Sialolithiasis - Stone Cold Facts
- Definition: Salivary gland stones.
- Epidemiology: Middle-aged adults; M > F.
- Most Affected Glands:
- Submandibular (80-90%): 📌 SMART (SubMandibular Anatomy Reasons for Trouble (Stones)) - Wharton's duct (long, tortuous, upward); saliva (↑ viscosity, alkaline, ↑ mucin, ↑ Ca).
- Parotid (10-20%).
- Sublingual/Minor (1-2%).
- Pathogenesis: Stasis, inflammation, organic nidus, calcium phosphate deposition.
- Risk Factors: Dehydration, anticholinergics, smoking, gout, hyperparathyroidism, ductal stenosis.
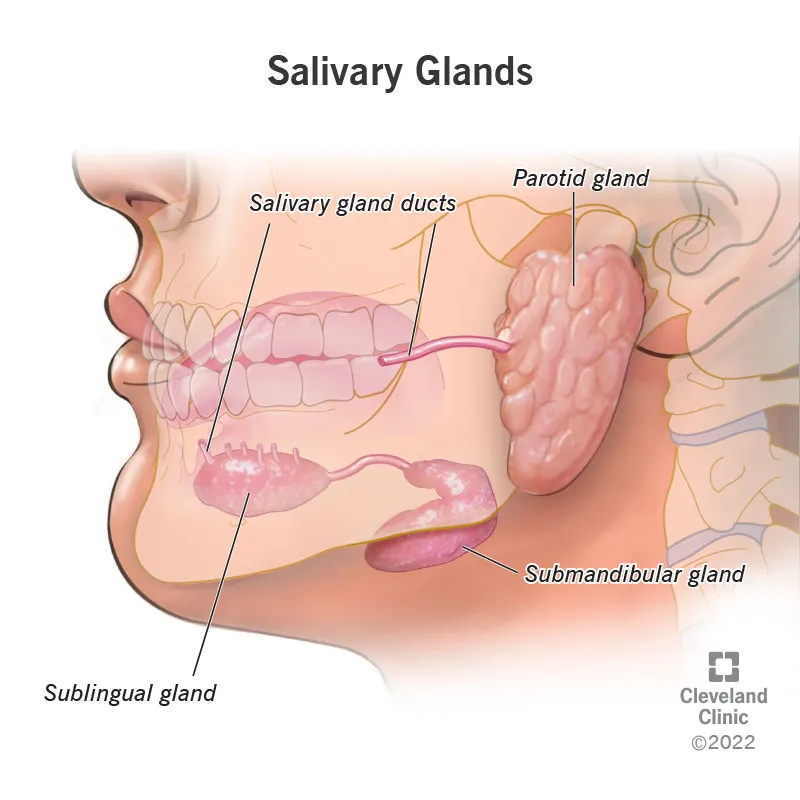
⭐ Submandibular gland is most commonly affected (80-90%) due to the long, tortuous, upward course of Wharton's duct and thicker, alkaline, mucin-rich saliva.
Sialolithiasis - Salty Symptoms Show
- Hallmark: Intermittent, painful gland swelling, worse with meals (📌 'mealtime syndrome' / 'gustatory colic').
- Symptoms:
- Pain, swelling, tenderness.
- Palpable stone (if superficial).
- ↓ or absent salivation (affected duct).
- Recurrent sialadenitis.
- Signs:
- Stone palpable bimanually along duct.
- Purulent discharge from duct (if infected).
- Location Specifics:
- Submandibular: palpable in mouth floor.
- Parotid: near Stensen's duct opening.
⭐ 'Mealtime syndrome' (colicky pain/swelling with meals due to salivary stimulation) strongly suggests sialolithiasis.
Sialolithiasis - Spotting the Stone
- Clinical Examination:
- Inspection: Glandular swelling, redness over duct orifice.
- Palpation: Firm, tender gland; stone may be palpable (bimanual palpation for submandibular gland).
- Imaging Modalities:
- X-rays (Occlusal/Panoramic): Show radiopaque stones (Submandibular ~80-90%, Parotid ~50-60% radiopaque).
- Ultrasound (USG): Initial modality. Detects stones >2mm, ductal dilatation. Non-invasive.
- Sialography: Visualizes ductal system, filling defects. Contraindicated in acute infection or iodine allergy.
- CT Scan (Non-contrast): High sensitivity for small/radiolucent stones, intraglandular stones.
- MR Sialography: Non-invasive, no radiation, good for ductal anatomy.
- Sialendoscopy: Diagnostic and therapeutic; direct visualization.
