Definition & Types - Swallow Saga Starts
- Dysphagia: Subjective sensation of difficulty or abnormality of swallowing. Food "sticking" or not passing correctly from mouth to stomach.

- Classification: Based on anatomical location of perceived problem.
| Feature | Oropharyngeal (Transfer) Dysphagia | Esophageal Dysphagia |
|---|---|---|
| Site of Problem | Oropharynx, Larynx, UES | Esophageal body, LES |
| Key Difficulty | Initiating swallow; bolus transfer from mouth to esophagus | Passage of bolus through esophagus |
| Common Symptoms | Nasal regurgitation, coughing/choking during swallow, drooling, dysarthria | Sensation of food stuck retrosternally, chest pain, regurgitation of undigested food |
| Liquids/Solids | Difficulty with liquids > solids (or both) | Solids > liquids (mechanical); Both (motility) |
Etiology - Who's Blocking?
Dysphagia, or difficulty swallowing, stems from problems in the oropharyngeal transfer phase or esophageal transport. Key causes include:
| Oropharyngeal (Transfer) Dysphagia | Esophageal Dysphagia |
|---|---|
| Neuromuscular: | Motility: |
| * Stroke, Parkinson's | * Achalasia, Scleroderma |
| * Myasthenia Gravis (MG), MND | * Diffuse Esophageal Spasm (DES) |
| Structural: | Mechanical (Intrinsic): |
| * Zenker's diverticulum | * Strictures (Peptic, Malignant) |
| * Tumors (pharyngeal/laryngeal) | * Rings (Schatzki), Webs |
| * Webs (e.g., Plummer-Vinson) | * Tumors (Esophageal cancer) |
| * Eosinophilic Esophagitis (EoE) | |
| Mechanical (Extrinsic): | |
| * Mediastinal mass, Vascular anomaly |
⭐ In adults, GERD is the most common cause of intermittent solid food dysphagia due to peptic strictures.
Clinical Evaluation & Diagnosis - Cracking the Case
-
History is key: Differentiate Oropharyngeal (difficulty initiating, nasal regurgitation, aspiration, coughing/choking) vs. Esophageal (food "sticking" sensation, retrosternal). Note solids/liquids, progression, duration, alarm symptoms (weight loss, odynophagia, anemia).
-
Examination: Thorough oral cavity, cranial nerve assessment (IX, X, XII), neck for masses, observe swallowing.
-
Investigations:
-
Barium Swallow: Initial for structural lesions (strictures, webs, rings). Useful for achalasia ("bird beak" appearance).
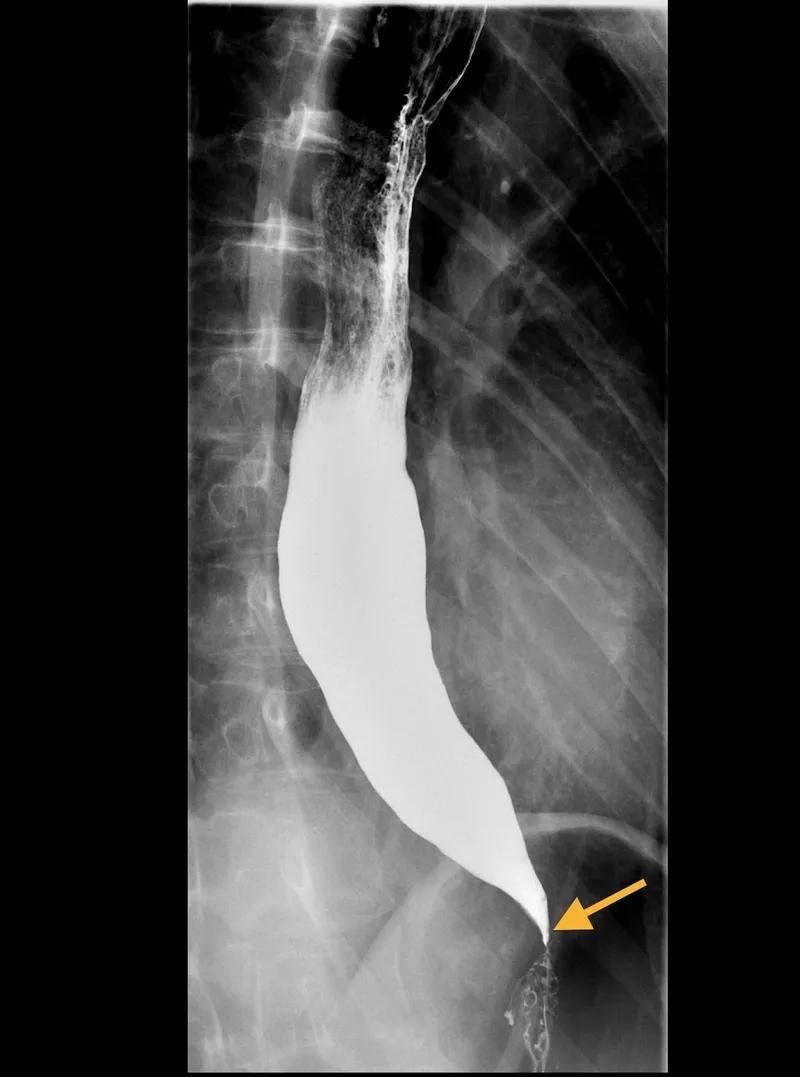
-
Upper GI Endoscopy (EGD): Direct visualization, biopsy, therapeutic intervention.
