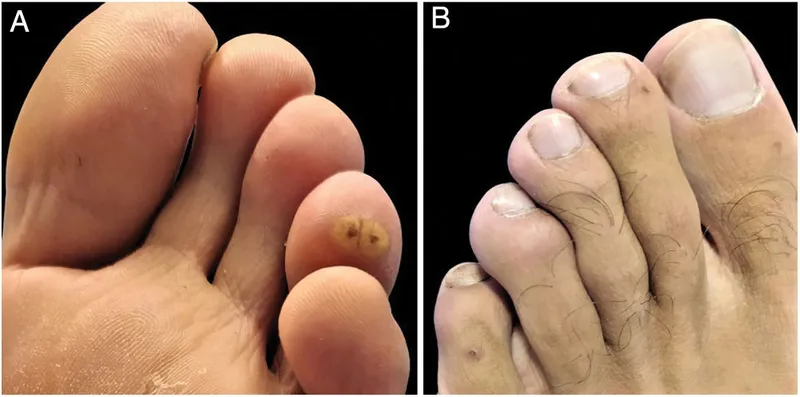
Tungiasis - Flea's Foot Fetish
- Definition: Ectoparasitic infection caused by the sand flea Tunga penetrans (jigger flea).
- Common Names: Jigger, chigoe flea, nigua, sand flea disease.
- Pathogenesis: Impregnated female flea burrows into the skin, typically feet (periungual, interdigital spaces), causing intense inflammation.
- Flea feeds on blood and lymph, hypertrophies, and expels eggs.
- Dies in situ after 2-3 weeks.

- Clinical Features: Papule → nodule with a central black dot (flea's posterior end).
- Itching, pain, edema, ulceration, and secondary bacterial infection are common.
- 📌 Mnemonic: Tiny Ugly Nasty Grubby Attackers Spoil Innocent Skin (TUNGASIS)
⭐ Most common sites are feet, especially periungual areas and interdigital folds; hands can also be affected in children or those with extensive exposure.
- Complications: Auto-amputation of digits, tetanus, gangrene, sepsis.
- Diagnosis: Clinical; dermoscopy shows flea segments or eggs.
Tungiasis - Burrower's Blueprint
- Causative Agent: Tunga penetrans (sand flea, jigger).
- Geography: Endemic in tropical/subtropical regions: Latin America, Caribbean, Sub-Saharan Africa, India.
- Risk Factors:
- Walking barefoot in sandy/dry soil.
- Poverty, poor housing, rural areas.
- Contact with infested animals (pigs, dogs, cats, rats).
- Lifecycle & Pathogenesis:
- Gravid female flea burrows into epidermis (feet, periungual areas common).
- Feeds on blood, hypertrophies (neosome), expels eggs to environment.
- Host inflammatory reaction: pain, itching, erythema, edema.
- Lesion: white/yellowish papule/nodule with central black dot (flea's posterior).

⭐ Exam Favourite: Secondary bacterial infections (e.g., Staphylococcus, Streptococcus) are common complications, leading to cellulitis, abscesses, tetanus, or gangrene if untreated. Lesions are typically found on feet, especially periungual areas, soles, and interdigital spaces (📌 "Toe-jam terror").
Tungiasis - Spot the Squatter
- Causative Agent: Tunga penetrans (sand flea, jigger). Female burrows into skin.
- Clinical Features:
- Initial: Erythematous papule at penetration site.
- Develops into: White, firm, itchy, painful nodule (1-10 mm) with a central black dot (flea's posterior).
- Common sites: Feet (soles, periungual, interdigital spaces), hands.
- Symptoms: Intense pruritus, pain, foreign body sensation.
- Progression (Simplified):
- Penetration & engorgement (days 1-2).
- Maximum hypertrophy & egg laying (week 1-3).
- Involution: Flea dies, expelled; lesion crusts (weeks 3-5).
- Residual: Scar, callus.
- Complications:
- Severe inflammation, ulceration.
- Secondary bacterial infections (cellulitis, abscess, tetanus, gangrene).
- Fissuring, desquamation.
- Nail dystrophy, auto-amputation (rare).
- Diagnosis: Primarily clinical. Dermoscopy shows flea segments.
⭐ The characteristic "black dot" in the center of a tungiasis lesion is the posterior abdomen and hind legs of the burrowed female flea, used for breathing and defecation.
Tungiasis - Evict & Protect
- Eviction (Flea Removal):
- Sterile extraction: Needle, forceps, or curette.
- Complete flea removal vital to prevent inflammation.
- Wound care: Antiseptics; antibiotics if secondary infection.
- Tetanus prophylaxis if indicated.
- Topical Pharmacotherapy:
- Dimethicone (NYDA): Suffocates flea, highly effective.
- Topical ivermectin or thiabendazole.
- Cryotherapy or electrocautery for resistant lesions.
- Protection & Prevention:
- Regular use of closed footwear.
- Insect repellents (e.g., DEET, picaridin).
- Environmental control: Insecticide spray (floors, animal sites).
- Treat infected domestic animals (dogs, pigs).

⭐ The female Tunga penetrans flea burrows head-first, leaving its posterior end exposed for breathing, defecation, and egg expulsion.
High‑Yield Points - ⚡ Biggest Takeaways
- Causative Agent: Gravid female sand flea, Tunga penetrans.
- Common Sites: Feet (periungual, interdigital, soles); also hands.
- Characteristic Lesion: Painful, itchy papule/nodule with a central black dot (flea's exposed abdomen/ova).
- Primary Symptoms: Intense pruritus, pain, and localized inflammation.
- Major Complications: Secondary bacterial infections (cellulitis, abscess), tetanus, ulceration.
- Treatment of Choice: Surgical extraction of the intact flea; ensure tetanus prophylaxis.
- Prevention: Use of closed footwear in endemic areas_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more