Pharyngitis: Definition & Etiology - Sore Throat Origins
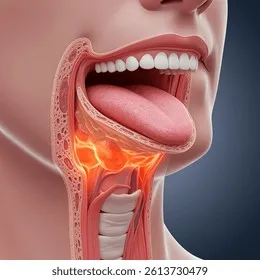
Pharyngitis: Inflammation of the pharynx, presenting as sore throat.
- Etiology (Causes):
- Infectious Agents (Predominant):
- Viral: Most common (~80% adults). E.g., Rhinovirus, Adenovirus, Influenza, Coronavirus, EBV, HSV.
- Bacterial: GABHS / S. pyogenes (main bacterial; esp. children 5-15 yrs). Others: M. pneumoniae, C. pneumoniae, N. gonorrhoeae, C. diphtheriae.
- Fungal: Candida albicans (immunocompromised).
- Non-Infectious Causes:
- Irritants (smoke, pollutants), GERD, allergies, trauma, vocal strain.
- Irritants (smoke, pollutants), GERD, allergies, trauma, vocal strain.
- Infectious Agents (Predominant):
⭐ Most cases of acute pharyngitis in adults are caused by viruses.
Pharyngitis: Clinical Features - Throat's Tale
-
Common Presentation: Sore throat (often severe, odynophagia), dysphagia, fever, pharyngeal erythema.
-
Distinguishing Features: Viral vs. Bacterial (GAS)
Feature Viral Pharyngitis Bacterial (GAS) Pharyngitis Onset & Fever Gradual; fever typically low-grade Sudden; high fever (>38°C or 100.4°F) Cough & Coryza Usually present Typically absent (important diagnostic clue) Tonsils/Pharynx Mild to moderate erythema; exudate rare Marked erythema; tonsillar swelling & exudates Cervical Nodes Diffuse, small, often non-tender Tender, enlarged anterior cervical lymph nodes Systemic Myalgia, fatigue, hoarseness, conjunctivitis Headache, nausea, vomiting, abdominal pain (esp. children)
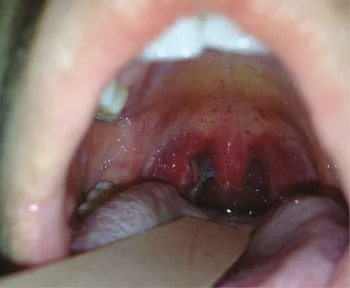
⭐ Palatal petechiae (petechial lesions on the soft palate or uvula) are highly suggestive of Group A Streptococcal pharyngitis.
- Suspicion for GAS ↑ with: Absence of cough, tonsillar exudates, history of fever, tender anterior cervical lymphadenopathy.
Pharyngitis: Diagnosis & DDx - The Whodunit
- Clinical Diagnosis: Sore throat, fever, odynophagia, tonsillar erythema/exudates, cervical lymphadenopathy.
- 📌 CENTOR Criteria (modified by McIsaac for age):
- Cough absent (+1)
- Exudates (tonsillar) (+1)
- Nodes (tender anterior cervical) (+1)
- Temperature (>38°C / 100.4°F) (+1)
- Age: 3-14 yrs (+1), 15-44 yrs (0), ≥45 yrs (-1)
- Interpretation:
- Score 0-1: Low GABHS risk; symptomatic treatment, no test/antibiotics.
- Score 2: Consider RADT or throat culture.
- Score ≥3: Perform RADT. If (+), treat for GABHS.
⭐ A negative Rapid Antigen Detection Test (RADT) in children and adolescents should be backed up by a throat culture.
- Differential Diagnosis (DDx):
- Viral (most common): Adenovirus, EBV (mononucleosis), Influenza.
- Bacterial: GABHS (key target!), Diphtheria (greyish pseudomembrane).
- Fungal: Candida (immunocompromised).
- Non-infectious: GERD, Kawasaki disease, Lemierre's syndrome.
Pharyngitis: Management & Complications - Healing Hurdle
-
Symptomatic Management:
- Analgesia (paracetamol, ibuprofen), lozenges, warm saline gargles, adequate hydration, rest.
-
GABHS Pharyngitis Management:
⭐ The primary goal of antibiotic treatment for GABHS pharyngitis is to prevent acute rheumatic fever.
-
Antibiotic Regimens for GABHS Pharyngitis:
Drug Child Dose Adult Dose Duration Notes Penicillin V 250mg BID-TID 500mg BID-QID 10 days Gold Std Amoxicillin 50mg/kg OD (max 1g) 1g OD / 500mg TID 10 days Palatable Benzathine Pen G 0.6MU (<27kg); 1.2MU (≥27kg) IM Single Dose Compliance Pen-Allergy: Cephalexin 20mg/kg/dose BID (max 500mg/dose) 500mg BID 10 days Non-anaphyl. Clindamycin 7mg/kg/dose TID (max 300mg/dose) 300mg TID 10 days Azithromycin 12mg/kg OD (max 500mg) 500mg OD 5 days
-
-
Management Algorithm:
-
Complications:
- Suppurative: Peritonsillar abscess (quinsy), retropharyngeal abscess, otitis media, sinusitis, cervical lymphadenitis.
- Non-suppurative: Acute Rheumatic Fever (ARF), Post-Streptococcal Glomerulonephritis (PSGN), PANDAS.
-
Referral Criteria (Red Flags):
- Airway compromise (stridor, drooling), severe dysphagia/dehydration, toxic appearance, neck stiffness/swelling, failure to improve in 48-72 hrs, suspected suppurative complications (e.g., quinsy).
High‑Yield Points - ⚡ Biggest Takeaways
- Viral infections are the most frequent cause of pharyngitis.
- Group A Streptococcus (GAS) is the primary bacterial pathogen, potentially causing rheumatic fever and PSGN.
- Centor criteria (fever, exudates, tender anterior cervical nodes, absence of cough) suggest GAS.
- Penicillin (or amoxicillin) is crucial for GAS pharyngitis to prevent complications.
- Diphtheria features a greyish-white pseudomembrane and "bull neck".
- Infectious Mononucleosis (EBV) presents with posterior cervical lymphadenopathy, splenomegaly, and atypical lymphocytes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

