Definition & Pathogenesis - Patchy Puzzle Pieces
- Definition: Acquired, chronic depigmenting disorder characterized by the selective loss of functional melanocytes from the epidermis and, occasionally, hair follicles.
- Melanocytes: Neural crest-derived cells responsible for melanin production; primarily in skin (epidermal, follicular reserves), but also eye (uvea) and inner ear.
- Key Pathogenetic Theories:
- Autoimmune: Most accepted; T-cell (CD8+) mediated destruction of melanocytes.
- Neural: Neurochemical mediators (e.g., neuropeptides) damage melanocytes or inhibit melanin synthesis.
- Oxidative Stress: Accumulation of Reactive Oxygen Species (ROS) and ↓antioxidant defenses (e.g., catalase) damage melanocytes.
- Genetic: Polygenic; associations with HLA (e.g., HLA-DRB1*07) and immune-related genes.
- Melanocytorrhaphy: Defective melanocyte adhesion and chronic detachment leading to transepidermal loss.
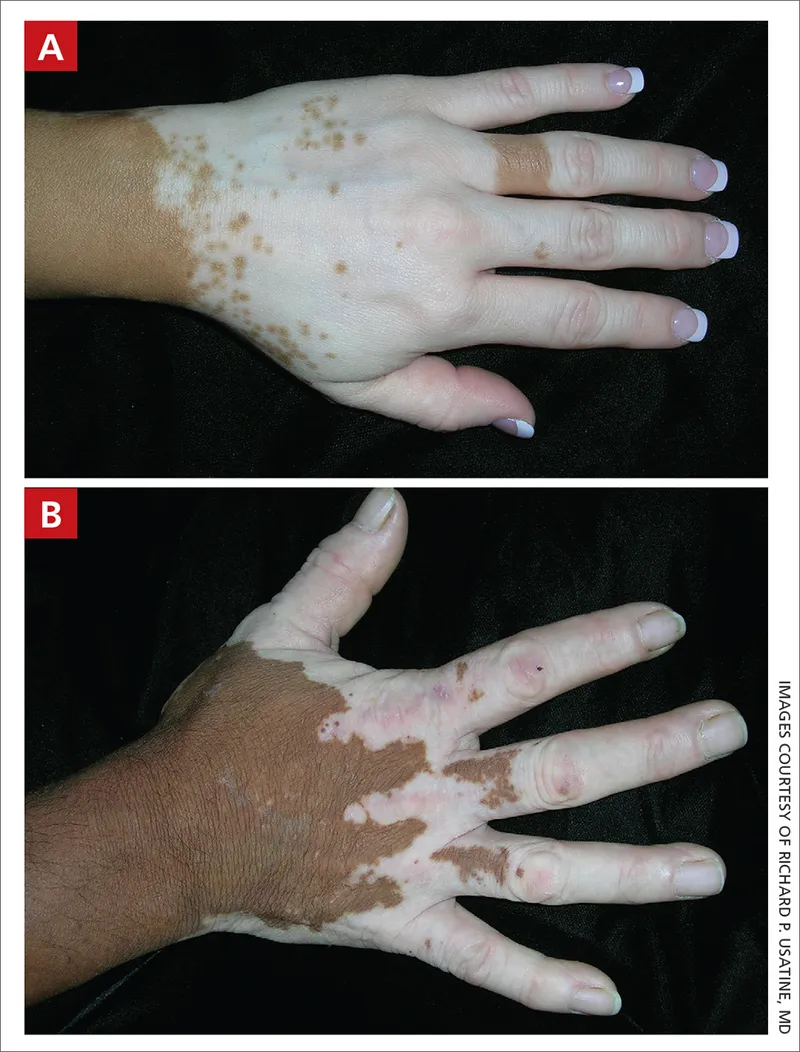
⭐ Koebner phenomenon (isomorphic response), the development of new vitiligo lesions at sites of skin trauma, is a common indicator of active disease progression and is seen in about 20-60% of patients.
Clinical Features & Types - Spot the Signs
- Types:
- Non-segmental (NSV): Most common; often symmetrical.
- Generalized: Widespread macules.
- Acrofacial: Lips, distal fingers/toes.
- Mucosal: Oral/genital mucosa.
- Universal: Affects >80% of body surface area.
- Segmental (SV): Unilateral, dermatomal; earlier onset, stable course.
- Mixed: Features of both NSV and SV.
- Non-segmental (NSV): Most common; often symmetrical.
- Morphology:
- Chalky/milky white, depigmented macules or patches.
- Well-demarcated borders.
- Trichrome vitiligo: Intermediate zone of hypopigmentation between normal and depigmented skin.
- Koebner phenomenon: Lesions at sites of trauma.
- Common Sites: Extensor surfaces (elbows, knees), periorificial areas (eyes, mouth, nostrils), hands, feet, genitals.
