Epiglottitis Essentials - Fiery Throat Peril
- Definition: Acute inflammation of epiglottis & supraglottic structures, potentially causing life-threatening airway obstruction.
- Etiology:
- Historically: Haemophilus influenzae type b (Hib) - incidence ↓ with vaccination.
- Currently (vaccinated/adults): Streptococcus pneumoniae, Staphylococcus aureus, Group A Streptococcus, viruses, fungi, thermal injury.
- Pathogenesis: Infection/insult → rapid, severe edema & erythema of epiglottis, aryepiglottic folds, arytenoids → airway narrowing.
⭐ In unvaccinated children, H. influenzae type b (Hib) remains the primary cause; in vaccinated populations, Streptococcus spp. and S. aureus are more frequent culprits of epiglottitis in adults and children alike.
Symptom Spotlight - Distress Signals
- Rapid, fulminant onset (hours) with high fever, severe sore throat.
- 📌 The 4 D's are key:
- Dysphagia: Painful swallowing, leading to refusal to eat/drink.
- Drooling: Unable to manage oral secretions.
- Distress: Respiratory distress, anxiety, air hunger.
- Dysphonia: Voice change, often muffled.
- Inspiratory stridor: Often a late, alarming sign of airway compromise.
- Tripod posture: Patient sits upright, leans forward, neck extended, chin out.
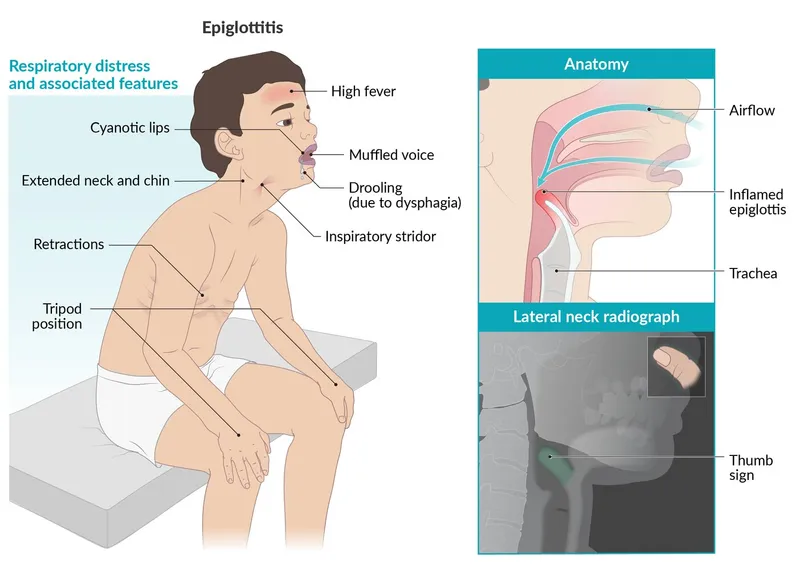
⭐ Muffled voice, often termed 'hot potato voice', is characteristic.
Diagnostic Detective - Unmasking the Culprit
- Direct Laryngoscopy (Definitive):
- Best performed in OR/controlled setting, especially in children.
- Shows 'cherry-red', swollen, oedematous epiglottis.