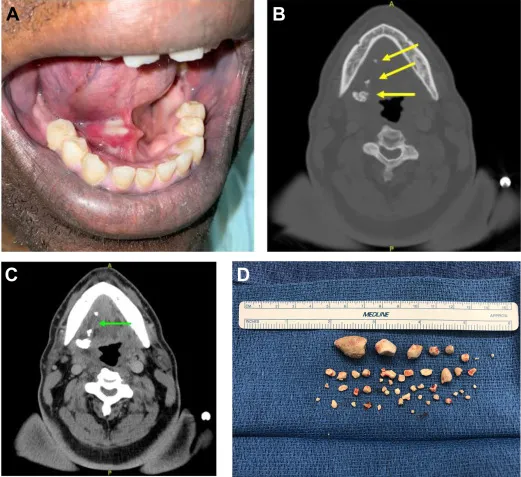
⭐ High-resolution non-contrast CT (HR-NCCT) is the gold standard for detecting salivary stones, especially small or radiolucent ones.
Sialolithiasis - Stone Eviction Plan
- Conservative Management (First-line): Hydration, sialogogues, gland massage, moist heat. Analgesics; antibiotics for infection.
- Minimally Invasive Techniques:
- Sialendoscopy: For stones < 5mm (SMG duct), < 3mm (parotid). Basket retrieval, laser/mechanical lithotripsy.
- ESWL: For solitary, radiopaque stones < 10mm (parotid/SMG).
- Surgical Approaches (if others fail/unsuitable):
- Transoral Ductal Slitting/Sialodochotomy: For palpable distal duct stones.
- Sialadenectomy (Gland Removal): Last resort. Large/multiple intraglandular, recurrent stones; severe gland damage; failed interventions.
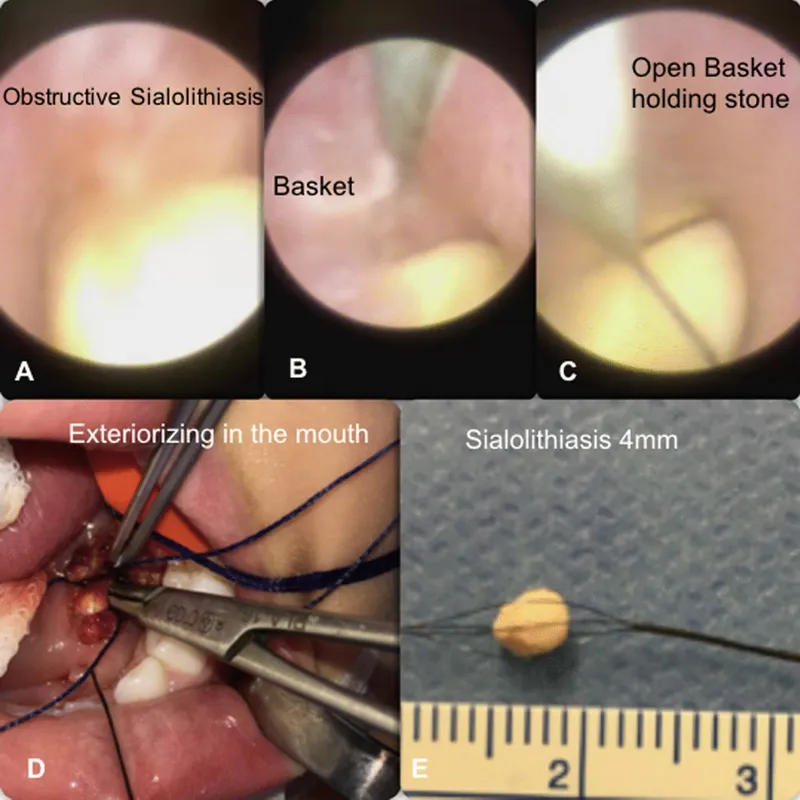
⭐ Sialendoscopy has revolutionized management, offering a gland-preserving, minimally invasive approach for both diagnosis and treatment of most sialoliths.
Sialolithiasis - Dodging Duct Drama
- Complications & Sequelae:
- Acute/chronic sialadenitis
- Ductal stricture/stenosis
- Glandular atrophy/fibrosis (due to chronic obstruction/inflammation)
- Abscess formation
- Salivary fistula (rare)
- Prevention Strategies:
- Adequate hydration
- Good oral hygiene
- Management of underlying risk factors (e.g., gout)
⭐ Chronic obstruction from sialolithiasis can lead to irreversible glandular damage and atrophy, emphasizing the need for timely management.
High‑Yield Points - ⚡ Biggest Takeaways
- Most common: Submandibular gland (Wharton's duct) due to alkaline, viscous saliva & upward duct course.
- Composition: Primarily calcium phosphate; mostly radio-opaque (80-90% submandibular).
- Key symptom: Mealtime syndrome - colicky pain and swelling with meals.
- Diagnosis: Palpation, X-ray (occlusal view), USG, CT. Sialography can be diagnostic.
- Management: Conservative (sialogogues), transoral removal, sialendoscopy, or gland excision for refractory cases.
- Parotid stones are less frequent, often smaller and may be radiolucent more often than submandibular stones.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

