Intro to Child Pigment - Palette Basics
- Skin color primarily determined by melanin; other contributors: carotene, oxyhemoglobin, deoxyhemoglobin.
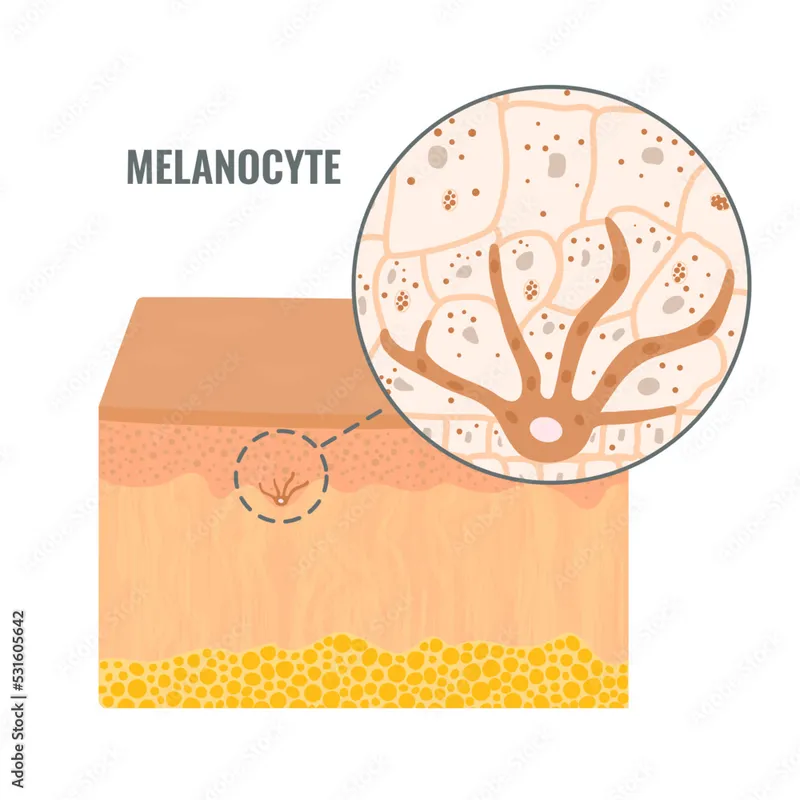
- Melanocytes: Neural crest-derived dendritic cells in epidermal basal layer, hair follicles, uvea. Synthesize melanin within melanosomes.
- Melanin types: Eumelanin (brown/black, photoprotective) & Pheomelanin (red/yellow, photosensitive). Their ratio dictates skin/hair phenotype.
- Synthesis: Tyrosine $ \xrightarrow{\text{Tyrosinase}} $ DOPA $ \xrightarrow{\text{Tyrosinase}} $ Dopaquinone $ \rightarrow $ Melanins.
- Regulation: Genetic factors, UV radiation (stimulates melanogenesis), Hormones (e.g., MSH, ACTH, estrogens).
⭐ Tyrosinase, a copper-containing enzyme, is the key rate-limiting enzyme in melanin biosynthesis pathway and a common target in pigmentary disorders research and treatment strategies for conditions like albinism or melasma where its activity is deficient or overactive respectively. This enzyme catalyzes the first two steps in melanin production: the hydroxylation of tyrosine to DOPA and the oxidation of DOPA to dopaquinone. Mutations in the TYR gene, which encodes tyrosinase, are the most common cause of oculocutaneous albinism type 1 (OCA1).
Hypopigmentary Disorders - Lighter Hues Lowdown
- Vitiligo: Acquired, autoimmune melanocyte loss. Well-demarcated, depigmented macules. Koebner (+). Wood's lamp: chalky white.
- Types: Segmental, Non-segmental.
- Pityriasis Alba: Common, ill-defined, hypopigmented, scaly patches. Face, neck, upper limbs. Post-inflammatory (eczema). Self-limiting.
- Albinism (Oculocutaneous - OCA): Congenital, AR. ↓/absent melanin (tyrosinase defects). Skin, hair, eye hypopigmentation. ↑ skin cancer risk. Nystagmus.
- 📌 OCA1 (Tyr-neg) vs OCA2 (Tyr-pos, P protein).
- Tuberous Sclerosis Complex (TSC): Ash leaf spots (≥3 diagnostic). Lance-ovate, hypopigmented macules. Wood's lamp enhances.
- Piebaldism: Congenital, AD (KIT gene). Stable, depigmented patches (forehead, central trunk, mid-extremities). White forelock (80-90%).
- Nevus Depigmentosus: Congenital, non-progressive, well-demarcated hypopigmented patch. Stable size/distribution. Normal melanocyte count, ↓ melanosomes.

