Tropical Dermatology

On this page
🌴 Tropical Dermatology: The Heat Zone Skin Survival Guide
Tropical climates transform skin into a battleground where heat, humidity, and unique pathogens create disease patterns you'll rarely see in temperate zones. You'll learn to recognize the distinct invasion strategies of tropical organisms, from leishmaniasis ulcers to chromoblastomycosis plaques, then master the clinical reasoning that separates mimics and guides targeted treatment. This lesson builds your diagnostic framework from pathogen behavior through therapeutic algorithms, connecting individual cases to global surveillance patterns that make you an effective clinician wherever medicine takes you.
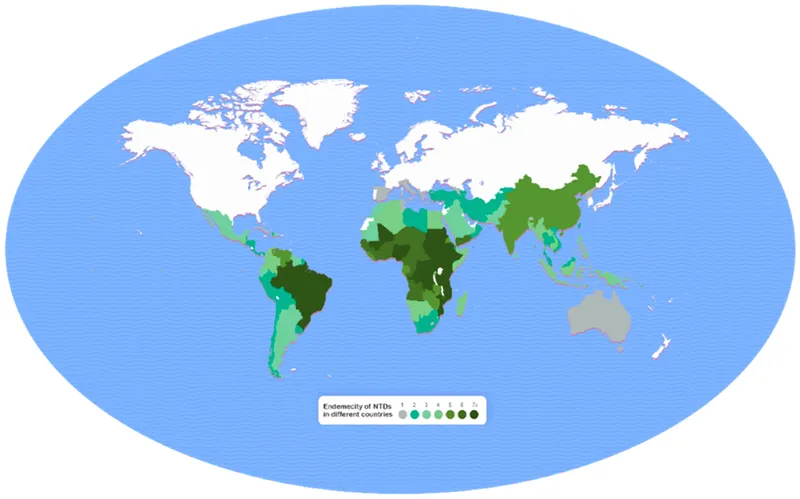
Foundation Architecture: The Tropical Skin Battlefield
Tropical skin diseases operate within a triadic framework of environmental factors, pathogen characteristics, and host vulnerability. Temperature ranges of 25-35°C with humidity >70% create optimal conditions for vector breeding and pathogen survival.
-
Environmental Amplifiers
- Temperature: >25°C accelerates pathogen replication by 300%
- Humidity: >70% extends vector survival to 21+ days
- Rainfall: >1000mm annually creates breeding grounds
- Standing water increases vector density 10-fold
- Flooding disperses soil-dwelling pathogens
- Poor drainage sustains transmission cycles
-
Pathogen Categories by Transmission
- Vector-borne: 40% of tropical skin diseases
- Direct contact: 35% through contaminated surfaces
- Soil-mediated: 15% via barefoot exposure
- Water-related: 10% through contaminated sources
📌 Remember: MOIST - Mosquitoes, Organisms, Immunity, Soil, Temperature - the five pillars determining tropical skin disease patterns
| Disease Category | Primary Vector | Incubation Period | Peak Transmission Season | Geographic Hotspots |
|---|---|---|---|---|
| Leishmaniasis | Sandfly | 2-8 weeks | Dry season | Middle East, India |
| Filariasis | Mosquito | 6-12 months | Monsoon | Sub-Saharan Africa |
| Onchocerciasis | Blackfly | 12-18 months | Year-round | West Africa |
| Myiasis | Botfly | 3-6 weeks | Wet season | Central America |
| Tungiasis | Sand flea | 7-14 days | Dry season | Brazil, Kenya |
💡 Master This: Every tropical skin lesion requires geographic history - knowing the patient's travel timeline within 6 months predicts 90% of possible pathogens
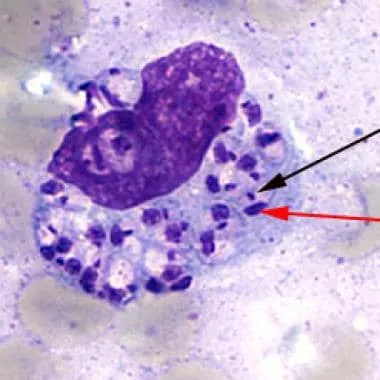
The foundation of tropical dermatology mastery lies in recognizing that climate drives pathogen behavior, creating predictable disease patterns that enable rapid diagnosis. Connect this environmental framework through pathophysiological mechanisms to understand how tropical pathogens exploit skin vulnerabilities.