- Associated Autoimmune Conditions: Thyroid disease (Hashimoto’s, Graves’), alopecia areata, pernicious anemia, type 1 diabetes.

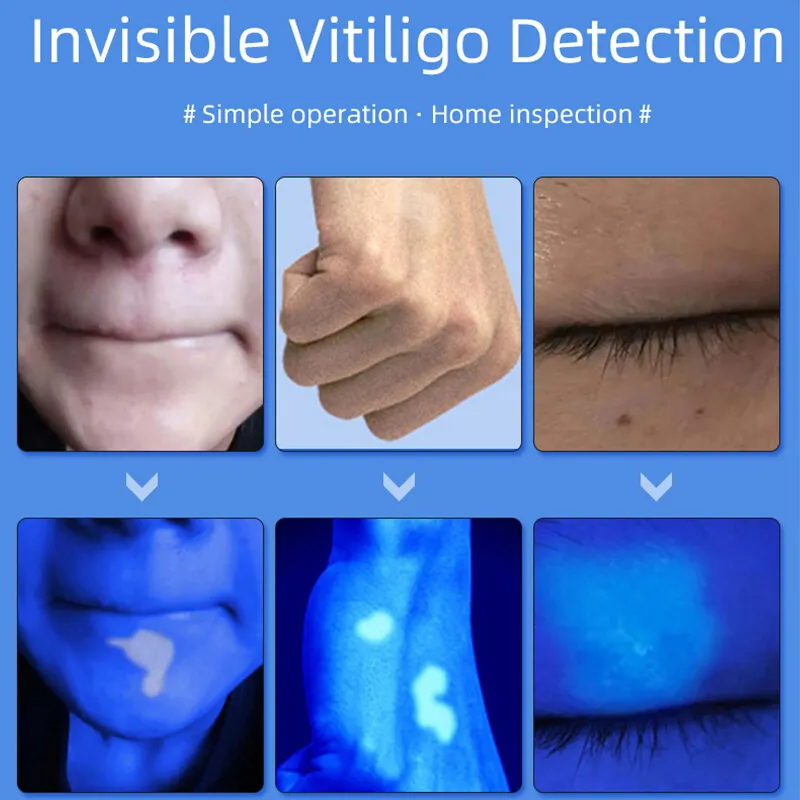
⭐ Wood's lamp examination (wavelength 365 nm) accentuates depigmented areas, appearing as bright blue-white fluorescence, especially useful in fair-skinned individuals where contrast is low under normal light.
Diagnosis & DDx - Confirming the Clues
- Clinical Diagnosis: Based on characteristic depigmented macules/patches.
- Wood's Lamp Examination:
- Accentuation of depigmentation (chalky white fluorescence).
- Helps identify subclinical/early lesions.
- Skin Biopsy (Rarely needed):
- Confirms absence of melanocytes.
- May show marginal lymphocytic infiltrate.
- Differential Diagnosis (DDx):
- Pityriasis alba
- Tinea versicolor (KOH: spaghetti & meatballs)
- Idiopathic guttate hypomelanosis
- Piebaldism (congenital, stable)
- Chemical leukoderma
- Leprosy (sensory loss)
⭐ Wood's lamp is crucial for detecting subtle lesions and assessing true extent, especially in fair-skinned individuals.
Vitiligo Management - Repigmenting Roadmap
Goals: Arrest progression, induce repigmentation.

- Medical Therapies:
- Topical: Corticosteroids (e.g., clobetasol propionate), calcineurin inhibitors (tacrolimus, pimecrolimus), JAK inhibitors (tofacitinib).
- Phototherapy: NB-UVB (311-313 nm), PUVA.
- Systemic: Corticosteroids (oral mini-pulse for active disease), JAK inhibitors.
- Surgical Therapies (for stable vitiligo):
- Autologous melanocyte transplant (MKTP), punch grafting, suction blister grafting.
- Depigmentation (extensive vitiligo >80% BSA):
- Monobenzyl ether of hydroquinone (MBEH).
- Always: Sunscreen use.
⭐ For generalized vitiligo, NB-UVB phototherapy (311-313 nm) is a first-line treatment, offering good efficacy and safety.
High‑Yield Points - ⚡ Biggest Takeaways
- Autoimmune destruction of melanocytes causes well-demarcated depigmented patches.
- Koebner phenomenon (new lesions at trauma sites) is frequently observed.
- Wood's lamp examination accentuates lesions, appearing as chalky white fluorescence.
- Strong association with other autoimmune diseases (e.g., thyroiditis, pernicious anemia).
- Segmental vitiligo follows dermatomes; non-segmental is more common and widespread.
- Mainstay treatments include topical corticosteroids, calcineurin inhibitors, and NB-UVB phototherapy.
- Surgical therapies like melanocyte transplantation are for stable, localized disease_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

