Tungiasis Basics - Sandy Stowaways
- Definition: Ectoparasitic skin disease caused by penetration of female sand flea Tunga penetrans.
- Common Names: Jigger, chigoe flea, sand flea, nigua.
- Epidemiology:
- Distribution: Tropical/subtropical - Latin America, Caribbean, Sub-Saharan Africa, India.
- High-Risk: Poverty, rural areas, barefoot individuals, children, elderly.
- Seasonality: Peaks in dry season.
⭐ Exam Favourite: Tunga penetrans is the smallest known flea, measuring about 1 mm in length before engorgement with blood and eggs after burrowing into the skin of its host (often feet).
Meet the Menace - Tunga penetrans Profile
- Causative Agent: Tunga penetrans (jigger or sand flea).
- Smallest known flea; female is an obligate parasite.
- Morphology:
- Size: Approx. 1mm (unfed female).
- Appearance: Wingless, reddish-brown, laterally compressed.

- Life Cycle: Egg (on ground/soil) → Larva → Pupa → Adult.
- Impregnated female burrows into the host's epidermis (typically feet).
- Mode of Transmission: Direct contact with soil or sand contaminated with fleas.
⭐ The burrowed female Tunga penetrans undergoes massive abdominal hypertrophy (neosomy), swelling up to 2000 times her original volume as she produces eggs. This causes intense local inflammation and pain for the host.
Skin Invasion - Symptoms & Sequelae
- Mechanism: Female sand flea (Tunga penetrans) burrows into stratum granulosum, undergoes hypertrophy, and expels eggs.
- Common Sites: Feet (soles, periungual areas, interdigital spaces), hands.
- Clinical Progression & Symptoms:
- Complications:
- Secondary bacterial infections (cellulitis, abscess, lymphangitis, tetanus, gas gangrene).
- Severe inflammation, edema, ulceration.
- Nail dystrophy or loss.
- Auto-amputation of digits (chronic, severe cases).

⭐ Tetanus is a significant and preventable complication; ensure patient's immunization is up-to-date or administer prophylaxis, especially with multiple lesions or signs of superinfection.
Identifying Intruders - Diagnostic Clues
- Clinical Diagnosis: History of exposure in endemic areas; characteristic lesion (visible flea posterior/eggs).
- Key Signs:
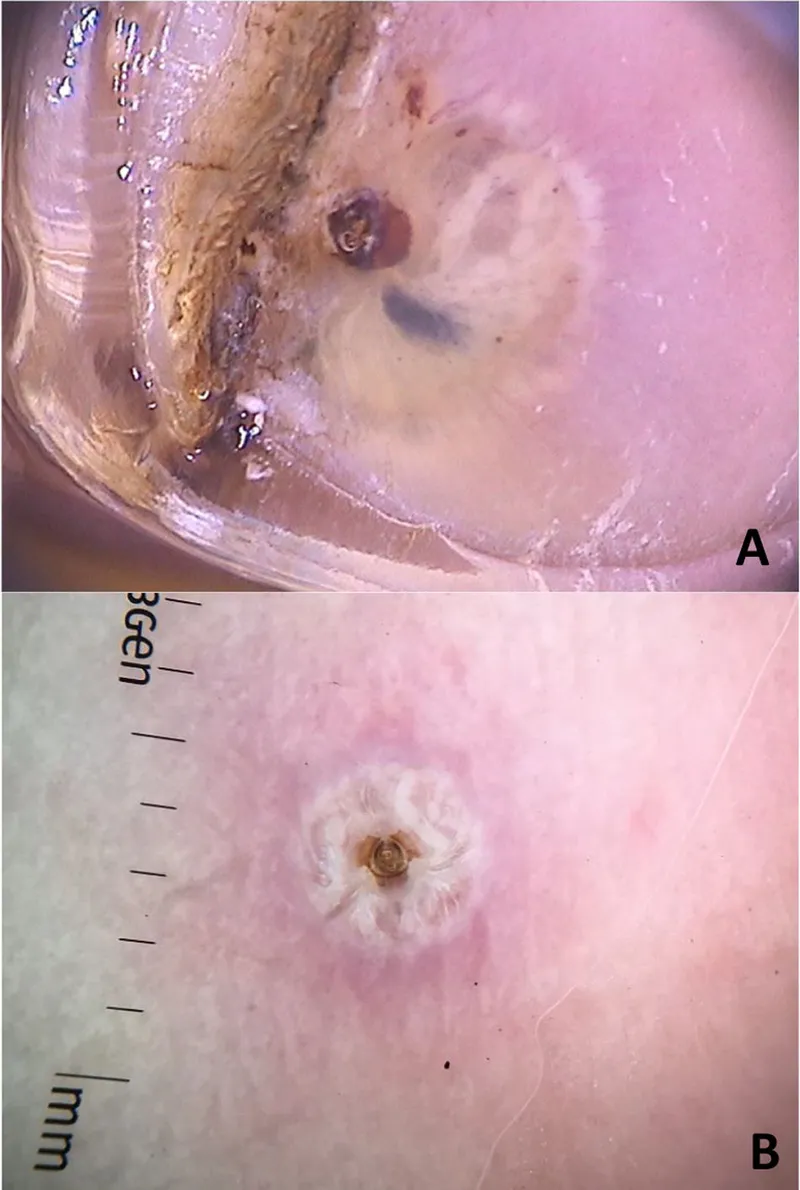
- Central black dot (flea's abdominal tip, spiracles, feces).
- Surrounding halo of hyperkeratosis/inflammation.
- Dermoscopy: May aid in visualizing the flea structure.
⭐ Diagnosis is primarily clinical, relying on the pathognomonic lesion appearance and exposure history.
- Biopsy: Rarely needed; shows flea parts within the epidermis.
- Differential Diagnosis: Myiasis, scabies, pyoderma, warts, foreign body granuloma, tick bite, cutaneous larva migrans.
Flea Eviction - Treatment & Prophylaxis
- Treatment of Choice:
- Surgical extraction: Sterile needle, complete removal.
- Post-extraction: Wound cleansing, topical antibiotic.
- Tetanus prophylaxis: Crucial.
- Adjunctive/Alternative Medical Management:
- Topical: Dimethicone-based (e.g., NYDA), ivermectin.
- Cryotherapy.
- Oral ivermectin (limited evidence).
- Complications Management: Antibiotics for secondary infections.
- Prevention (📌 "SEE JCC")
- Shoes: Regular use of closed footwear.
- Environmental control: Insecticides in homes/animal shelters.
- Education: Health education.
- Jojoba oil (in repellents like Zanzarin).
- Coconut oil (in repellents).
- Contact avoidance: With infested soil.
⭐ Exam Favourite: Tetanus prophylaxis is a critical component of tungiasis management post-flea extraction due to the risk of secondary infection with Clostridium tetani from contaminated soil or instruments during non-sterile removal attempts.
High-Yield Points - ⚡ Biggest Takeaways
- Caused by Tunga penetrans (sand flea).
- Presents as an itchy, painful papule with a central black dot (flea), typically on feet/toes.
- Key symptoms: intense pruritus, pain, and inflammation; secondary infection common.
- Complications include cellulitis, abscess, gangrene, and tetanus.
- Diagnosis is clinical, by visualizing the embedded flea.
- Treatment: Surgical extraction of the flea, wound care, tetanus prophylaxis.
- Prevention: Wearing closed footwear in endemic areas.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