🌴 Tropical Dermatology: The Heat Zone Skin Survival Guide
🔬 Pathogen Warfare: The Tropical Invasion Strategies
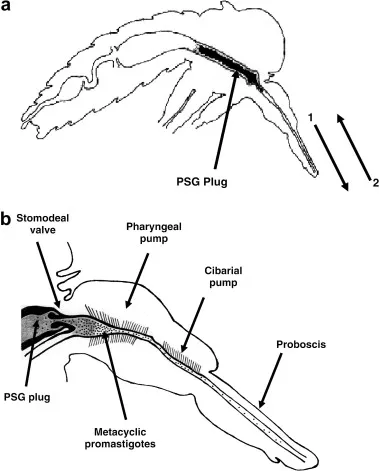
Vector-Mediated Precision Strikes
Vector-borne pathogens utilize arthropod delivery systems with surgical precision. Sandflies inject 10-100 Leishmania promastigotes per bite, while mosquitoes deliver 1,000-10,000 microfilariae directly into dermal capillaries.
-
Sandfly Leishmania Delivery
- Proboscis penetration: 0.1-0.3mm depth
- Saliva volume: 0.1-0.5 microliters
- Parasite load: 10²-10⁴ promastigotes
- Survival rate in skin: 60-80% at 24 hours
- Macrophage invasion: 2-6 hours post-injection
- Lesion development: 2-8 weeks incubation
-
Mosquito Microfilaria Transport
- Feeding duration: 3-5 minutes average
- Blood volume: 2-5 microliters per feeding
- Larval transfer: 10-40 L3 larvae per bite
- Lymphatic migration: 24-48 hours
- Adult development: 6-12 months
- Microfilaria production: 1,000-50,000 daily
📌 Remember: BITE - Blood meal, Injection depth, Transmission load, Establishment time - the vector delivery parameters determining infection success
Direct Penetration Mechanisms
Soil-dwelling pathogens employ mechanical and enzymatic penetration strategies. Hookworm larvae penetrate intact skin within 5-10 minutes using collagenase and hyaluronidase enzymes.
- Enzymatic Breakdown Cascade
- Collagenase activity: pH 7.0-8.5 optimal
- Hyaluronidase concentration: 100-500 units/ml
- Penetration rate: 0.5-2.0mm per hour
- Stratum corneum breach: 2-5 minutes
- Dermal invasion: 10-30 minutes
- Vascular access: 1-3 hours
⭐ Clinical Pearl: Barefoot exposure accounts for 85% of soil-transmitted skin infections - protective footwear reduces transmission by >95%
| Pathogen | Penetration Method | Time to Breach | Enzyme Arsenal | Clinical Onset |
|---|---|---|---|---|
| Hookworm larvae | Enzymatic | 5-10 minutes | Collagenase, Hyaluronidase | 24-48 hours |
| Strongyloides | Mechanical + Enzymatic | 10-20 minutes | Metalloprotease | 2-7 days |
| Schistosome cercariae | Mechanical | 2-5 minutes | Elastase | 4-12 hours |
| Tungiasis flea | Mechanical burrowing | 30-60 minutes | Mandible action | 7-14 days |
| Botfly larvae | Wound deposition | Immediate | None required | 1-3 weeks |
Understanding invasion strategies reveals why prevention timing is critical - most tropical skin pathogens establish infection within minutes to hours of contact. Connect these mechanisms through clinical recognition patterns to identify early intervention opportunities.
🔬 Pathogen Warfare: The Tropical Invasion Strategies
🎯 Recognition Mastery: The Tropical Skin Detective Framework
The Big 5 Morphological Signatures
Each tropical pathogen creates signature lesion patterns determined by invasion route, tissue tropism, and host immune response. Recognition depends on identifying key discriminating features within seconds.
-
Ulcerative Patterns (35% of cases)
- Leishmaniasis: Volcano crater with raised borders
- Tropical ulcer: Punched-out with undermined edges
- Buruli ulcer: Painless with necrotic base
- Border characteristics: 90% diagnostic accuracy
- Pain presence: Distinguishes bacterial vs parasitic
- Depth assessment: Predicts treatment duration
-
Nodular Patterns (25% of cases)
- Onchocerciasis: Mobile subcutaneous nodules
- Mycetoma: Fixed, draining nodules with grains
- Sporotrichosis: Linear ascending nodular chain
- Mobility: Fixed = deep infection
- Drainage: Purulent = bacterial, granular = fungal
- Distribution: Linear = lymphatic spread
📌 Remember: MOUND - Mobility, Ostium (drainage), Underlying fixation, Number, Distribution - the nodule assessment framework
Geographic-Temporal Correlation Matrix
Location + timing = diagnosis in 70% of tropical skin diseases. Master the geographic-pathogen correlation and you'll narrow differentials immediately.