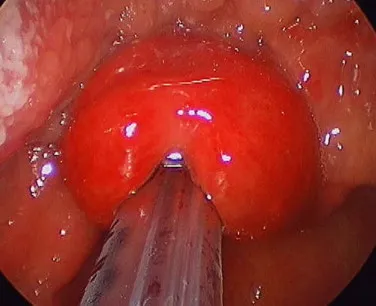
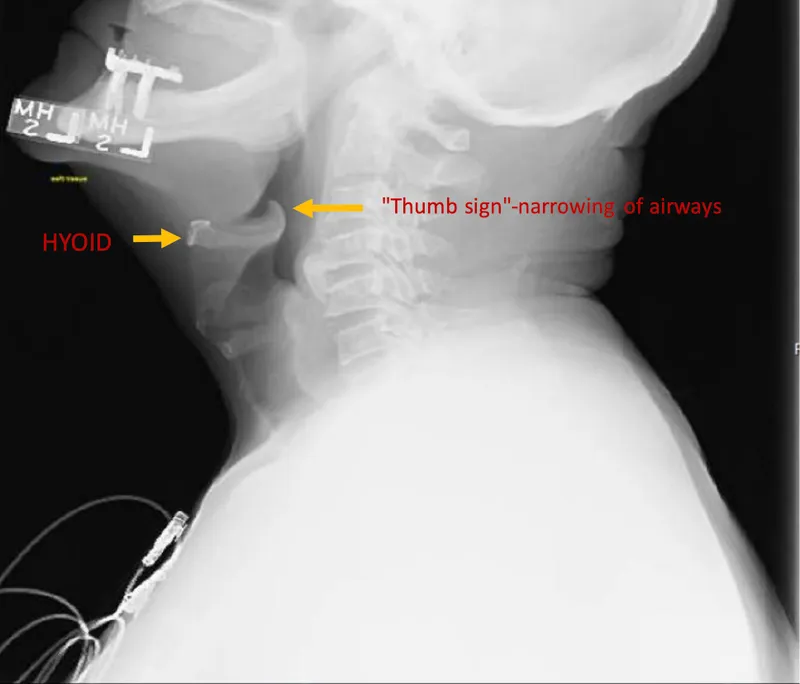
- Lateral Neck X-ray:
- Classic 'thumb sign' (swollen epiglottis).
- Thickened aryepiglottic folds, obliterated vallecula.
- Blood cultures: May identify pathogen (e.g., Hib).
- CBC: ↑ WBC count.
⭐ Avoid routine oral examination with a tongue depressor in children with suspected epiglottitis outside a controlled setting (e.g., OR) due to risk of precipitating acute airway obstruction.
Airway & Action - Lifesaving Moves
- Immediate Goal: Secure airway. Keep patient calm, upright; avoid upsetting maneuvers.
- Team Alert: Senior ENT, Anesthesia, Pediatrics.
- Definitive Airway (OR/ICU):
- Endotracheal intubation by skilled personnel.
- Surgical airway (cricothyroidotomy/tracheostomy) if intubation fails/contraindicated.
- Post-Airway Rx:
- IV Ceftriaxone (e.g., 50-75 mg/kg/day).
- IV Dexamethasone (e.g., 0.15-0.6 mg/kg).
- Humidified O2, IV fluids.
- Monitoring: ICU admission for close observation.
⭐ Securing the airway is the foremost priority, often requiring intubation or tracheostomy in a controlled environment like OR.
Beyond the Flare-up - Complications & Shield
- Complications (Rapid & Severe):
- Airway Obstruction: Hypoxia, anoxic brain injury, death.
- Epiglottic Abscess: Localized pus; may require incision & drainage.
- Descending Infection: Pneumonia, mediastinitis, empyema.
- Systemic Spread: Sepsis, septic shock, meningitis (if bacteremia).
- Rare: Vocal cord paralysis, post-obstructive pulmonary edema.
- Shield (Proactive Defense):
- ⭐ > The Haemophilus influenzae type b (Hib) vaccine is primary prevention, dramatically reducing pediatric epiglottitis incidence.
- Chemoprophylaxis: Rifampicin for unvaccinated close contacts (household, daycare) to eradicate carriage, preventing secondary cases.
High‑Yield Points - ⚡ Biggest Takeaways
- Etiology: Primarily Haemophilus influenzae type b (Hib), though incidence ↓ post-vaccination; also Streptococcus spp.
- Pediatric Triad: Dysphagia, Drooling, Distress; often assumes tripod position.
- Adult Presentation: Severe sore throat (out of proportion), odynophagia, muffled "hot potato" voice.
- Key Sign: Thumbprint sign on lateral neck X-ray is characteristic.
- Definitive Diagnosis: Laryngoscopy (cherry-red, swollen epiglottis), done cautiously.
- Management Priority: Secure airway (intubation/tracheostomy); followed by IV antibiotics (e.g., ceftriaxone).
- Major Complication: Rapidly progressive airway obstruction.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