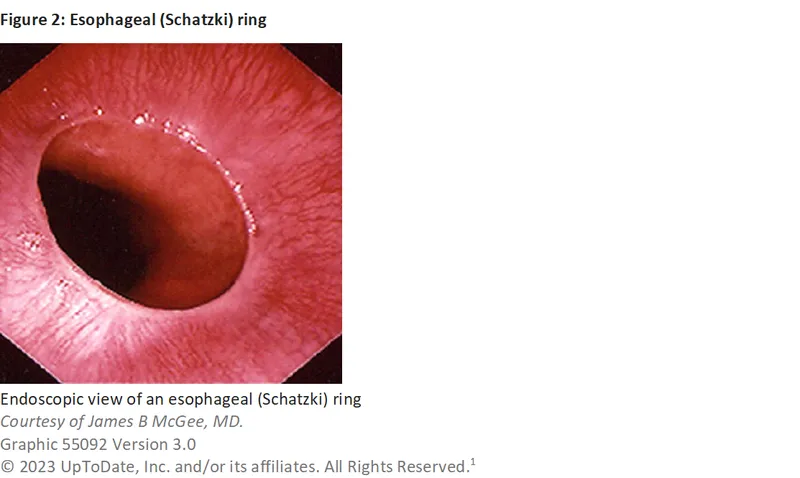
-
Esophageal Manometry: Gold standard for motility disorders (e.g., achalasia: LES pressure > 45 mmHg, incomplete LES relaxation).
-
Videofluoroscopic Swallowing Study (VFSS) / Fiberoptic Endoscopic Evaluation of Swallowing (FEES): For oropharyngeal dysphagia.
-
⭐ Endoscopy with biopsy is mandatory if malignancy is suspected or to evaluate structural lesions.
Red Flags & Specific Conditions - Danger Signals
Red Flags:
- Significant unexplained weight loss
- Progressive dysphagia (solids → liquids)
- Odynophagia (painful swallowing)
- Persistent hoarseness
- Associated neurological deficits
- New onset dysphagia in age > 50 years
- Signs of anemia or GI bleeding
- Palpable neck mass
Specific Conditions:
- Achalasia Cardia:
- LES non-relaxation, esophageal aperistalsis.
- 📌 Bird's Beak on barium swallow. Dysphagia (solids & liquids).

- Zenker's Diverticulum:
- Pulsion diverticulum (Killian's dehiscence).
- Regurgitation (undigested food), halitosis, gurgling.
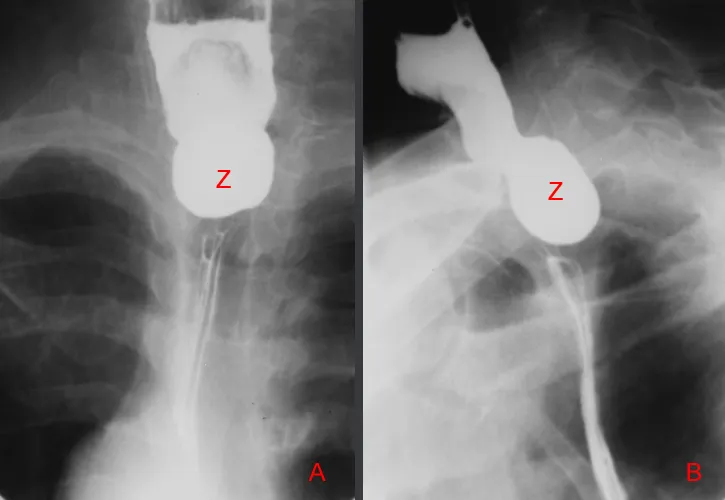
⭐ Zenker's diverticulum is a pulsion diverticulum in Killian's dehiscence, presenting with regurgitation of undigested food and halitosis.
- Plummer-Vinson Syndrome (PVS):
- 📌 PVS = Post-cricoid web, Iron deficiency anemia, Spoon nails (koilonychia).
- ↑ Esophageal/pharyngeal SCC risk.
- Pharyngeal/Esophageal Malignancy:
- Progressive dysphagia (solids first), weight loss, anorexia.
- Often Squamous Cell Carcinoma (SCC).
- Myasthenia Gravis:
- Fluctuating muscle weakness.
- Dysphagia worse with repetitive swallowing/end of day. Ptosis, diplopia.
High‑Yield Points - ⚡ Biggest Takeaways
- Dysphagia: Difficulty swallowing; distinguish oropharyngeal (initiation, neuromuscular) from esophageal (food stuck, mechanical/motility).
- Oropharyngeal causes: Stroke, Myasthenia Gravis; investigate with Modified Barium Swallow.
- Esophageal causes: Strictures, Achalasia, Tumors; Endoscopy is primary investigation.
- Achalasia: "Bird-beak" on barium, impaired LES relaxation.
- Plummer-Vinson Syndrome: Triad of dysphagia, iron-deficiency anemia, esophageal webs.
- Scleroderma esophagus: Features aperistalsis and severe GERD.
- Red flags: Weight loss, progressive dysphagia demand urgent evaluation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