-
Sub-Saharan Africa Signatures
- Onchocerciasis: River blindness belt - 31 countries
- Buruli ulcer: Wetland proximity within 200m
- Tungiasis: Sandy soil regions with <500mm rainfall
- Seasonal peaks: Dry season = 80% of cases
- Age distribution: Children = 60% of infections
- Occupation risk: Farmers = 5x higher incidence
-
South Asian Patterns
- Leishmaniasis: Bihar, West Bengal - 90% of Indian cases
- Filariasis: Coastal regions with monsoon flooding
- Tropical ulcers: Rural areas with poor sanitation
- Monsoon correlation: 3x increase during wet season
- Urban vs rural: 10:1 rural predominance
- Socioeconomic factors: Poverty = primary risk
⭐ Clinical Pearl: Travel history within 6 months provides 85% diagnostic accuracy for tropical skin diseases - always ask about specific regions and seasonal timing
| Geographic Region | Top 3 Skin Diseases | Peak Season | Key Risk Factors | Diagnostic Clues |
|---|---|---|---|---|
| West Africa | Onchocerciasis, Buruli, Tungiasis | Dry season | River proximity | Nodules + blindness |
| East Africa | Leishmaniasis, Myiasis, Tropical ulcer | Post-rainy | Conflict zones | Ulcers + scarring |
| South Asia | Filariasis, Leprosy, Chromoblastomycosis | Monsoon | Flooding areas | Lymphedema + nodules |
| Central America | Cutaneous larva migrans, Sporotrichosis | Wet season | Beach/garden exposure | Serpentine tracks |
| Amazon Basin | Leishmaniasis, Myiasis, Paracoccidioidomycosis | Year-round | Forest exposure | Multiple ulcers |
Pattern recognition mastery transforms complex tropical presentations into systematic diagnostic workflows. Connect these recognition frameworks through differential analysis to build comprehensive diagnostic strategies.
🎯 Recognition Mastery: The Tropical Skin Detective Framework
⚖️ Differential Mastery: The Tropical Skin Discrimination Matrix
Ulcerative Lesion Discrimination Matrix
Ulcerative tropical diseases share overlapping morphologies but differ in quantifiable characteristics. Use the 5-parameter discrimination system for >90% accuracy.
-
Border Architecture Analysis
- Leishmaniasis: Raised, indurated borders 2-5mm elevation
- Buruli ulcer: Undermined borders extending 5-15mm
- Tropical ulcer: Sloping borders with minimal undermining
- Border-to-base ratio: Leishmaniasis >1:3
- Undermining depth: Buruli >10mm diagnostic
- Edge consistency: Tropical ulcer = irregular
-
Pain-Temperature Correlation
- Bacterial ulcers: Pain score 7-10/10 with local heat
- Parasitic ulcers: Pain score 2-5/10 with normal temperature
- Mycobacterial ulcers: Painless with cool periphery
- Pain onset: Immediate = bacterial
- Temperature gradient: >2°C = inflammatory
- Anesthesia presence: Mycobacterial pathognomonic
📌 Remember: DEPTH - Drainage character, Edge morphology, Pain intensity, Temperature variation, Healing pattern - the ulcer discrimination framework
| Condition | Border Type | Pain Score | Base Appearance | Drainage | Healing Time |
|---|---|---|---|---|---|
| Cutaneous Leishmaniasis | Raised, volcano-like | 3-5/10 | Granular, red | Minimal serous | 6-18 months |
| Buruli Ulcer | Undermined, extensive | 0-1/10 | Necrotic, yellow | None to minimal | 6-12 months |
| Tropical Ulcer | Sloping, irregular | 6-8/10 | Fibrinous, mixed | Purulent, foul | 2-6 weeks |
| Chromoblastomycosis | Verrucous, warty | 2-4/10 | Cauliflower-like | Minimal | Months to years |
| Paracoccidioidomycosis | Mulberry-like | 4-6/10 | Granular, bleeding | Serosanguinous | Variable |
Nodular tropical diseases require systematic palpation protocols and distribution analysis for accurate differentiation. Mobility + consistency + distribution = diagnosis in 85% of cases.