⭐ Wood's lamp examination is crucial: Vitiligo fluoresces bright blue-white/chalky white, while ash leaf spots of TSC are accentuated. Pityriasis alba may show slight accentuation but not as intense as vitiligo.
Hyperpigmentary Disorders - Darker Tints Tour
- Café-au-Lait Macules (CALMs): Light brown, well-demarcated macules. If >6 lesions, each >5mm (prepubertal) or >15mm (postpubertal), suspect Neurofibromatosis Type 1 (NF-1).

- Becker's Nevus: Unilateral, sharply demarcated, hyperpigmented patch, often with hypertrichosis. Typically appears around puberty; androgen-dependent.
- Mongolian Spots (Congenital Dermal Melanocytosis): Blue-grey patches, commonly lumbosacral. Prevalent in Asian infants; usually fade spontaneously.
- Nevus of Ota/Ito: Bluish-grey pigmentation. Ota (CN V1/V2 distribution; risk of glaucoma), Ito (supraclavicular/deltoid region).
- Erythema Dyschromicum Perstans (Ashy Dermatosis): Asymptomatic, slowly progressive, slate-grey to blue-brown macules. Trunk, neck, upper extremities.
- Post-Inflammatory Hyperpigmentation (PIH): Acquired hypermelanosis following skin injury or inflammation. More common and persistent in darker skin types.
- Acanthosis Nigricans: Velvety, hyperpigmented plaques, typically in flexural areas (axillae, neck). Associated with insulin resistance, obesity.
⭐ Multiple Café-au-Lait Macules (>6 lesions, >5mm in prepubertal children or >15mm in postpubertal individuals) are a major diagnostic criterion for Neurofibromatosis Type 1 (NF-1).
Key Syndromes & Approach - Gene Spots & Strategy
-
Key Syndromes & Gene Spots:
- Neurofibromatosis-1 (NF1): ≥6 CALMs (>5mm prepubertal, >15mm postpubertal), axillary/inguinal freckling. Gene: NF1.
- Tuberous Sclerosis Complex (TSC): ≥3 Ash-leaf spots (hypopigmented macules), shagreen patch, facial angiofibromas. Genes: TSC1, TSC2.
- McCune-Albright Syndrome (MAS): CALMs (large, irregular "coast of Maine" border), polyostotic fibrous dysplasia, precocious puberty. Gene: GNAS.
- Waardenburg Syndrome (WS): White forelock, heterochromia iridis, dystopia canthorum, sensorineural hearing loss (SNHL). Genes: PAX3, MITF, SOX10.
- Piebaldism: Congenital stable white forelock & ventral depigmented patches. Gene: KIT.
-
Diagnostic & Management Strategy:
- Thorough history (family hx, onset) & cutaneous exam (Wood's lamp).
- Identify type: Hypo/depigmentation vs. Hyperpigmentation.
- Pattern: Localized vs. Generalized/diffuse.
- Systemic evaluation for syndromic features.
- Genetic counseling for heritable disorders.
- Sun protection is paramount.

⭐ NF1 diagnostic criteria: Two or more features required. CALMs are often the first sign.
High‑Yield Points - ⚡ Biggest Takeaways
- Neurofibromatosis-1: >6 Café-au-lait macules (CALMs) before puberty, axillary/inguinal freckling, Lisch nodules are key.
- Tuberous Sclerosis: Ash-leaf spots (hypopigmented, best seen with Wood's lamp), shagreen patch, facial angiofibromas.
- Piebaldism: Autosomal dominant, congenital stable depigmented patches with a white forelock; KIT gene mutation.
- Vitiligo: Acquired, progressive depigmentation due to melanocyte loss; strong autoimmune association.
- Oculocutaneous Albinism: Autosomal recessive, generalized hypopigmentation of skin, hair, eyes; ↑ risk of skin malignancies.
- Incontinentia Pigmenti: X-linked dominant, characteristic hyperpigmented streaks along Blaschko's lines in later stages_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

