Ear Embryology - Listen Up, Arches!
- Inner Ear (Otic Labyrinth): From otic placode (surface ectoderm) invaginating to form otic vesicle by 4th week. Forms membranous labyrinth (cochlea, vestibule, semicircular canals).
- Middle Ear:
- Tympanic cavity & Eustachian tube: 1st pharyngeal pouch (endoderm).
- Ossicles & Muscles:
Structure Arch Origin Nerve Supply Malleus, Incus 1st (Meckel's cartilage) V3 Tensor Tympani 1st V3 Stapes (suprastructure) 2nd (Reichert's cartilage) VII Stapedius Muscle 2nd VII
- External Ear:
- External Auditory Meatus (EAM): Dorsal part of 1st pharyngeal cleft (ectoderm).
- Auricle/Pinna: Fusion of 6 auricular hillocks (mesenchyme) from 1st (3) & 2nd (3) pharyngeal arches.
- Tympanic Membrane: Trilaminar: ectoderm (cleft), mesoderm, endoderm (pouch).
⭐ Malleus & Incus from 1st arch (Meckel's); Stapes (suprastructure) from 2nd arch (Reichert's).

Nose & Sinus Embryology - Sniffing Out Origins
- Nasal Cavity Development:
- 4th week: Nasal placodes (ectodermal thickenings) appear.
- 6th week: Placodes invaginate → nasal pits.
- Medial & lateral nasal prominences form around pits.
- Fusion of medial prominences → intermaxillary segment (philtrum, primary palate, premaxilla).
- Nasal pits deepen → primitive nasal cavity.
- Oronasal membrane ruptures (end of 6th week) → choanae.

- Paranasal Sinus Development: Evaginations of nasal mucosa.
- Maxillary: Starts 3rd-4th fetal month; present at birth.
- Ethmoidal: Starts 5th-6th fetal month; present at birth.
- Sphenoidal: Starts 5th-6th fetal month (as an ethmoidal outpouching); rudimentary at birth, pneumatizes postnatally.
- Frontal: Develops from anterior ethmoidal cells after birth (around 4-5 years); not visible on X-ray until ~6 years.
⭐ The maxillary sinus is the first paranasal sinus to develop, beginning in the 3rd-4th fetal month.
📌 Mnemonic for sinus development order (earliest to latest): My Elephant Sees Flies (Maxillary, Ethmoid, Sphenoid, Frontal).
Pharynx & Larynx Embryology - Pouch Power Plays
Pharyngeal Arch Derivatives:
| Arch | Nerve | Muscles | Cartilage/Skeletal |
|---|---|---|---|
| 1st | V3 (Trigeminal) | Mastication mm., Mylohyoid, Ant. digastric, Tensors (tympani, veli palatini) | Meckel's (Malleus, Incus), Mandible |
| 2nd | VII (Facial) | Facial expression mm., Stapedius, Stylohyoid, Post. digastric | Reichert's (Stapes, Styloid, Lesser hyoid) |
| 3rd | IX (Glossopharyngeal) | Stylopharyngeus | Greater hyoid |
| 4th-6th | X (Vagus: SLN-4th; RLN-6th) | Pharynx & Larynx mm. | Laryngeal cartilages |
- 1st: Middle ear cavity, Eustachian tube.
- 2nd: Palatine tonsil crypts.
- 3rd: Inferior parathyroid glands, Thymus. (📌 3rd pouch: Inf. Parathyroid & Thymus migrate caudally)
- 4th: Superior parathyroid glands, Ultimobranchial body (→ C cells).
Pharyngeal Clefts (Ectoderm):
- 1st: External auditory meatus.
- Others typically obliterate (failure → branchial cleft cyst).
Larynx: Develops from 4th & 6th arches. Laryngeal inlet recanalizes by 10th week.

⭐ Treacher Collins syndrome (1st arch defect) → Mandibulofacial dysostosis: hypoplastic mandible, zygomatic bones, malformed ears.
ENT Congenital Anomalies - Embryo's Oopsies
- Branchial Cleft Anomalies: Persistent pharyngeal clefts/pouches.
- Types: Cysts, sinuses, fistulae. Often along sternocleidomastoid's anterior border.
- Preauricular Sinus/Tag: Faulty fusion of 6 auricular hillocks (1st/2nd branchial arches).
- Choanal Atresia: Bony (90%) or membranous blockage of posterior nasal passage; failed bucconasal membrane rupture.
- Laryngeal Web: Incomplete laryngeal recanalization (10th week); glottic area common.
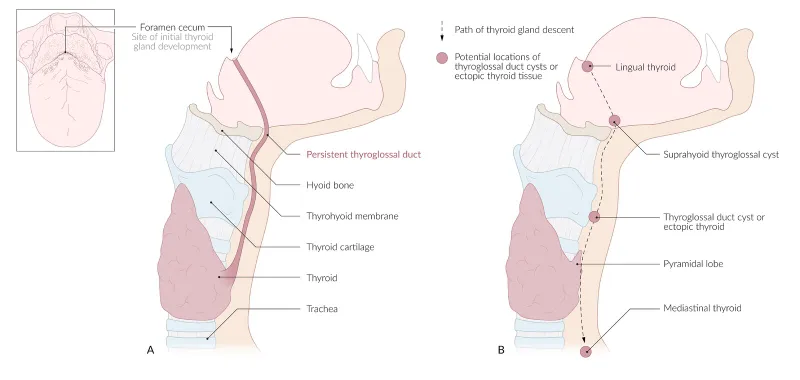
- Thyroglossal Duct Cyst: Midline neck mass from persistent thyroglossal duct.
- Cleft Lip/Palate: Failed fusion: medial nasal/maxillary prominences (lip); palatal shelves (palate).
⭐ Second branchial cleft anomaly is the most common type, accounting for approximately 95% of cases.
High‑Yield Points - ⚡ Biggest Takeaways
- Branchial arches (1st-6th) form key cartilage, nerves, muscles, and arteries of the head and neck.
- 1st Arch (Mandibular) derivatives include Meckel's cartilage, malleus, incus, muscles of mastication, and CN V3.
- 2nd Arch (Hyoid) derivatives include Reichert's cartilage, stapes, styloid process, muscles of facial expression, and CN VII.
- Pharyngeal pouches (endoderm): 1st forms Eustachian tube & middle ear; 2nd forms palatine tonsil fossa.
- The 1st Pharyngeal cleft (ectoderm) develops into the external auditory meatus.
- The thyroid gland originates from the foramen cecum at the tongue's base and descends.
- The otic placode gives rise to the membranous labyrinth of the inner ear (cochlea, semicircular canals).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