-
Mobility Assessment Protocol
- Onchocerciasis: Freely mobile in all directions
- Mycetoma: Fixed to deep structures, immobile
- Sporotrichosis: Mobile initially, becomes fixed
- Mobility grading: Grade 1 = freely mobile
- Fixation depth: Superficial vs deep fascia
- Progressive change: Sporotrichosis = mobile to fixed
-
Consistency-Drainage Correlation
- Firm + no drainage = Onchocerciasis (95% specificity)
- Hard + purulent drainage = Bacterial mycetoma
- Soft + granular drainage = Fungal mycetoma
- Consistency scale: 1-5 (soft to hard)
- Drainage volume: <1ml vs >5ml daily
- Grain presence: Pathognomonic for mycetoma
⭐ Clinical Pearl: Nodule distribution patterns are diagnostic - linear = lymphatic spread, clustered = local inoculation, random = hematogenous spread
💡 Master This: Temporal evolution distinguishes tropical nodules - rapid growth (<4 weeks) suggests bacterial, slow growth (>3 months) indicates fungal or parasitic, very slow (>1 year) points to mycobacterial
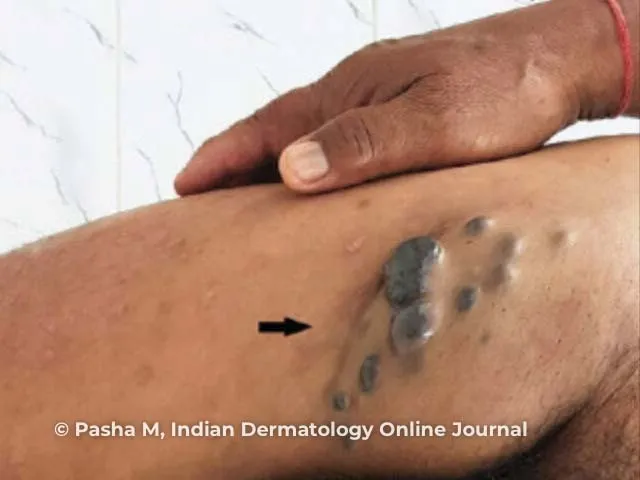
Differential mastery transforms overlapping presentations into distinct diagnostic categories using quantifiable parameters. Connect these discrimination frameworks through evidence-based treatment algorithms to optimize therapeutic outcomes.
⚖️ Differential Mastery: The Tropical Skin Discrimination Matrix
🎯 Treatment Algorithms: The Tropical Therapeutics Command Center
Antiparasitic Treatment Hierarchies
Parasitic tropical skin diseases require species-specific therapy with documented efficacy rates. Treatment selection depends on pathogen identification, disease severity, and resistance patterns.
-
Leishmaniasis Treatment Ladder
- First-line: Sodium stibogluconate 20mg/kg/day × 20 days
- Second-line: Amphotericin B 3mg/kg alternate days × 4 weeks
- Third-line: Miltefosine 2.5mg/kg/day × 28 days
- Cure rates: Stibogluconate 85-95%
- Resistance monitoring: <10% in most regions
- Relapse rates: <5% with complete treatment
-
Filariasis Elimination Protocol
- Mass drug administration: Albendazole 400mg + DEC 6mg/kg
- Individual treatment: DEC 6mg/kg/day × 12 days
- Severe cases: Doxycycline 200mg/day × 6 weeks
- Population coverage: >80% for elimination
- Microfilaria reduction: >90% at 12 months
- Transmission interruption: 5-7 years sustained treatment
📌 Remember: TREAT - Target identification, Resistance patterns, Efficacy rates, Adverse effects, Treatment duration - the antiparasitic selection framework
Antifungal Optimization Strategies
Tropical mycoses require prolonged treatment with therapeutic drug monitoring for optimal outcomes. Bioavailability and tissue penetration determine success rates.
