most voice disorders.
Stroboscopy Deets - Flicker & Function
- Principle: Talbot's law & stroboscopic effect. Xenon light flashes synchronized near vocal fold $F_0$ create apparent slow-motion.
- Key Parameters (📌 Mnemonic: SAMPLe C & P):
- Symmetry of movement
- Amplitude of vibration
- Mucosal wave
- Periodicity
- **(L)**ateral excursion/edge
- Closure pattern (e.g., complete, gap)
- Phase (Symmetry & Closure)
- Also: Fundamental frequency ($F_0$), Non-vibrating portion.

- Advantages: Dynamic assessment, widely available.
- Limitations: Requires periodic vibration, $F_0$ tracking issues, not true slow motion.
⭐ Stroboscopy relies on the Talbot-Plateau law, creating an optical illusion of slow-motion vocal fold vibration by timing light flashes slightly offset from the vocal fold's fundamental frequency.
High-Speed Imaging - Real-Time Reels
-
Principle: Records actual vocal fold motion at high frame rates (e.g., 2000-8000 fps).
-
Comparison with Stroboscopy:
- HSDI: True, real-time motion.
- Stroboscopy: Apparent motion (illusion).
- Crucial for aperiodic/aphonic voices where stroboscopy is unreliable.
-
Derived Analyses:
- Videokymography (VKG): Spatiotemporal analysis of a single line across the glottis, detailing mucosal wave.
-
Advantages:
- Accurate depiction of vocal fold vibration.
- Effective for irregular/aperiodic vibrations.
- Provides detailed cycle-to-cycle information.
-
Disadvantages:
- Expensive equipment.
- Large data storage needs.
- Lengthy analysis time.
⭐ High-Speed Digital Imaging (HSDI) is particularly valuable for assessing highly dysphonic or aphonic patients where vocal fold vibration is too irregular for stroboscopy to track.
Pathology Spotting - Voice Vice Views
Stroboscopy & High-Speed Digital Imaging (HSDI) are crucial for visualizing vocal fold vibration and diagnosing pathologies.
| Pathology | Key Stroboscopic/HSDI Findings |
|---|---|
| Nodules | Bilateral, ↓ mucosal wave at lesion, hourglass closure, often symmetric |
| Polyps | Often unilateral, ↓ wave at lesion, incomplete closure, asymmetric |
| Cysts | Unilateral, absent/markedly ↓ wave over lesion, stiffness, adynamic segment |
| Paralysis | Immobility/paresis, asymmetric vibration, ↓/absent wave (affected side), glottic gap |
| Sulcus Vocalis | Groove/furrow, ↓/absent wave over sulcus, stiffness, spindle-shaped gap |
| Reinke's Edema | Bilateral, diffuse swelling, ↑ floppy mucosal wave, ↓ amplitude, often complete closure |
⭐ In vocal fold cysts, a key diagnostic feature on stroboscopy is the marked reduction or absence of the mucosal wave over the lesion, often contrasting with a more preserved wave on the rest of the fold.
High‑Yield Points - ⚡ Biggest Takeaways
- Stroboscopy: Apparent slow-motion of vocal folds via intermittent light (Talbot's Law), assessing mucosal wave.
- Key parameters: Amplitude, glottic closure pattern, periodicity, symmetry, and phase closure.
- High-Speed Videoendoscopy (HSV): Captures true, real-time vocal fold motion (2000-8000 fps).
- HSV excels for aperiodic/irregular vibrations, spasmodic dysphonia, and short phonatory segments.
- Stroboscopy is unreliable with severe aperiodicity; HSV provides accurate analysis.
- Both are crucial for diagnosing voice disorders and planning phonosurgery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