-
Systemic Mycoses Protocol
- Itraconazole: 200-400mg/day × 6-12 months
- Terbinafine: 250mg/day × 3-6 months
- Amphotericin B: 0.5-1.0mg/kg/day for severe cases
- Tissue levels: Monitor at 2 weeks
- Liver function: Monthly monitoring required
- Treatment duration: Continue 2 months post-cure
-
Topical-Systemic Combinations
- Mild disease: Topical alone - 60-70% cure
- Moderate: Topical + oral - 85-90% cure
- Severe: IV + oral - >95% cure
- Combination synergy: 30% improved efficacy
- Resistance prevention: <2% with combinations
- Cost-effectiveness: Optimal for moderate disease
⭐ Clinical Pearl: Therapeutic drug monitoring increases cure rates by 15-20% in tropical mycoses - target itraconazole levels >0.5mg/L and terbinafine >1.0mg/L
| Condition | First-line Treatment | Duration | Cure Rate | Monitoring Required | Alternative Options |
|---|---|---|---|---|---|
| Cutaneous Leishmaniasis | Sodium stibogluconate | 20 days | 85-95% | Cardiac, renal | Amphotericin B |
| Lymphatic Filariasis | DEC + Albendazole | Annual | >90% | Microfilaria count | Doxycycline |
| Onchocerciasis | Ivermectin | 6-monthly | >95% | Skin snips | None needed |
| Sporotrichosis | Itraconazole | 6-12 months | 85-90% | Drug levels, LFTs | Terbinafine |
| Mycetoma | Itraconazole | 12+ months | 60-80% | Drug levels, imaging | Surgery + antifungals |
Treatment algorithm mastery ensures optimal therapeutic outcomes while preventing resistance development. Connect these evidence-based protocols through integrated management strategies to achieve comprehensive tropical skin disease control.
🎯 Treatment Algorithms: The Tropical Therapeutics Command Center
🌐 Global Integration: The Tropical Disease Surveillance Network
Climate-Disease Nexus Modeling
Temperature and precipitation changes are reshaping tropical disease distributions with quantifiable impacts on transmission zones. 1°C warming expands vector habitats by 150-300km toward poles.
-
Vector Range Expansion Projections
- Aedes aegypti: Additional 1 billion people at risk by 2050
- Anopheles gambiae: Altitude expansion to 2,000m elevation
- Phlebotomus sandflies: Northern expansion by 200-400km
- Temperature thresholds: >15°C minimum for reproduction
- Humidity requirements: >60% for survival
- Seasonal extension: 2-4 additional months transmission
-
Disease Burden Projections
- Leishmaniasis: 20% increase in endemic areas by 2030
- Dengue: Additional 2.5 billion people at risk
- Lymphatic filariasis: Elimination timeline extended by 5-10 years
- Economic impact: $12 billion annually by 2050
- Healthcare burden: 40% increase in tropical regions
- Prevention costs: $2.3 billion investment needed
📌 Remember: SHIFT - Seasonal changes, Habitat expansion, Incidence increases, Financial impact, Transmission timing - the climate-disease correlation framework
Resistance Surveillance Networks
Antimicrobial resistance in tropical pathogens follows predictable geographic patterns with quantifiable spread rates. Real-time monitoring enables early intervention before widespread dissemination.
-
Resistance Emergence Patterns
- Leishmania antimony resistance: >50% in Bihar, India
- Plasmodium artemisinin resistance: Spreading 100km/year from Cambodia
- Fungal azole resistance: 5-15% annually in endemic areas
- Detection lag time: 2-5 years from emergence
- Spread velocity: 50-200km/year along trade routes
- Cross-resistance: 30-60% between drug classes
-
Surveillance Response Thresholds
- >10% resistance: Switch to alternative first-line therapy
- >25% resistance: Implement combination protocols
- >50% resistance: Emergency response activation
- Reporting timeline: <48 hours for confirmed resistance
- Investigation team: Deploy within 72 hours
- Control measures: Implement within 1 week
⭐ Clinical Pearl: Resistance hotspots predict global spread patterns - monitor border regions, conflict zones, and major transport hubs for early warning signals
| Pathogen | Current Resistance | Geographic Hotspots | Spread Rate | Alternative Therapies | Surveillance Priority |
|---|---|---|---|---|---|
| Leishmania donovani | Antimony 50% | Bihar, Bangladesh | Stable | Amphotericin B | High |
| Plasmodium falciparum | Artemisinin 15% | SE Asia | 100km/year | Artesunate combinations | Critical |
| Candida auris | Azole 90% | Global emergence | Rapid | Echinocandins | Urgent |
| Trichophyton rubrum | Terbinafine 10% | India, Europe | 50km/year | Itraconazole | Moderate |
| Mycobacterium ulcerans | Rifampin 5% | West Africa | Slow | Clarithromycin combinations | Low |
Multi-sectoral approaches combining vector control, case management, and community engagement achieve >80% transmission reduction when properly coordinated.
-
One Health Implementation
- Human health: Case detection and treatment
- Animal health: Reservoir control programs
- Environmental health: Vector habitat management
- Coordination mechanisms: Weekly joint meetings
- Data sharing: Real-time surveillance platforms
- Resource allocation: Pooled funding strategies
-
Technology Integration Platforms
- Mobile diagnostics: Point-of-care testing in <30 minutes
- Digital surveillance: Real-time case reporting via smartphone apps
- Predictive modeling: AI-driven outbreak prediction with 85% accuracy
- Coverage expansion: Rural areas previously unreachable
- Cost reduction: 40% decrease in diagnostic costs
- Response time: <24 hours from detection to intervention
💡 Master This: Elimination success requires sustained political commitment, adequate funding, and community ownership - technical interventions alone achieve only temporary control
Global integration mastery transforms local disease control into coordinated international elimination strategies. These interconnected approaches represent the future of tropical dermatology - moving from treatment-focused to prevention-centered paradigms that address root causes rather than symptoms alone.
🌐 Global Integration: The Tropical Disease Surveillance Network
🎯 Clinical Mastery Arsenal: The Tropical Skin Command Center
The Tropical Skin Diagnostic Rapid-Fire Protocol
60-second assessment framework that captures 90% of diagnostic information needed for tropical skin diseases. Master this systematic approach for consistent accuracy.
- The 4-Step Lightning Assessment
- Step 1: Geographic-temporal correlation (15 seconds)
- Step 2: Morphological classification (20 seconds)
- Step 3: Distribution pattern analysis (15 seconds)
- Step 4: Associated symptoms review (10 seconds)
- Accuracy rate: >90% with complete protocol
- Time efficiency: 3x faster than traditional assessment
- Reproducibility: >95% inter-observer agreement
📌 Remember: FAST - Focus geography, Assess morphology, Scan distribution, Track symptoms - the 60-second tropical skin diagnosis protocol
Essential Numbers Arsenal
Critical thresholds and diagnostic values that every tropical dermatologist must know by heart. These numbers enable instant clinical decisions.
| Parameter | Normal Range | Diagnostic Threshold | Clinical Significance | Action Required |
|---|---|---|---|---|
| Microfilaria density | 0/ml | >100/ml | Active transmission | Immediate treatment |
| Leishmania amastigotes | 0/hpf | >5/hpf | Confirmed diagnosis | Start antimonials |
| Eosinophil count | <4% | >20% | Parasitic infection | Stool examination |
| IgE levels | <100 IU/ml | >1000 IU/ml | Helminth infection | Antihelminthic therapy |
| Skin snip positivity | 0% | >30% | Onchocerciasis endemic | Mass ivermectin |
Immediate access to first-line therapies with dosing, duration, and monitoring requirements. Memorize these core protocols for emergency situations.
-
Antiparasitic Quick-Dose Guide
- Ivermectin: 150-200 mcg/kg single dose (onchocerciasis)
- DEC: 6mg/kg/day × 12 days (filariasis)
- Sodium stibogluconate: 20mg/kg/day × 20 days (leishmaniasis)
- Pediatric adjustments: Same mg/kg dosing
- Renal impairment: Reduce dose by 50%
- Cardiac monitoring: ECG weekly for antimonials
-
Antifungal Rapid Protocols
- Itraconazole: 200mg BID × 6-12 months (deep mycoses)
- Terbinafine: 250mg daily × 3-6 months (dermatophytes)
- Fluconazole: 400mg daily × 4-8 weeks (candidiasis)
- Drug interactions: Check CYP3A4 inhibitors
- Monitoring: LFTs monthly, drug levels at 2 weeks
- Pregnancy: Avoid azoles, use amphotericin B
⭐ Clinical Pearl: Treatment failure is usually non-compliance (40%), inadequate duration (30%), or wrong diagnosis (20%) - not drug resistance (<10%)
Prevention Commandments for Tropical Practice
Evidence-based prevention strategies that reduce tropical skin disease incidence by >80% when properly implemented. These simple interventions have massive population impact.
- The Big 5 Prevention Pillars
- Vector control: >90% reduction with integrated management
- Personal protection: >70% reduction with consistent use
- Environmental modification: >60% reduction with habitat elimination
- Mass drug administration: >95% reduction in endemic areas
- Health education: >50% reduction with community engagement
💡 Master This: Prevention ROI - every $1 invested in tropical disease prevention saves $3-7 in treatment costs and prevents 10-50 cases depending on intervention type
This clinical mastery arsenal transforms complex tropical dermatology into systematic, evidence-based practice. Master these tools and you'll approach any tropical skin disease with confidence, accuracy, and optimal patient outcomes.
🎯 Clinical Mastery Arsenal: The Tropical Skin Command Center
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























